
Medical tourism has played a catalytic role in making the Asian hospital strive for world-class quality standards.
The fact that medical tourism in Asia is happening, is no longer news. But prediction of its huge growth potential certainly is. Abacus International, a UK-based healthcare consultancy believes that the lure of low-cost, high quality healthcare in Asia will attract more than 1.3 million tourists a year to the key locations – Thailand, Singapore, India, South Korea and Malaysia. The medical tourism market is expected to be worth US$ 4 billion by 2012.
Rising healthcare costs in the US have forced the un-insured and under-insured patients to look at cheaper healthcare alternatives outside the US. But while high costs have been an important driver, the factor that has actually pushed the patients to undertake the long journey is that the hospitals in Asia have made an effort to match the quality standards that exist in the US and other western countries. They did so by striving to achieve the global accreditations like Joint Commission International (JCI). “An accreditation is a way to distinguish a hospital,” says Anne Rooney, Executive Director of International Services at JCI.
However, the importance of international accreditations to Asian hospitals goes far beyond just attracting foreign tourists. Better quality of healthcare and higher standards of patient safety help the hospitals to give the best treatment to a patient – irrespective of nationality - in the least possible time and with minimal wastage and lesser medical errors. While for the patients this means better treatment, for hospitals it is reduced wastage and lower costs in the long run. With accreditations, quality no longer remains the job of a few but it gets woven into the fabric of function involving all processes and people to pursue the same goal.
Accreditations - Reshaping Asian healthcare
Healthcare in Asia has emerged as a major focus area, with many nations recovering from the Asian Crisis as also the increasing prosperity China and India have begun to experience as a result of their policy reforms. There is a greater need to revamp the healthcare systems for better quality of healthcare. Attempts are on to benchmark with the best globally. India established the National Association Board for Hospitals and Health Service Providers (NABH) for accreditation of hospitals in the country recently. Absence of such standards always put the patients at risk. A survey by the World Health Organization (WHO) found the incidence of hospital- acquired infections to be highest in the Southeast Asian region at 10%, only marginally behind the Eastern Mediterranean region at 11.8%, which topped the list.
But there has been a gradual increase in the awareness regarding the importance of quality, thanks mainly to the increasing role of private players in the sector, especially in countries like India and China, where private sector hospitals have aggressively pursued accreditation. Medical tourism has played a catalytic role in making the Asian hospitals strive for world-class quality standards. Despite accreditations being a voluntary process, the competition to attract foreign tourists has been driving hospitals towards them. This of course is good news for domestic patients as well since they will be able to access the best healthcare without having to travel a lot.
Among the various international accreditations available, the one awarded by JCI, the international arm of the US-based accreditation body Joint Commission on Accreditation for Healthcare Organisations (JCAHO), has become very popular. High standards, wide scope and rigorous process of evaluation have made JCI accreditation a ‘gold standard’ in hospital accreditation. Already, as many as 30 Asian hospitals have got themselves accredited. And this number is only going up. While Singapore leads the Asian pack with 11 accredited hospitals, India, so far has 5 accredited hospitals with a few others preparing for it.
The other option that could soon be available for hospitals is the NIAHO- ISO certification developed by the TUVHS America. This program combines two independent sets of standards — ISO 9001 Quality Management standards and Hospital Conditions and Participation standards set by the Medicare program in the US. This new system has a wider scope than ISO 9001:2000 certification, which focuses largely on the administrative processes. However, it is yet to receive the final approval from the Centers for Medicare and Medicaid Services (CMS) of the US. Only then it will be able to accredit hospitals internationally.
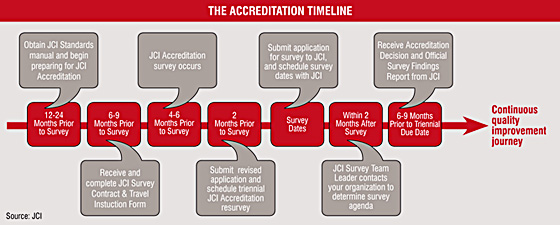
 The accreditation process
The accreditation process
The accreditation process For any hospital, the accreditation process represents bringing about a significant change in the way it functions. A comprehensive accreditation, such as that of JCI, needs to be implemented organization-wide, with the involvement of all the employees who take part in the patient’s journey from admission to discharge. In JCI, there are 565 standards divided into 197 core standards that must be met to achieve accreditation and 368 other standards that lead organisations to best practice levels. These standards are further divided into 1033 measurable parameters, which focus on aspects such as patient safety, patient rights, facilities, and physicians’ credentials besides policies and procedures of the organisation. To get accredited a hospital will have to fully meet most of these parameters and the remaining ones at least partially. Singapore’s National Health Centre (NHC), which got accredited in November 2005, met 1013 of the 1033 parameters successfully. The JCI accreditation is valid for 3 years and has to be renewed on a regular basis.
