
McDonald’s consumer focus offers some important lessons for the healthcare providers to ponder as they are forced to transform into more consumer-driven organisations.
As industrialised societies pursue solutions for providing cost-effective healthcare services to their larger and older populations, consumerism is emerging as a new force with the potential to reshape the industry and its economics. Whether in the context of a fully public, fully private or a hybrid healthcare system, consumerism is now a global phenomenon that, many believe, may be the “holy grail” for achieving greater efficiency and value in healthcare, while keeping costs under control.
Media reports and marketing campaigns touting the potential of healthcare consumerism proliferate, but what that means for providers—hospitals, in particular—remains cloudy. With so much attention focussed on mechanisms that empower patients to shoulder greater financial responsibility for their care, providers still need guidance as to what they can do to best cater to changing consumer needs. At a minimum, we can realistically expect that regardless of national boundaries, the consumer-driven hospital of tomorrow is going to need to look substantially different from the system-driven hospital of today.
We first want to articulate clearly what we believe to be the newly emerging paradigm in healthcare consumerism around the globe. While each national system can be characterised by its own unique context and trends, there are several key principles that, we believe, define consumer-driven healthcare environments. We highlight these basic principles in table 1.
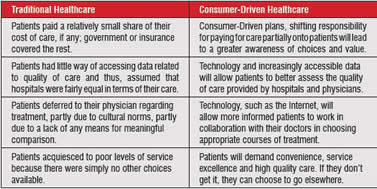
Table 1 While consumerism has been a transformational force in other industries, it has yet to have the same impact in healthcare, making the right side of the comparision above more of a projection than a description. Even though healthcare service provision is so different than other consumer-driven services-not to mention exponentially more complex-we believe that there are key lessons to be learned from other industries that have weatheredthe challenges of providing consumers exactly what they want. While consumerism has been a transformational force in other industries, it has yet to have the same impact in healthcare, making the right side of the comparision above more of a projection than a description. Even though healthcare service provision is so different than other consumer-driven services—not to mention exponentially more complex—we believe that there are key lessons to be learned from other industries that have weathered the challenges of providing consumers exactly what they want.
In our search for example, one consumer-driven company boldly shines as an international success story.
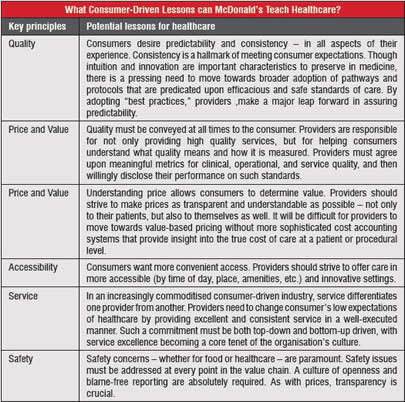
Table 2 McDonald’s, the fast-food behemoth, is the envy of companies everywhere. With over US$ 21 billion in sales in 2006 and a US$ 3.5 billion profit, they have much to covet. Last year, it served more than 52 million people every day in one of its 30,000 restaurants in any of the 119 countries where it operates. Whether serving a McOz burger in Australia, or a McAloo Tikki Vegetarian burger in India, McDonald’s has mastered the art of satisfying its local customers. Health effects of fast food aside, McDonald’s can offer some interesting lessons to health providers worldwide.
As an economic, social and cultural phenomenon, McDonald's had adapted its operational and strategic model to every national culture. To achieve the success it has, McDonald's has managed to stay true to some key principles as to how it can best suit the wants and desires of even the most demanding international customers.
McDonald’s success is deeply rooted in its ability to deliver a product with great predictability and consistency, giving consumers great confidence in the McDonald’s brand. Whether a Big Mac is purchased in the US or Japan (depending on regional variations), customers have come to expect a similar experience. Even behind the product, the tight engineering process used minimises variations and results in tremendous efficiencies. To hardwire that predictability, over 275,000 graduates of McDonalds’ Hamburger University have worked in franchises worldwide.
