Lean Management Principles in Healthcare Operations
Healthcare systems worldwide face increasing pressure to enhance efficiency, reduce waste, and improve patient care outcomes. Lean management, originally developed in the manufacturing industry, has emerged as a powerful methodology for streamlining healthcare processes. By focusing on continuous improvement, eliminating inefficiencies, and optimizing workflows, Lean principles contribute to better healthcare delivery, cost-effectiveness, and patient satisfaction. Today, we have two esteemed panelists who bring extensive experience and deep insights into the implementation of Lean principles in healthcare.
1. Lean management is often associated with manufacturing. How do you see its adaptation to the complexities of healthcare operations, and what strategies have been most effective in its implementation?
Dr. KOH Hau-Tek: Lean management is traditionally linked to manufacturing, but its principles, such as eliminating waste, improving efficiency, and enhancing value are highly adaptable to a complex healthcare environment. The most effective strategy in Lean implementation is strong leadership commitment to foster a culture of continuous improvement, with leadership being key to shape and drive both company culture and successful change initiatives. The leaders can partake to be one of the architects of change but it is their full commitment to the vision that will set the tone for how the entire organization approaches and adapts to change.
2. From a medical practitioner’s perspective, how does Lean management impact clinical workflows, and what are the key challenges in ensuring that efficiency improvements do not compromise patient care quality?
Dr. Gaby Venera: Healthcare organizations often face operational inefficiencies, including long patient waiting times, workflow bottlenecks, resource misallocation, and administrative burdens. These inefficiencies reduce patient satisfaction, increase healthcare cost and employees' burn out. Lean management has been widely used in clinics to eliminate inefficiencies and streamline processes by removing non- value added activities in the workflows. The first challenge is how the improvement design and planning can be accepted by healthcare professionals and the second challenge is providing the software system. Data collection, monitoring and feedback systems are hard to get right, which are often poorly understood, poorly designed and poorly implemented. Systems need to be fit for purpose and avoid imposing excessive burdens or other unintended consequences, and staff need training on how to implement the improvement design and collect and interpret data.
3. Can you share real-world examples where Lean principles have successfully improved healthcare operations and patient outcomes?
Dr. KOH Hau-Tek: Lean management has been used in Jiahui International Hospital in Shanghai, China to improve efficiency and reduce costs. Through the use of technology, patients within 500 meters of the hospital or clinic will be automatically registered as detected by their GPS location. And upon entering the hospital, automated temperature checks and facial recognition with auto-registration, so that by the time they reach the outpatient clinics, the nurses and receptionists already expect the patients and bring them into the vital checks area. This leads to much shorter waiting times, and significantly reduces the need for large waiting rooms, optimising noth manpower and space.
Dr. Gaby Venera: A simple real-world example where we combine lean management with digital automation is in our medical check-up centers where we created medical check-up results automated email delivery systems. We designed and implemented a medical check-up workflow and identified areas of suboptimal use of resources and wastage. This identified the overuse of human resources which could be easily eliminated through automation. A digital automation system is then developed by sending it automatically to individual email addresses registered in the patient’s personal data. It can also detect if the emails were not sent correctly.
4. Leadership plays a crucial role in the success of Lean initiatives. What strategies do you recommend for fostering a culture of continuous improvement within healthcare organizations?
Dr. KOH Hau-Tek: Leaders and team managers are the backbone of change. There is 5C's framework of change leadership: Clarity, Communication, Collaboration, Culture, and Commitment.
- The leader needs clear communication with the board of directors and all the teams involved from before, during and after the intended change, to bring about a smooth transition. They also provide full support throughout the process to ease into the new normal.
- The manager identifies key employees in the respective and relevant teams, appoint them as champions for the change process, and provide them with support needed, but also to hold the key employees accountable throughout the process.
- The organization stays committed to the change and stays the course. There will always be reasons to change course and that will derail the process.
- Developing a learning culture within the organisation through action. With a culture of learning, employees will seek out areas of improvement, and when sufficiently engaged, will want to improve and also feedback on areas of continuous improvement.
5. Healthcare professionals often resist process changes. What approaches have you found effective in gaining acceptance and engagement for Lean initiatives?
Dr. Gaby Venera: Resistance to change is one of the most prevalent and difficult barriers to effective change management. To overcome change resistance, you need to understand its sources and address them effectively. Engaging middle managers and frontline staff in improvement efforts can be particularly challenging, as they already navigate multiple complex and competing clinical and organizational demands, often while dealing with staff shortages, limited resources, and equipment deficiencies. To reduce the change resistance, you need to communicate the vision, benefits, and rationale of the change clearly and empathetically. You also need to provide support, coaching, and feedback to help people cope with the emotional and cognitive aspects of change. It is also essential to engage stakeholders, particularly key influencers and champions, in both the planning and execution of the change. Trying to shift the norms and values before you have created the new way of operating will not work.
