Evolution of Transcatheter Interventions in Pediatric Cardiology: A Decade of Progress

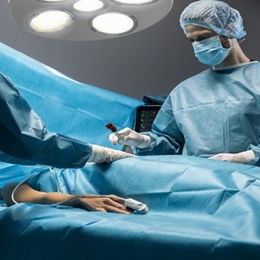
Over the past decade, transcatheter interventions in pediatric cardiology have undergone significant transformations, marking a pivotal evolution in the management of congenital heart diseases. Technological advancements have been at the forefront of this progress, introducing innovative devices and techniques that enhance the safety and efficacy of minimally invasive procedures tailored specifically for neonates and infants.
These interventions have led to markedly improved patient outcomes, as they allow for precise treatment of congenital heart defects that were once considered difficult or impossible to address without open-heart surgery. Procedures such as transcatheter closure of atrial and ventricular septal defects, valve interventions, and hybrid approaches have expanded the spectrum of treatable conditions, there by broadening clinical indications.
Introduction
Transcatheter interventions have emerged as a vital approach in managing congenital heart diseases among pediatric patients. These minimally invasive techniques offer numerous advantages over traditional surgical methods, fundamentally changing the landscape of pediatric cardiology over the last decade.
Advantages of Transcatheter Techniques
- Minimally Invasive Nature: Unlike open-heart surgery, transcatheter procedures typically require only small incisions, reducing trauma and facilitating faster recovery times for young patients.
- Lower Risk of Complications: With reduced operative stress, there is often a lower incidence of complications, which is crucial for the delicate physiologies of neonates and infants.
- Shorter Hospital Stays: Many transcatheter procedures enable patients to return home sooner than those undergoing conventional surgeries, ideal for both families and healthcare systems.
- Expanded Treatment Options: Advances in technology have broadened the scope of defects that can now be treated transcatheterly, including complex conditions that previously required extensive surgical intervention.
Developments in the Last Decade
Over the past ten years, the refinement of devices, such as specialized occluders and stents, has improved treatment precision and effectiveness. Moreover, advancements in imaging technologies allow for better guidance during procedures, enhancing outcomes and reducing the risk of incorrect placements.
The combination of these advancements has made transcatheter interventions increasingly relevant, providing safer, less invasive care options that significantly impact the prognosis for young patients with congenital heart defects. Ongoing research and clinical trials are essential to continue this momentum, addressing both challenges and ensuring accessibility to these life-saving treatments.
Technological Advancements
The last decade has witnessed remarkable technological advancements in transcatheter interventions, fundamentally enhancing the landscape of pediatric cardiology. Key improvements have focused on device miniaturization, the development of bioabsorbable materials, and advancements in imaging techniques, all of which have significantly raised the safety and efficacy of these procedures.
Device Miniaturization
One of the most critical developments has been the miniaturization of cardiovascular devices, enabling their use in neonates and infants who possess anatomical constraints that pose challenges for traditional interventions. Smaller devices such as occluders and stents can now be delivered through narrow vascular pathways, minimizing trauma and allowing for more precise placements in delicate structures.
Bioabsorbable Materials
The introduction of bioabsorbable materials has revolutionized device design. These materials degrade over time, reducing the need for subsequent interventions associated with permanent implants. Such innovations not only alleviate long-term complications related to device permanence but also enhance patient comfort by decreasing foreign body reactions and associated inflammatory responses.
Improved Imaging Techniques
Advancements in imaging technologies, including high-resolution echocardiography and real-time 3D fluoroscopy, have drastically transformed procedural planning and execution. These imaging modalities facilitate superior visualization of the heart's structure and function, allowing clinicians to navigate complex anatomies with enhanced precision during interventions. Additionally, augmented reality (AR) is being explored to overlay critical anatomical information onto the operating field, providing real-time guidance during procedures.
