
A gait screening tool used in a variety of applications is described. Details of a longitudinal study on elderly people attending an exercise class are provided. Results show that simple information to the individual and person running the exercise class helped improve their gait and reduced their risk of falling.
Maintaining mobility is important to both individuals and healthcare providers as it is a fundamental aspect of living a healthy, active lifestyle. Gait analysis is recognised as a clinically useful tool for identifying problems with mobility yet clinical use is still not routine. This is due to limitations with existing technologies, namely: length of time and costs required for performing a gait test and difficulty in interpreting the results. However, with advancements in ICT it is now possible for individuals of every age to be monitored regularly using a sensor based-gait screening tool. One such system, gaitSMART, provides accurate data in a simple, easy to understand format within minutes, overcoming the barriers that are present using existing technical approaches. This originated from a European project, Healthy Aims, with the overall goal to develop a range of medical implants and diagnostic equipment.
If a person grows up with a poor gait then compensatory gait deficits may introduce musculosketal pain in different parts of the body, or osteoarthritis later in life, whereas a good gait will reduce the risk of joint problems later in life. For the generation where joints are already causing problems and replacement surgery is required, good recovery to a normal gait profile will help to prolong the life of the implant. For those active in sports, good recovery from injury is essential. And for the elderly, where falls are a major concern, identifying those with a problematic gait and monitoring through exercises or treatment improves mobility and reduces costly falls.
This paper describes how the gait screening tool has been used in a variety of applications and then provides details of a two year longitudinal study on a group of 11 elderly people attending a weekly exercise class. The findings are that providing simple information to the individual and the person running the exercise class helped improve their gait and reduced their risk of falling.
Identifying the precise abnormality within the gait profile is essential if it is to be corrected, either by training, exercises, drugs or surgical intervention. If identified early enough, exercises may be sufficient, alleviating pain and reducing the likeliness of surgical intervention. An unstable or uneven gait can result in a worsening in a medical condition, or in the elderly it may result in a fall. Gait profiling as part of a medical diagnosis makes it possible to quantify the gait abnormality for individuals, identify problems early and prescribe the best course of treatment. For example, if early stage knee osteoarthritis (OA) can be detected then therapy may be an option, whereas late stage knee OA generally dictates replacement surgery. The elderly may be offered a set of exercises to strengthen particular muscles and help reduce their risk of falling.
GaitSMART is a sensor-based system that accurately monitors the lower limb movement through the gait cycle. It does this using four Inertial Measurement Units (IMUs), which collect acceleration and rotational data in six Degrees of Freedom (DOF) at 100Hz. The sensors are mounted onto the thigh and shank of each leg using custom designed straps with integral pockets, which are light enough not to affect the limb movement. All units are synchronised in time prior to the test and data is stored onto an SD card for the duration of the test, which typically lasts a few minutes. Once the test is complete the IMUs are linked to a laptop, the data is automatically downloaded and the thigh and shank movement, knee flexion and stride duration are calculated. These values are presented on the screen in simple graphical form and the user can then prepare a simple report with graphical and tabular output, all within minutes, making it suitable for use in a clinical setting. In addition, the values are automatically compared to normalised data and amber or red warning indicators given on any parameters that are outside the limits.
The gait cycle can be described as the movement of the lower limbs in 3D space over time. Using sensor technology, the orientation of each limb segment can be quantified and plotted in time. In any test there will be a number of strides, or repeat gait cycles. These can be automatically calculated and individual strides identified, from which the typical stride can be determined. This can then be compared to normalised data, and values which are outside range can be highlighted. This approach overcomes one of the major barriers with previous gait systems, where normalised data is not readily available or referenced.
The data presentation is also important as both the client and person responsible for treating the client need to be able to understand the results. The simple graphics in the gaitSMART system report show movement of each segment and the knee angle through the gait cycle, which visually highlights differences between the left and right. A table identifies specific values which are easy to understand, for example knee range of motion (flexed to straight).
The system has been validated against an optical system and data on healthy people over the age range 18-97. This data forms the normalised data used to identify and highlight any values outside the normal range. It has also been used in a variety of health applications over the last two years. These include:
It has been used in rugby and football clubs to help ensure that injured players recover correctly and do not overwork the injury during training or when playing. Regular gait screening has enabled the physiotherapist to adjust training so that players remain match fit.
It has been used in both the NHS and private sector as part of the diagnosis process for knee problems and monitoring the rehabilitation phase after treatment. This has included ACL reconstruction, meniscus tear repair, treatment of knee osteoarthritis, and knee replacement surgery. It is evident from these studies and other published studies that pain is not a good indicator for the severity of the problem and individuals are unaware of their gait defects. It is also evident that if no quantifiable objectives are set during rehabilitation, the outcomes may be poor, particularly for total knee replacement. Individuals will often not work through pain unless they can see the benefits, and so gait screening would improve the long term outcome.
