
Healthcare providers lag behind other industries as far as transformation to customer-driven or customer-focussed organisation is concerned. For this to happen, the customer needs to be equipped with information about products and services, which in turn necessitates collaboration along healthcare continuum.
During the last decade we have seen significant efficiency gains in many industries – specifically in industries such as manufacturing, automotive, trading etc. Processes have been optimised and streamlined within enterprises, as also significantly across enterprises. Costs have been reduced through closer collaboration with suppliers. Customer service has improved, for example, through provision of information, access to products and services any time and anywhere.
The driving force of this change is competition, which has been created by the consumer, who is shopping for the best price and best quality for almost every product or service. This has forced enterprises to reduce costs while improving services, and it has resulted in more intelligent business processes and improved business models. Today, flexibility, adaptability and speed of change are the key for enterprises to survive in the increasingly competitive environment.
All these changes have been enabled by the increasing use of Information Technology. In fact, many of the innovations wouldn’t have been possible without a strong IT support. IT has become strategic in enterprises, enabling efficiency through standardisation, and providing the flexibility to accelerate innovation.
In healthcare, we have seen great innovations and significant improvement in the healthcare product arena. The increase in life expectancy is an achievement which, to a high extent, comes from improved medicines. It is very characteristic that a majority of the change has happened in ancillary departments, but not in core processes that directly face the healthcare customers. Little has been changed in the way healthcare is approached and delivered. For example, little attention is being paid to prevention, which in other quality-critical industries such as the airline industry, is fundamental to do business.
What is the reason for the lack of change and transformation in healthcare? By nature, healthcare in terms of diagnostics and treatment is something people need and nothing people want. Today in most of the healthcare systems, health insurers or the government are covering the majority of the cost, so that patients do not really look at costs or better prices. Due to lack of incentives, individual stakeholders such as provider organisations, insurers or pharmaceutical companies have not driven cross-organisational change. The patient today is not in a strong enough position to drive changes. This is mainly because the patient does not have the necessary information and understanding to assess, for instance, whether a service or a treatment is good or bad, whether there are alternatives and what a best choice can be. This is very different from other industries where product information is widely available that allows to assess quality and go for the best alternative. Through making more information available, the patient first needs to be enabled to behave and act as a consumer. In some areas, where the insurance system has cut funding and where significant co-payments need to be made by patients, a consumer-oriented environment has developed. For example, insurance coverage for eyeglasses has been significantly limited which in turn has opened a competitive market where prices have fallen far below the traditional levels. But consumerism, a key market force in many other industries, so far has had limited effect in healthcare.
 More significantly, healthcare faces major challenges which have put its affordability and sustainability at significant risk. Key challenges are ageing population, quality issues, increased cost and skill shortage (Figure 1).
More significantly, healthcare faces major challenges which have put its affordability and sustainability at significant risk. Key challenges are ageing population, quality issues, increased cost and skill shortage (Figure 1).
One impact of these challenges is that our daily life is more affected than it has been before. While healthcare in general has been very event-driven, so that the patient has had to deal with the health system mainly when a disease had to be cured, the increase of chronic diseases, for example, makes healthcare much more home bound and affecting our daily life.
One of the impacts of an ageing population is that elderly people living alone require more long-term care and a continuous services support, less an event-based care.
The cost pressure has started to lead to more cost-effective models, e.g. we see more healthcare services being moved from inpatient to outpatient and from outpatient to home. So the environment where healthcare delivery is taking place becomes increasingly consumer-driven. In addition, reduced insurance coverage leads to more awareness and shopping attitude of the patients.
The discussion around increasing number and influence of diseases such as obesity, diabetes and back pain causes recognition in the population that we all can individually influence health, which creates a demand for more and better information.
These examples indicate that the health system needs to be patient-centric in the future. A patient-centric system that is designed to provide more and better information and high quality services will require true collaboration between all stakeholders, collectively using and sharing knowledge and information.
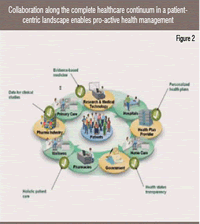 As a first step, provider collaboration is the key, allowing sharing of patient information not only between hospitals and primary care providers, but also with pharmacies. This collaboration should also include other and new providers that will enter the market such as home health organisations, disease management and wellness companies.
As a first step, provider collaboration is the key, allowing sharing of patient information not only between hospitals and primary care providers, but also with pharmacies. This collaboration should also include other and new providers that will enter the market such as home health organisations, disease management and wellness companies.
Collaboration along the healthcare continuum places the patient at the centre of this ecosystem, creating what we call a patient-centric landscape (Figure 2). Providing patients access to information that is available from all of these sources enables them to improve the decisions they make concerning their health and their lifestyle.
Further down the road, more informed patients will wield more power to make the health system work in the interest of the patients themselves.
Patient advocacy groups will support individual patients in getting their interests respected.
We also believe that there will be an increasing need to support the patients in understanding and handling the increasing information flow they confront. 'Health information brokers' will assist patients in making informed choices and decisions to better manage their own health.
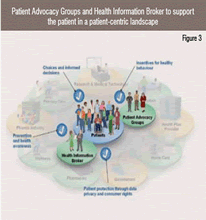 Incentives for healthy behaviour and healthy lifestyle from the payer community will increase patient interest in prevention and health awareness and in turn lead to a reduction of overall healthcare cost.
Incentives for healthy behaviour and healthy lifestyle from the payer community will increase patient interest in prevention and health awareness and in turn lead to a reduction of overall healthcare cost.
Since health data is particularly sensitive information, a legislation framework will be required that enables information exchange while protecting patient privacy and honoring the consumer rights. (Figure 3).

In summary, a collaborative healthcare network that places the patient at the centre of the health system enables the transformation from a passive patient to an informed consumer who is able to select wellness maintenance and treatment from a collaborative global healthcare community that provides personalised, evidence-based care (Figure 4). The patient, in fact, may become the owner of his data and decide about its distribution and use.
The transformation creates space for new or enhanced business models in healthcare. Examples for that are:
Summary
Consumerism has driven transformation and innovation in industries. Healthcare—despite significant improvement in the healthcare product—has seen limited transformation in the way it is approached and delivered. However, major challenges put the affordability and sustainability at risk. Collaboration and patient-centricity will make information more easily available and understandable, change the patients’ behaviour and give patients wider choice. The passive patient will be transformed to an informed consumer who is able to select wellness maintenance and treatment from a collaborative global healthcare community that provides personalised, evidence-based care.