CCR5 Modulation as a Systems-Level Strategy for Addressing Neuropathic Pain
Neuropathic pain affects millions worldwide and remains resistant to conventional treatments due to chronic neuroimmune dysregulation. Emerging evidence highlights CCR5-driven inflammatory signaling as a key mechanism in persistent neuropathic pain. This article explores the rising burden on healthcare systems and outlines how CCR5 modulation may offer durable neural resilience through host-directed, biologically grounded interventions.
Introduction
Neuropathic pain has become one of the most costly and strategically neglected health challenges of the modern era. Affecting hundreds of millions globally, including rapidly aging populations across Asia and its impact extends beyond clinical symptoms to economic burden, disability, and long-term healthcare strain. Unlike nociceptive pain, neuropathic pain arises from dysfunctional neuroimmune signaling and maladaptive neural plasticity, making it resistant to traditional analgesics and a driver of long-term opioid use and dependency risk.
By targeting upstream inflammatory pathways and neural circuitry dysfunction, CCR5-based therapies may offer the potential for disease modification, reduced reliance on opioids, and improved long-term quality of life for patients.
Neuropathic Pain as a Systems-Level Disorder
Neuropathic pain persists due to a pathological dialogue between neurons, immune cells, and glia. Following injury, infection, chemotherapy exposure, or chronic inflammation, microglia become activated, releasing cytokines and chemokines that sensitise neurons and maintain hyperexcitability. This neuroimmune dysfunction establishes a persistent pain state that continues long after the original insult has resolved. Traditional analgesics often fail because they target downstream symptoms rather than upstream immune-driven mechanisms.
Recognising neuropathic pain as a systems-level disorder underscores the need for therapies that restore normal neuroimmune communication. Emerging interventions, including glial modulators, anti-inflammatory biologics, and neuromodulation are shifting the paradigm toward disease-modifying approaches. By understanding how immune signals alter synaptic plasticity and neural circuitry, researchers can develop precision treatments tailored to underlying mechanisms rather than masking symptoms. This holistic perspective may offer more durable relief to the millions living with chronic neuropathic pain, where current medications often provide incomplete or temporary benefit.
CCR5 in Neuroimmune Dysregulation
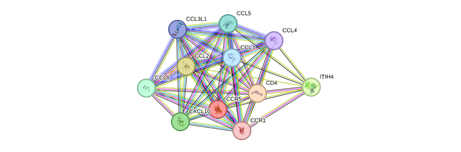
The CCR5 receptor—known for its role in immunology and infectious disease—has increasingly been recognised as a critical driver of neuroinflammation. Expressed on microglia, macrophages, T cells, and some neurons, CCR5 amplifies inflammatory cascades when activated by ligands such as CCL3, CCL4, and CCL5.
Injury/Trigger → CCR5 Activation → Microglial Response → Neuroinflammation → Central Sensitisation → Chronic Pain
CCR5 acts as a molecular switch capable of locking the nervous system into a heightened danger state. When excessively activated, it promotes persistent glial reactivity and disrupts normal neuronal signaling, contributing to long-term pain sensitisation. Pharmacological CCR5 blockade has demonstrated the ability to reduce neuroinflammation, reverse synaptic dysfunction, and support functional recovery in preclinical studies. As such, CCR5 represents a promising target for next-generation therapies targeting chronic pain, neurodegeneration, and post-injury cognitive impairment. Ongoing research focused on CCR5 modulation may help break the cycle of neuroimmune dysfunction and enable restoration of neural homeostasis.
Key Evidence Supporting CCR5 in Neuropathic Pain
| Model | Key Finding |
| Paclitaxel model | CCR5 blockade reduced mechanical allodynia |
| Glial activation models | CCR5 regulated chronic microglial inflammation |
| Chronic pain models | CCR2–CCR5 synergy maintains neuroinflammation |
| Persistent pain models | CCR5 contributes to central sensitization |
Figure. Key Studies Linking CCR5 and Neuropathic Pain
CCR5 Modulation as a Host-Directed Therapy
Targeting CCR5 offers several upstream advantages:
- Reduced glial activation and inflammatory signaling
- Improved synaptic regulation by normalising maladaptive plasticity
- Suppression of chronic immune-activation cycles
- Compatibility with multimodal pain strategies and trauma-informed care
Host-directed approaches work at the biological level where neuropathic pain actually begins.