6. Value stream mapping and root cause analysis are fundamental Lean tools. How can these be applied effectively in healthcare to eliminate inefficiencies and optimize resource utilization?
Dr. KOH Hau-Tek: Value Stream Mapping (VSM) helps visualize the entire patient care process to identify bottlenecks and areas for improvement, while Root Cause Analysis (RCA) delves deeper into specific problems to understand their underlying causes, allowing healthcare organizations to implement targeted solutions, eliminate inefficiencies, and optimize resource utilization by pinpointing areas for process changes and preventing future issues.
Dr. Gaby Venera: The initial step in implementing Value Stream Mapping (VSM) is to establish the project's scope and purpose, which is determining the specific process or service to be mapped, defining its boundaries, identifying inputs and outputs, and setting clear goals and objectives. The next step involves gathering data and insights on the current state of the process or service. This requires collecting both quantitative and qualitative information, including cycle times, wait times, defect rates, inventory levels, staff satisfaction, and patient feedback. Various methods, such as observations, interviews, surveys, document analysis, and performance metrics, can be used to obtain this data. The third step is to create a visual representation of the current state map using symbols and icons to depict the flow of materials and information. The fourth step involves analyzing this map to identify areas for improvement. This includes calculating key value stream metrics, such as value-added time, non-value-added time, lead time, cycle time, throughput, and overall efficiency. On the fourth step, analyze the map with Root Cause Analysis ((RCA) to dig deeper into the root cause of delays, errors, or resource wastage.
7. In cost-sensitive healthcare environments, how can Lean principles help in balancing cost efficiency with high-quality patient care?
Dr. KOH Hau-Tek: Lean management is proven able to boost “customer happiness” while raising profits. These are some areas that applying Lean principles to balance cost-efficiency and high-quality patient care:
- Healthcare organizations can potentially lower their inventory levels. Inventory represents tied-up capital and incurs storage expenses for a business. Various factors contribute to inventory waste, such as excessive supplies and medications, surplus equipment, redundant data, and stockpiles of pre-printed forms. Additionally, maintaining large inventories locks up cash and adversely affects cashflow, increases the likelihood of financial losses due to theft or the expiration of medical consumables. An optimal inventory based on Lean principles allows the healthcare organisation to re-channel cashflow and funding to direct patient care areas.
- Defective wastage includes issues such as avoidable re-admissions to hospitals, medication or surgical errors, blood clots (deep venous thrombosis DVTs and Pulmonary embolism PE), hospital acquired infections, and inaccurate or incomplete medical records — all of which stem from healthcare-related defects and deficits.
8. What are some key performance indicators (KPIs) that healthcare institutions should monitor to assess the success of Lean management implementation?
Dr. Gaby Venera: One of the main goals pursued with the Lean management implementation is to improve some Key Performance Indicators (KPI) of the organization. We can group the KPI into three main pillars:
- Operational indicators : clinical quality, cost reduction, patient safety, organizational responsiveness, lead time, delivery performance, process time, inventory level, equipment performance, reducing delays, error rate, service quality and patient satisfaction.
- Environmental indicators: waste reduction, energy consumption, resource reduction, carbon footprint, carbon value efficiency and fossil fuel reserve emissions.
- Social indicators: employee well-being, work–life balance, employee satisfaction, work accidents, turnover rate, etc.
9. Digital transformation is reshaping healthcare. How do you see automation and technology complementing Lean methodologies in achieving operational excellence?
Dr. KOH Hau-Tek: Automation and technology significantly complement Lean methodologies, which help data driven decision making, improve process flow with process mapping and visualization, quality check and inventory management by automated task execution and real-time monitoring and feedback, ease the collaboration and communication with digital platforms. Examples of specific technologies that align with Lean methodologies are Robotic Process Automation (RPA). RPA brings in the power of automation, using software bots to take over repetitive, rule-based tasks with speed and precision.
Dr. Gaby Venera: From my perspective, Lean methodologies will be enhanced by integrating automation digital tools and technologies, whereas we are capable of achieving higher levels of operational excellence. Lean 4.0, a fusion of lean manufacturing and digital technologies, is a powerful tool for implementing Industry 4.0. There are several literature and studies regarding Lean 4.0 for Healthcare by now to evaluate the impact of Lean 4.0 principles in Healthcare. Lean 4.0 meets the growing demand in healthcare for enhanced patient care quality and operational efficiency by incorporating advanced digital technologies such as IoT, AI, and data analytics. This integration streamlines workflows, minimizes waste, and supports more effective decision-making. Here are primary supportive technologies of lean 4.0:
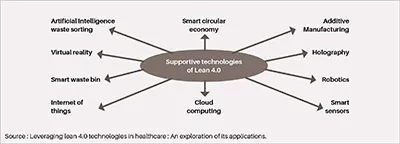
Source : Leveraging lean 4.0 technologies in healthcare : An exploration of its applications.