Healthcare is the antithesis of McDonalds: its ability to produce standard, replicable outcomes and processes is very limited. In the US, dramatic geographic variations in delivery and outcomes have been well documented.
Physicians, the key health decision makers in all cultures, have tended to adopt pathways and protocols slowly, if at all, contributing to vast differences in how care is delivered.
McDonald’s has been methodical in developing its supply chain to ensure timely and local access to the right ingredients for its products. It has set exceedingly high training expectations to ensure that its brand standards are understood, honoured and delivered every day.
The healthcare industry is just beginning to make some inroads with quality indicators, though quality is infinitely more complex and difficult to measure. Healthcare could benefit from more science and far less marketing hype related to conveying quality. In a consumer-driven environment, value cannot be assessed in the absence of reliable quality metrics.
McDonalds’ customers can easily determine, by looking at value and price, whether they want to eat at another restaurant or not.
Pre-packaged meal options, as well as portions of various sizes and prices, allow customers to select exactly what they wish with a clear sense of the value it offers them. When arriving at a hospital, few patients have any idea about the value of the care they receive. True compensation or reimbursement in many systems varies based upon contractual allowances invisible to patients.
Though some insurers and hospitals have developed small, limited menus with prices, that practice is still rare.
In some markets, it seems as if there is a McDonald’s on every street corner. With 30,000 distribution points around the world (and growing), McDonald’s can offer its products to everyone, anytime and almost anywhere.
The complexity of traditional healthcare precludes the easy distribution of many services. While some services can be offered in stand-alone ambulatory facilities, few innovative models exist that succeed on the same level. For privately insured systems, lack of health insurance also restricts accessibility.
McDonald’s customers worldwide expect to be greeted rapidly and politely upon their arrival. They can quickly place their order and know it will be delivered promptly. If there are problems, the manager and staff can remedy them immediately.
For many patients, service in healthcare is an oxymoron. Patients and providers have come to expect hassles, multiple forms, unreasonable wait times, mistakes and miserable conditions when they seek healthcare services. Many hospitals speak the language of service; yet fall short when it comes to delivering it.
McDonald’s has successfully infused its restaurants and suppliers with a culture of safety that includes 72 daily safety checks per restaurant per day, 2,000 safety and quality checks in each chicken and beef supplier’s facilities, and 95 daily checks for potato providers. In the US, McDonald’s has a collaborative relationship with USDA inspectors—who have unfettered access to all points of production at all times.
Issues of safety violations in healthcare abound around the world. With all its complexities, the healthcare industry is still rife with structural barriers to safety and a culture of “shame & blame” when it comes to reporting errors. Too often, episodic care models simply do not allow for sufficient safety monitoring of patients, resulting in unnecessary infections, costs and even deaths.
Given McDonald’s unquestionable success as a global leader in providing consumers with exactly what they desire, what lessons might we extrapolate out to the healthcare industry around the world? We summarise some of the key lessons in the table 2.
The need for transformational change is being heeded by healthcare organisations across the globe, though the pace of change seems glacial at times. Among the leading organisations in the United States committed to such change are:
• Intermountain HealthCare, Salt Lake City, Utah, which has been a pioneer in the adoption of clinical best practices, and devotes significant resources to ensuring the quality and safety of its services.
• The Mayo Clinic, which has maintained a tradition of process standardisation and quality since its very inception. Today, it is a pioneer in the adoption of health information technology—which is transforming its organisation into a paperless provider of care.
• US Oncology, a premier provider of ambulatory oncology services, that integrates diagnostic, medical and radiation oncology services in state-of-the art facilities designed to meet the needs of consumers. US oncology represents an example of disruptive innovation whereby the market is fundamentally challenged by the emergence of a new model of care that resonates strongly with the needs and desires of consumers
As consumerism evolves in each national market, healthcare providers are going to be required to adapt to the unique demands and expectations of their patients and governments. To succeed, hospitals must quickly learn from other industries and take action to make themselves as responsive to consumers as possible. While there is much conceptual distance between fast food and healthcare, McDonald’s offers some important lessons for providers to ponder as they are forced to transform into more consumer-driven organisations.