
The use of e-health can positively impact doctor-patient relationship promoting the mutual participation model of medicine, which implies that, e-health can promote a shared responsibility in decision making and problem solving.
Health systems around the world are facing numerous challenges, including the rapid increase in the prevalence of certain chronic diseases, limited funds and the pressure of an ever-ageing population. The shortage of health professionals to provide essential services is an important issue which both developed and developing countries are struggling to cope with. The rising costs of healthcare makes the situation even more complicated. Governments and international organisations worldwide are seeking solutions. Among others, e-health has been identified as one such solution that may help alleviate some of the challenges described.
In general terms, e-health may be used to describe the delivery of healthcare and exchange of healthcare information across distances using Information and Communication Technologies (ICT). Synonymous with e-health, other terms such as telemedicine, telehealth and mobile health are often used interchangeably. Despite the high expectations raised in the early 1990s, e-health has not been widely adopted and integrated as a mainstream service internationally. Unlike the use of ‘e methods’ in other spheres of the human society, such as online banking and online shopping—the health sector has been slow to adopt e-health. Nonetheless, hope for e-health to play its role is still there. A number of governments have implemented national e-health strategies. National initiatives such as National e-Health Transition Authority (Australia), the Health and Human Services (United States) and the NHS Modernisation Program (United Kingdom) can be few such examples. It has been recognised that the use of online communication techniques may be the key to improving quality, safety and patient outcomes.
In principle, e-health can be categorised as real-time and store-and-forward (pre-recorded). A common example of a real-time e-health application is communication via telephone. The use of the telephone has become commonplace around the world and we can tend to forget the value of it. Videoconferencing is another example—however much more expensive and generally less accessible than telephone services. Alternatively, e-health can be achieved using pre-recorded techniques, for example, the ordinary email. Whilst considered a relatively inexpensive form of e-health, this modality gives participants the opportunity to access information and communicate at their own convenience.
e-Health can be used for clinical, educational and administrative purposes. For example, the access of clinical data at distance can be useful for diagnoses and making important decisions regarding patient management. The growing use of technology-enhanced learning (e-learning) in medical/health education is a good example of e-health for educational purposes. In terms of administrative value of e-health, studies have shown that the use of electronic tools and medium (for example, computers, PDAs, Internet) can ease the administrative process in healthcare settings.
It may be argued that the use of e-health can positively impact doctor-patient relationship promoting the mutual participation model of medicine. This means e-health can promote a shared responsibility in decision making and problem solving.
In Australia, the integration of electronic technologies in routine clinical practice has been most prominent in the field of general practice. A recent survey reported by the Australian Medical Association (AMA) indicates that a well over 90% of the Australian general practitioners are utilizing computer technologies such as electronic prescribing and communications systems. Another area where e-health has been making some progress is the use of the Internet as a source of health information. A number of web-based health information sites are growing rapidly, and so too are the number of respective users.
Telepaediatrics
One of the successful e-health projects reported in the literature is the telepaediatric service in Queensland. The service commenced in November 2000 as a research trial through the University of Queensland’s Centre for Online Health (COH) in collaboration with the Royal Children’s Hospital (RCH) in Brisbane, and in time has emerged as a routine service. The telepaediatric service provides specialist consultations to children and their families living in rural and remote areas of Queensland. About 90% of telepaediatric consultations provided through the service are done via videoconference. More than 5000 consultations have been conducted since the service began, benefiting thousands of families statewide. Specialists at the RCH are now using this service to provide consultations to children who otherwise would have to travel hundred or thousands of kilometres to the specialist hospital. Paediatric sub-specialities offered by the telepaediatric service include post-acute burns care, cardiology, diabetes, neurology, oncology, orthopaedics, psychiatry and surgery. Both patients and providers have reported high levels of satisfaction with the service. Routine telepaediatric clinics are now scheduled 12 months in advance and managed in a very similar way to the conventional outpatient service.
An important factor in the success of the telepaediatric service is the unique referral model developed by the research team. Firstly, a centralised referral centre has been developed which gives selected regional hospitals direct access to a telepaediatric coordinator via a dedicated toll-free number. Staff in regional hospitals could easily make a referral by contacting the service instead of automatically sending patients to Brisbane to see the specialist in person.