10. One major misconception about Lean is that it only focuses on cutting costs. How do you address this misconception when introducing Lean principles in healthcare settings?
Dr. KOH Hau-Tek: Indeed, many people see Lean as simply removing wasteful steps, which makes it seem like a cost-cutting measure. In reality, cost reduction is only a byproduct of Lean principles, not the main focus. The real goal is to improve efficiency by streamlining processes, reducing human error, and ensuring a faster and higher quality response to patient needs. This leads to enhanced resource utilization and, ultimately, a better experience for patients. Through eliminating inefficiencies, hospitals typically create smoother operations, reduce delays, and improve overall service quality, leading to better patient outcomes, and not just financial savings.
11. Interdisciplinary collaboration is essential for Lean success. How can Lean methodologies foster better teamwork among healthcare professionals?
Dr. Gaby Venera: Lean methodologies foster a culture of continuous improvement, transparency, and shared responsibility among the diverse range of healthcare professionals. One key principle of Lean is breaking down silos by encouraging cross-functional collaboration. Instead of departments operating in isolation, Lean promotes open communication and teamwork, ensuring that doctors, nurses, administrative staff, and other healthcare professionals work together seamlessly to identify inefficiencies and enhance patient care.
12. Sustainability is a major concern in Lean implementation. What measures can healthcare organizations take to ensure that Lean improvements are sustained long-term?
Dr. KOH Hau-Tek: To sustain Lean improvements long-term, healthcare organizations can:
• Foster a culture of continuous improvement: Regularly review performance metrics, audit processes, and implement small-scale improvement projects.
• Train staff: Provide comprehensive training programs to help staff identify and address inefficiencies.
• Establish standardized processes: Create consistent procedures to improve efficiency and identify opportunities for improvement.
• Encourage a growth mindset: Create an environment where learning and development are valued.
Dr. Gaby Venera: To achieve sustainable change, quality improvement initiatives must become the new way of working rather than something added on to routine clinical care. There are some basic strategic ways to maintain Lean implementation in operational daily activities, such as developing clear Standard Operating Procedures (SOPs), regularly updating workflow to reflect improvements, and implementing Key Performance Indicators (KPIs) to track the impact of Lean improvements. You can also take measures on employee satisfaction surveys to see the staff engagement in implementing the Lean initiatives. Such activities still need to be supported by sufficient resources, leadership support, data infrastructure, and team motivation.
13. Given your experience, what common mistakes do healthcare organizations make when trying to implement Lean, and how can they be avoided?
Dr. KOH Hau-Tek: From my experience, there are some mistakes while trying to implement Lean methodologies such as:
- Inconsistent commitment to performance improvement by the leadership. On many occasions, there is a change of leader every 3 to 5 years with the result that the Lean methodology cannot be implemented sustainably. To overcome this challenge, one will need to embed Lean into the organizational culture and values, create a dedicated Lean team and structure, provide ongoing coaching and mentoring, and celebrate and share the successes and lessons learned.
- There will always be resistances to change from various stakeholders, such as staff, managers, patients, and regulators. To overcome this challenge, one will need to communicate the vision, strategies, benefits and goals of Lean clearly and frequently, involve and empower the frontline workers, thereby creating a culture of continuous improvement, while providing adequate training and support.
14. Looking ahead, what future trends do you foresee in Lean healthcare management, and how should organizations prepare for these changes?
Dr. Gaby Venera: Lean healthcare management will become increasingly integrated with digital technology such as automation, artificial intelligence (AI), and machine learning (ML). This integration will greatly aid operational simplification, data analysis, and problem-solving. Lean principles will leverage the use of technology such as digital platforms, automation and AI. AI-driven predictive analytics will help identify inefficiencies, reduce waiting times, and improve resource allocation. Digital platforms, such as electronic health records (EHRs) and automation in administrative tasks, will further streamline operations, reducing the burden on healthcare workers. To prepare for these changes, healthcare organisations need to establish a clear vision, conduct current state assessment, build cross-functional teams, standardize lean pilot projects, and invest in lean training.
On behalf of AsianHHM Magazine, I extend my heartfelt thanks to Dr. Koh Hau-Tek and Dr. Gaby Venera for sharing their expertise and experiences with us. Your insights have been incredibly valuable in understanding the impact of Lean management in healthcare.
Thank you!