Implications for Safety and Efficacy
These technological advancements converge to significantly improve patient outcomes. The combination of less invasive techniques, better visualization, and tailored materials results in reduced procedure times, lower rates of complications, and shorter hospital stays. The expansion of transcatheter approaches into previously untreatable conditions further underscores the transformative nature of these innovations, ultimately broadening access to life-saving interventions for pediatric patients with congenital heart diseases.
Impact on Patient Care
The shift towards transcatheter methods has profound implications for patient management and outcomes:
| Benefits of Transcatheter Interventions | Traditional Surgical Approach |
| Minimized Surgical Trauma | Involves extensive incisions and recovery time |
| Quicker Recovery | Prolonged hospital stays and downtime |
| Reduced Risk of Complications | Higher operative risk and associated complications |
| Lower Anesthesia Exposure | Longer exposure during surgical procedures |
Accessibility and Acceptance
The broadening of clinical indications has not only simplified treatment pathways but also facilitated quicker access to care. As a result, families can benefit from earlier interventions, thus improving quality of life for patients. However, despite these advancements, challenges remain. Specialized training for healthcare teams is essential to ensure the safe and effective implementation of these techniques. Furthermore, economic barriers must be addressed to maintain equitable access to these innovations, ensuring that all pediatric patients benefit from advances in transcatheter interventions.
Challenges and Limitations of Newer Transcatheter Therapies
Despite the promising advancements in transcatheter therapies for pediatric patients, several significant challenges and limitations persist. These issues can impact the widespread implementation and overall success of these innovative techniques, particularly in various healthcare settings.
Need for Specialized Medical Teams
The complexity of transcatheter procedures necessitates well-trained, multidisciplinary medical teams. Surgeons, interventional cardiologists, anesthesiologists, and specialized nursing staff must work cohesively to ensure optimal outcomes. However, the lack of access to adequately trained professionals in some regions can hinder the adoption of these therapies, particularly in rural or developing areas where pediatric cardiology services may be limited.
Economic Barriers
Transcatheter interventions often involve high costs associated with advanced technologies, specialized equipment, and personnel training. These expenses can create significant financial barriers for healthcare systems, particularly in low- and middle-income countries. Funding constraints may limit access to state-of-the-art devices, making it challenging for hospitals to offer these life-saving treatments.
Access Disparities
Access to transcatheter therapies is not uniform, as disparities exist between urban and rural settings, as well as between developed and developing nations. Addressing these challenges is crucial for maximizing the benefits of transcatheter therapies and ensuring that all pediatric patients with congenital heart diseases have equal access to life-saving interventions.
Improved Safety Profiles and Outcomes
Over the past decade, the safety profiles and outcomes of pediatric transcatheter interventions have shown remarkable improvements, underscoring their critical role in the management of congenital heart diseases. As techniques have evolved, so too have the metrics that define their success.
Success Rates and Complication Statistics
Current data indicate that success rates for common transcatheter procedures—such as atrial septal defect (ASD) and ventricular septal defect (VSD) closures—exceed 90%, reflecting the growing proficiency in this field. Complication rates have significantly decreased, averaging around 2-5% for many interventions, compared to up to 20% associated with traditional surgical approaches. This reduction is vital for high-risk populations, particularly neonates and infants who possess unique physiological challenges.
Advances in Patient Monitoring
Innovative technologies have led to enhanced real-time monitoring during transcatheter procedures, contributing to improved patient outcomes. For instance, the integration of advanced imaging modalities allows for:
- Technical precision to guide device placement
- Reduced procedural times
- The avoidance of unnecessary risks associated with traditional open-heart surgeries
Personalized and Image-Guided Therapy
In recent years, there has been a noteworthy shift toward personalized treatment approaches in pediatric cardiology, driving advancements through genetic insights and sophisticated imaging techniques. Personalized therapy aims not only to enhance the efficacy of interventions but also to tailor treatments based on unique patient characteristics.