Knee OA is one of the most common causes of knee pain, and therapy can alleviate the pain if the condition is detected at the early stage. Specific gait parameters quantified using the gaitSMART system relate to knee OA and hence the condition can be detected early. This is also applicable to the orthopaedics sector, where less invasive treatment could be offered.
One of the main concerns with elderly people is their risk of falling. If a fall occurs it can lead to hospitalisation, joint replacement, a reduction in their quality of life, or even death. In the year 2000, it was the second most common form of accidental death in Asia, and the prevalence of falls in those over 60 was over 10 per cent, rising to 30 per cent in some regions. The annual cost of falls varies across Asia, for example $500 million in Australia and $17 million in Japan. It is recognised that there are many intervention strategies that can be used to help prevent falls, but there is no standard process for monitoring the long-term benefits of these on an individual basis. One of the most common reasons for falling is tripping and this is directly related to knee flexion in swing.
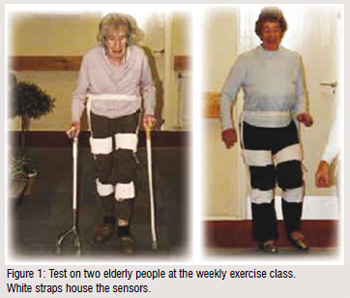
The gait system has been used in a longitudinal study on a group of elderly people attending a weekly exercise class, age range 68-91 (Figure 1). Many of the class members have trouble walking and some use walking aids. The study was to test the hypothesis that providing gait data to the individuals and the class teacher in a simple to understand format on a regular basis would result in an improved gait and lower the risk of falling. The gait profiles from healthy individuals over the same age range were used for comparison purposes.
The study started in September 2010 and the gait system was taken to the exercise class location every 2 months. All those in attendance at each session were monitored, with each person leaving the class for less than 5 minutes. This ensured minimal disruption to the class activities and ensured all people were tested and results fed back before the end of the class. As their progress was monitored their history data as well as current data was provided. The age, health status and time of monitoring for 11 class members is summarised in Table 1.
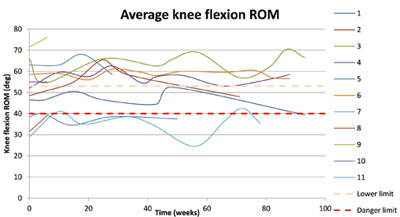
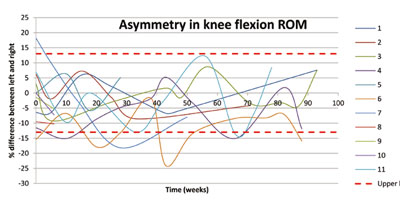
The average knee range of motion (ROM) and asymmetry in knee ROM over time have been plotted in Figures 2 and 3 respectively for 11 members of the class.
As can be seen from figure 2, seven of the members were above the normal limit throughout. Two other members were below the normal limit but above the danger limit. The final two members were below the danger level. These were the person with the lower limb prosthesis and the one walking with sticks. Positive intervention was provided in the way of focused exercises for all 11 members, particularly when their own values were reducing significantly. This can be seen from the cyclic motion in the plots.
For the symmetry between the left and right leg, eight of the class members retained symmetry within the normal limits and none of the class members were outside the limit consistently. Of those members where symmetry was sometimes an issue, corrections were made by focusing exercises on the less active knee.
The knee ROM was chosen as this directly relates to toe clearance, which is important to avoid tripping on objects. Minimum toe clearance occurs around peak knee flexion and small variations in knee angle can result in noticeable changes in minimum toe clearance. A limit of 40? is seen as the danger level, whereby below this value toe clearance may not be adequate to clear small obstacles on the floor. The two class members were aware of the dangers and applied extra vigilance, but occasionally a fall would occur. None of the other nine members experienced falls.
Asymmetry is seen as important as this can cause problems with balance. The worst class member was the one who had a stroke. When the asymmetry went outside limits, extra exercises for the poor side were given and the asymmetry reduced accordingly.
Mobility is crucial for a good quality of life. In our early years this may be hampered by injury and it is important that recovery is complete otherwise problems such as osteoarthritis can occur later. As people get older, joints often suffer and less invasive treatment such as exercises or drugs may suffice. Left untreated until the problem becomes critical often results in joint replacement surgery. And finally as they get older they may have problems moving as effectively and if this is not addressed it may lead to falls and ultimately complete loss of mobility. With this new technology it is now possible to monitor gait profile, so problems can be identified early enough and corrective action taken. This will lead to a more active lifestyle, an improved quality of life and ultimately lower health costs.