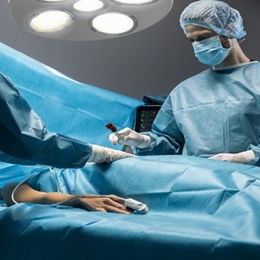
Closing the Loop on Perioperative Safety
Leveraging Closed-Loop TIVA is Transforming Anesthesia Delivery
Closed-loop total intravenous anesthesia (TIVA) systems represent a transformative shift in perioperative medicine. By integrating real-time physiological feedback with algorithm-driven drug delivery, these platforms enhance patient safety, support consistency of care, reduce clinician workload, and support scalable, high-reliability anesthesia delivery worldwide.
Introduction
The World Health Organisation estimates that medical harm affects approximately 10% of patients, with nearly half of these events preventable. In anesthesiology, where clinicians manage high-stakes physiology in real time, the pace of decisions, the complexity of systems, and the sheer volume of information heighten the risk of harm. To meaningfully advance perioperative safety, the field must move beyond incremental improvements to legacy systems. Transformative gains in perioperative safety must integrate next-generation technologies that reduce cognitive burden, automate routine tasks, and strengthen situational awareness, enabling clinicians to focus on complex decision-making and whole-patient care.
Rising surgical complexity and mounting workforce pressures intensify the urgency to adopt technologies that strengthen safety and reduce variation in care. Clinicians commonly administer TIVA manually, but this approach relies heavily on operator judgment and generates substantial variability in drug delivery, patient response, and recovery trajectories. Even experienced clinicians adjust infusions continuously, and these moment-to-moment titrations can create dosing fluctuations that trigger hemodynamic instability, delay emergence, or increase the risk of unintended intraoperative awareness.
Closed-loop anesthesia systems deliver a compelling solution. These platforms interpret real-time physiologic data, typically processed EEG for hypnotic depth and nociception metrics when opioids are integrated, and algorithmically decide when to adjust drug delivery. They then execute those adjustments automatically. This approach delivers more precise, reliable, and efficient perioperative care and it frees clinicians to focus on higher-order decision-making.
Crucially, these systems are not designed to replace anesthesiologists, but to empower them. By maintaining anesthetic depth within tight therapeutic boundaries, supporting hemodynamic stability, reducing cognitive load, and standardising performance across disparate environments, closed-loop anesthesia offers more than operational efficiency, it offers a pathway to fundamentally reimagine patient safety. It enables clinicians to shift from reactive management to proactive, high-fidelity decision-making, ultimately advancing a future in which no patient is harmed by anesthesia care.
Understanding Closed-Loop TIVA
First-generation closed-loop TIVA systems used a single-input, single-output architecture that linked a depth-of-anesthesia index directly to propofol infusion rates. As technology advanced, closed-loop anesthesia platforms entered a period of rapid generational refinement. Second- and third-generation systems now deliver far greater stability, responsiveness, and resistance to artifact, and they consistently outperform earlier prototypes.
A current iterative product coordinates three essential components of anesthetic management: sedation, analgesia, and neuromuscular blockade. It relies on continuous physiological feedback, such as the Bispectral Index (BIS) for sedation and train-of-four for muscle relaxation, and uses these data streams to maintain target ranges and adapt to each patient’s needs in real time in an integrated, coherent manner. By continuously synchronizing these variables, the system maintains a balanced anesthetic state tailored to each patient’s dynamic physiological state. This data-driven coordination enhances stability while reducing the need for frequent manual intervention.
From a patient safety standpoint, the essential feature is not automation per se but in the system’s ability to pair high-quality monitoring signals with medication delivery through transparent algorithms and well-defined safety limits. These systems actively reduce variability in drug effect and promote consistent physiological control in perioperative environments that demand high cognitive performance.
How Closed-Loop Control Works
A closed-loop TIVA system operates in two operational phases: induction and maintenance. During induction, algorithm-driven sequential dosing adjusts drug delivery and achieves the targeted anesthetic state while minimising hemodynamic perturbations. In the maintenance phase, the system continuously analyses real-time physiologic signals and adjusts infusion rates to keep drug concentrations within the therapeutic range. It maintains tight alignment between measured physiologic inputs and defined treatment targets to prevent supra- or subtherapeutic dosing.