 The accreditation process typically lasts for about 2 years and involves two surveys by a team of consultants from JCI who also educate the hospital staff about various standards and their implementation. Here, the role of the top management becomes very crucial since it is their commitment that in turn influences the commitment of the whole organization. “It takes strong commitment from the top management” says Rooney and adds that the point-of-care staff, nursing staff, physicians and other employees of the hospitals too play a crucial role, as they have to adapt to a whole new way of functioning.
The accreditation process typically lasts for about 2 years and involves two surveys by a team of consultants from JCI who also educate the hospital staff about various standards and their implementation. Here, the role of the top management becomes very crucial since it is their commitment that in turn influences the commitment of the whole organization. “It takes strong commitment from the top management” says Rooney and adds that the point-of-care staff, nursing staff, physicians and other employees of the hospitals too play a crucial role, as they have to adapt to a whole new way of functioning.
The benefits are multi-fold. Both the healthcare provider and customer stand to gain if an organization complies with the standards. The benefits that ensue accreditations include better care for the patients, a customer-centric approach, improved branding as a result of increased confidence within the community, high employee morale and continuous monitoring of standards. Over a period of time the hospital would experience cost reductions as efficiency go up and more is achieved through less effort. Medical errors that cost hospitals thousands of dollars every year could be reduced as well. The final beneficiaries would be the patients since the new processes would be designed to meet their requirements and they have access to the best treatment. Says Rooney, “It’s interesting to note that some organizations have reduced medication errors by almost 75% to 80%. That obviously translates into a better patient experience.” Further, as processes get streamlined and designed around the patient needs, there is also a better chance for the hospital to provide evidence-based medicine to their patients.
Implementing the exacting standards of accreditation is usually a tough task to begin with. With so many standards to deal with, there is a need for meticulous planning and thorough implementation, which involves active participation of all the employees. As the process aims to influence the functioning of the organisation itself, change management – the process of generating a buyin by all, attains utmost importance prior to implementation. “Organizations that do this well really get to see a huge difference in the way they manage their hospitals”, claims Rooney.
Affordability
While the benefits of international accreditation are quite attractive, the fact is that accreditations such as JCI’s could be very expensive for a majority of medium-to-smaller hospitals in the region. A JCI accreditation would cost a hospital approximately US$ 100,000 and this does not include the expenses incurred for upgrading its facilities. The Apollo Indraprastha Hospital in New Delhi, India – first hospital in India to get the JCI accreditation – spent close to Rs. 30 crore (US$ 600,000 approximately) to upgrade its facilities. Medium-sized hospitals may not have such financial muscle!
While this being the limitation, accreditations also give rise to another possibility – national level accreditations with standards designed on the lines of international accreditations and customized to the needs of the local hospitals. In this scenario, the cost tends to come down significantly. The NABH could perform this very function helping smaller hospitals improve quality of healthcare and patient safety without having to spend huge amounts of money. While this may or may not result in them being able to attract international patients, it would certainly help in improving the quality of care in the hospitals.
The future
With an opportunity worth US$ 4 billion around, competition for medical tourists is bound to heat up and more hospitals are likely to queue up for international accreditations.
Accreditation organisations would have to work closely with the governments of various Asian countries to make this happen lest the world-class healthcare facilities would be confined only to a small portion of the population. As more hospitals start acquiring accreditations, domestic patients too would prefer to opt the accredited hospitals for treatment. This scenario will eventually push a general move towards improvement in quality of care. The peerpressure is two-fold – those who can afford accreditations start drawing blueprint for the same whereas those who cannot start learning about how to improve the status quo. This sort of a trend is already evident. “A recently held five-day practicum at Singapore was fully booked about six weeks in advance! This shows that there is a very strong interest in education about quality standards in Asia,” points Rooney.
To be successful, the hospitals that are gearing up to acquire accreditations, would do well to remember what Phillip Crosby, initiator of the Zero Defect concept said, “It (quality) has to be the fabric of the organisation, not part of the fabric.”