Implications for Asia’s Healthcare Systems
Across Asia, neuropathic pain contributes to rising hospital utilisation, disability costs, and care complexity, particularly among cancer survivors, diabetic patients, aging populations, and trauma-exposed workers. These trends are accelerating due to increasing diabetes rates, greater cancer survivorship, and higher occupational injury burdens.
CCR5 modulation aligns well with these healthcare priorities by offering a precision-based, inflammation-targeting strategy capable of reducing system strain and improving patient resilience. By addressing inflammation and central sensitization at their biological source, CCR5-based approaches have the potential to reduce opioid reliance, improve functional recovery, and support healthy aging key priorities throughout the region.
The Neuroimmune Feedback Loop
Neuropathic pain is sustained by a self-reinforcing neuroimmune feedback loop involving injury-triggered inflammation, CCR5 activation, glial responses, and central sensitisation. Interrupting this loop is essential for durable pain relief.
Nerve damage activates peripheral immune cells, which release pro-inflammatory mediators that sensitise nociceptors. This inflammatory surge triggers CCR5 signaling, a chemokine receptor pathway that plays a pivotal role in coordinating immune-cell recruitment and inflammatory amplification.
As the process continues, microglia and astrocytes transition into reactive states that secrete cytokines and neurotoxic factors, enhancing pain transmission. The nervous system becomes locked in a state of heightened responsiveness, central sensitisation, where even non-painful stimuli may be interpreted as painful (allodynia).
Proposed Framework for Clinical Integration
To prepare for next-generation neuropathic pain therapeutics, healthcare systems should prioritise:
- Clinician education in neuroimmune biology
- Investment in host-directed therapy research
- Multidisciplinary integration across neurology, immunology, pain medicine, and rehabilitation
- Policy adoption recognising neuropathic pain as a systems-level challenge requiring upstream interventions
Educating clinicians on neuroimmune mechanisms enables earlier recognition of pain pathophysiology and better alignment of therapy with underlying biological drivers. Increased investment in host-directed research, including therapeutics that modulate CCR5 and related pathways will accelerate access to treatments designed to interrupt chronic pain at its source.
Integrated care models ensure collaboration among specialists addressing the neural, immune, and functional dimensions of pain. In parallel, health policy must shift toward prevention, early intervention, and mechanistic treatment models that reflect the systems-level nature of neuropathic pain.
This framework positions healthcare systems to deliver durable, mechanism-based relief and improved patient outcomes.
Conclusion
Neuropathic pain is a systems-level challenge requiring biological insight and therapeutic innovation. CCR5 modulation represents a promising therapeutic direction capable of reshaping pain treatment by targeting the immune-neural circuits responsible for chronic pain. By embracing host-directed approaches, healthcare leaders can improve patient outcomes and strengthen long-term system resilience.
Chronic neuropathic pain remains one of the most difficult conditions to manage, often persisting despite conventional treatments. Its complexity reflects disruption not only in nerve signaling but also in the immune pathways that shape neural function. This makes the disorder both a clinical and strategic challenge, one that demands therapies capable of addressing its root biological drivers.
CCR5 modulation moves meaningfully toward this goal. By targeting chemokine pathways responsible for ongoing neuroinflammation and hypersensitivity, CCR5-focused approaches aim to break the mechanisms that convert acute injury into chronic pain. Instead of temporarily masking pain symptoms, these therapies work to restore healthier immune–neural communication.
A systems-level problem requires systems-level solutions, grounded in precision biology and an understanding of the full landscape of neural–immune interactions.
References
- Zhong J, Fang J, Gao R, et al. Blockade of CCR5 suppresses paclitaxel-induced peripheral neuropathic pain. Neuroscience Letters. 2023.
- García-Domínguez J, et al. The role of the CCR5 receptor in neuropathic pain. Biomedicines. 2025.
- Bober Z, et al. Chemokine receptor interactions in chronic pain. International Journal of Molecular Sciences. 2024.
- Szabo-Pardi T, et al. CCR5 contributes to persistent pain states. Pain. 2021.









-(1).jpg)