Once a referral is made to the telepaediatric service, a response is guaranteed within 24hrs. Telepaediatric coordinators liaise between the referer and specialist, and coordinate the response subject to the urgency of each case. It is also the responsibility of the coordinator to manage the technology during each consultation. Upon the specialist’s arrival, the coordinators ensure that an adequate (videoconference) link is made to the regional site, that the sessions run smoothly and accurate usage records are maintained.
Telepaediatric clinics are conducted using standard videoconferencing equipment available in the hospitals. Since the service was established, project designers have set up dedicated videoconferencing rooms (studios) in selected remote sites. The specialists use videoconference studios at the COH. However, at both regional and Brisbane sites, technology handling of clinicians has been kept to a minimum. Basic training is offered to all clinicians, but the majority of responsibility for operating the equipment is maintained by the telepaediatric coordinators. Videoconference calls are made using digital telephone lines (ISDN) at a preferred minimum bandwidth of 384 kbit/s.
The acceptance of this system from both patients and clinicians has been highly satisfactory. For patients, telepaediatric service has resulted in savings for the family who are saved the inconvenience and need for extensive visiters to Brisbane for follow up consultations with specialists. The telepaediatric service has resulted in substantial cost savings for the health service in Queensland which is responsible for subsidising a patient travel scheme. From the specialists’ perspective, it has become obvious that a substantial proportion of sub-specialist outpatient appointments can be done at a distance. One of the leading examples of telepaediatrics is in the area of post-acute burns care where about 17% of all outpatient services are now done through the telepaediatric service.

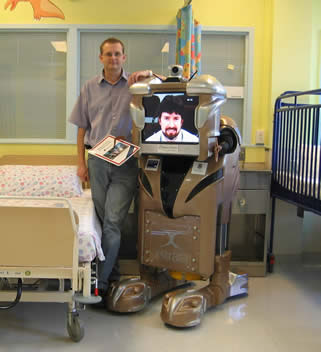
In addition to standard studio-based videoconferencing units, the telepaediatric service has developed a mobile videoconference system for use in the clinical areas. In 2004, the COH introduced a videoconferencing unit dressed up in the shape of a robot in a regional hospital which lacked a full-time paediatrician. “Roy the Robot” (named after Royal Children’s Hospital) has been used for ward rounds where specialist paediatricians from Brisbane could offer remote consultations directly at the bedside. Roy has won the hearts and minds of the children in the hospital while nurses and doctors find him clinically useful. Indicating the success of this method, four new robots are now being launched in different distant sites in Queensland.
Technologies involved in e-health are not always need to be expensive. A low cost e-health project run by the COH in collaboration with the Swinfen Charitable Trust (SCT) has proven that inexpensive methods such as email can be useful for the delivery of health related services. This charitable service provides free medical advice to doctors in developing countries using ordinary email and attached digital images where appropriate. The SCT has been running for eight years and has facilitated a specialist response to more than 1000 clinical questions. More than 200 specialist consultants from around the world have volunteered to provide advices. The growing use of this system is an indication of the usefulness of an email-based e-health application.
The use of the Internet for accessing health and medical information has rapidly increased for the last few years. Both clinicians and health consumers are relying on the Internet as a useful information source. For example, in a survey conducted in 2002, 80% of adult Internet users, or almost half of Americans over the age of 18 (about 93 million), said they have researched health topics on the Internet. 30% of email users have sent or received health-related email.
Online health information sources allow consumers to become informed about diagnoses, surgery or health promoting behaviours, prepare for a visit to their doctor or hospital, share information and give or receive support. From the perspective of a healthcare professional, the Internet may be useful for continuing medical education, conducting online peer review research and access to the latest evidence-based information. The Internet has also become useful tool for health communication. Online discussion lists and news groups, email chat rooms are becoming popular tool for health communication.
With the growing pressures on health services around the world, there is potential for e-health to be used more widely. Despite predictions and high hopes that telehealth (e-health) would become commonplace in the 1990’s, evidence suggests that widespread integration has not occurred. Despite this, the potential of e-health should not be ignored. Instead, important lessons (both successful and failed) should be considered before and during the development of e-health within an organisation.