Genetic Insights
The integration of genomic data into clinical practice enables healthcare professionals to customize interventions for each patient. Genetic testing can identify specific molecular markers related to congenital heart defects, allowing for
- Targeted therapies
- Enhanced risk assessment
Advanced Imaging Techniques
The role of advanced imaging technologies in pediatric cardiology has become increasingly pivotal. Tools such as 3D printing and augmented reality provide unparalleled support in procedural planning and execution:
- 3D Printing: This technology allows for the creation of patient-specific anatomical models, offering a tangible reference for planning complex interventions.
- Artificial Intelligence (AI): AI applications enhance image interpretation, assisting clinicians in making data-driven decisions. By analyzing various imaging modalities, AI can forecast the potential success of procedures based on historical data.
- Virtual Simulations: These tools provide a platform for training and skill development, allowing cardiologists to refine their techniques in a risk-free environment. Simulation-based learning can significantly reduce the learning curve associated with new transcatheter interventions.
The Importance of Specialized Training
Training and collaboration among multidisciplinary teams are essential components in advancing pediatric interventional cardiology. Specialized training programs are pivotal for equipping healthcare professionals with the technical skills and theoretical knowledge required for successful implementation of transcatheter interventions. These programs often include:
- Hands-On Workshops: Practical sessions focus on device manipulation and procedural techniques.
- Simulation Technologies: Advanced simulation systems allow trainees to practice complex procedures in a controlled environment, enhancing their proficiency and confidence.
- Interdisciplinary Learning: Collaborations between cardiologists, anesthesiologists, and nursing staff foster comprehensive understanding and elevate communication, which is critical during procedures.
Enhancing Clinical Practices
Multidisciplinary collaboration is instrumental in optimizing patient outcomes. Several notable benefits include:
- Shared Knowledge: Team discussions enhance decision-making processes, ensuring all aspects of a patient's condition are considered.
- Streamlined Processes: A coordinated approach minimizes procedural delays and enhances efficiency during surgeries.
- Improved Outcomes: Studies have shown that hospitals with collaborative practices see lower complication rates and shorter recovery times.
Future Directions
As the field of pediatric cardiology evolves, the integration of new training methodologies and collaboration frameworks remains vital. Innovations such as telemedicine and online learning platforms can expand access to training for healthcare professionals in remote regions, thereby addressing disparities in care delivery. This concerted effort will ultimately shape a future where transcatheter interventions are safely and effectively implemented, maximizing the benefits for pediatric patients with congenital heart diseases.
Future Directions
The advancement of pediatric transcatheter interventions is poised for exciting developments. As we move forward, key trends are likely to shape this vital field of cardiology.
Continued Innovation
The demand for innovation will drive researchers and manufacturers to enhance device design and functionality. Expect:
- New Materials: The introduction of biocompatible and bioabsorbable materials will further enhance patient comfort and reduce the need for additional procedures.
- Enhanced Imaging Techniques: Integration of advanced imaging technologies, such as real-time 3D echocardiography and artificial intelligence analytics, will refine procedural accuracy and outcomes.
Cost Reduction Efforts
Economic barriers have been a significant hurdle to accessibility. Future efforts may focus on:
- Manufacturing Efficiency: Streamlining production processes to lower costs while maintaining quality will be essential.
- Insurance Reform: Advocating for better coverage options for innovative interventions can alleviate financial pressures on families and healthcare systems.
Conclusion
Over the past decade, pediatric transcatheter interventions have significantly evolved, transforming the standards of care for congenital heart diseases. These advancements have led to a paradigm shift, with procedures now safer and more effective for neonates and infants, thus improving overall patient outcomes immensely. The success rates of interventions like atrial and ventricular septal defect closures have surpassed 90%, with a declining complication rate of around 2-5%.
Efforts must focus on overcoming economic barriers and addressing disparities in care availability, particularly in underserved regions. Future directions in this field should prioritize the integration of personalized therapies and a commitment to collaborative practice, ensuring that advancements benefit all pediatric patients, regardless of their demographic or geographic circumstances.