The system incorporates multiple safety controls. It sets dosing limits, allows clinicians to override automation instantly, and issues alerts when it detects abnormal trends. These controls keep automation transparent, bounded, and responsive to the clinician. They ensure that automation strengthens, rather than replaces, clinical judgment.
Clinical Benefits
Early evaluations of closed-loop TIVA systems demonstrate several clinically significant advantages. These systems maintain anesthetic depth within predefined target ranges more consistently than manual control, decrease the number of manual adjustments during prolonged or complex procedures, and provide more stable physiologic control throughout the anesthetic course. Together, these effects promote more uniform patient management and lessen the cognitive and physical demands placed on clinicians.
More stable anesthetic delivery directly contributes to faster emergence, lowers postoperative opioid requirements, and produces more predictable recovery trajectories. These outcomes are priorities for health systems globally and underscore the potential of closed-loop TIVA to enhance perioperative efficiency and patient outcomes.
Safety and Ethical Considerations
Patient safety remains the primary consideration for any new or emerging technology. Automation redistributes work; it does not redistribute responsibility. Anesthesiologists retain responsibility for overall patient management, including hemodynamic stability, airway protection, and responses to surgical stimuli. Ethical and legal questions, including accountability for algorithmic errors and the protection of patient data, demand clear guidelines and well-defined governance frameworks.
As closed-loop systems enter clinical practice, several concerns warrant heightened attention. Closed-loop platforms must preserve immediate clinician authority by providing unmistakable visual confirmation of system status, continuous alarm visibility, and instant, unambiguous manual override. Any delay between recognition and intervention creates a patient-safety vulnerability. Transparent algorithm design and robust fail-safe mechanisms strengthen clinician and patient trust and ensure that automation supports, rather than compromises, high-reliability care.
Challenges and Future Directions
Closed-loop TIVA systems continue to advance, yet their adoption unfolds within a complex ecosystem. Health systems confront financial pressures, clinicians navigate ingrained cognitive habits, and regulators are challenged to keep pace with rapidly evolving technologies. Institutions must invest in compatible infusion platforms and high-fidelity monitoring systems, while clinical teams commit to mastering new workflows and override protocols. Leaders who integrate these systems thoughtfully can improve operating-room efficiency and accelerate the transition toward data-informed, high-reliability anesthesia delivery.
As workforce shortages intensify and large segments of the anesthesia workforce approach retirement, the specialty faces a defining moment. Supporting technologies will increasingly fill critical gaps, extending the reach of skilled clinicians and stabilising perioperative care in resource-constrained environments. Emerging innovations already point toward a more connected and adaptive future, AI-enabled predictive analytics that anticipate physiologic instability before it arises, remote-monitoring architectures that bring tele-anesthesia to underserved regions, and refined nociception metrics that strengthen analgesic precision across diverse clinical settings.
The integration of artificial intelligence is driving rapid progress in closed-loop anesthesia. Unlike traditional rule-based systems, AI models learn patient-specific physiologic responses in real time, foresee evolving risk, and generate dosing strategies that optimise safety and efficiency. These capabilities shift automated anesthesia from reactive control to anticipatory, personalised management, an evolution that parallels broader transformations across medicine.
Ultimately, automation should complement human expertise, enabling clinicians to focus on complex decision-making and patient advocacy, the elements of care that define the future of the specialty. As these technologies mature, they offer a vision of perioperative medicine in which every patient benefits from the combined strengths of human insight and advanced computational support.
Conclusion
Closed-loop TIVA systems signal a pivotal evolution in anesthesia care. By uniting closed-loop control and real-time physiologic feedback, these platforms do more than refine existing practice; they redefine what is achievable in high-reliability perioperative medicine. They enhance patient safety, reduce unwarranted variability, improve efficiency, and support workforce sustainability. Successful implementation depends on education, infrastructure, and iterative improvements. For healthcare leaders worldwide, closed-loop anesthesia is not simply a technological upgrade; it is a strategic investment in safer, more reliable, and more scalable perioperative care delivery.
As innovation accelerates, these systems hold the potential to become a defining pillar of modern perioperative healthcare. By coupling human expertise with advanced computational intelligence, closed-loop TIVA systems help shift healthcare from a reactive paradigm to one that anticipates risk, personalises therapy, and proactively protects the patient. They point toward a future in which precision, reliability, and compassion converge, advancing a new era of perioperative care in which every patient benefits from the combined strengths of clinician judgment and intelligent technology.