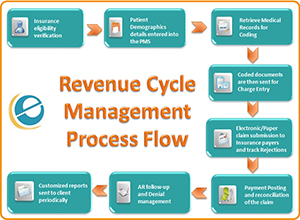
Mastering Revenue Cycle Management in Healthcare: A Strategic Guide for Hospital Leaders

Hospitals need to have effective revenue cycle management (RCM) that will help them to become financially stable and operationally excellent. This article discusses strategic avenues of maximizing healthcare revenue cycle operations by discussing automation, data analytics, and patient-centered practices. It emphasizes the ways hospital leaders can maximize cash inflow, minimize denials, and optimize hospital finance sustainability.
Introduction:
Financial stability in the constantly changing healthcare environment is as important as clinical excellence. Healthcare facilities and hospitals are at the crossroads to ensure quality patient care and the ability to sustain the financial performance. Revenue cycle management (RCM) plays a major role in this scenario. RCM makes sure that healthcare providers are not just solvent, competitive, and efficient in their operations by optimizing financial processes through which patient care is taken care of during registration to the final payment. To the leaders of hospitals, revenue cycle management in healthcare is not just an administration requirement but a strategic requirement.
Understanding Revenue Cycle Management in Healthcare
In its simplest form, revenue cycle management (RCM) is the financial procedure that is adopted by healthcare institutions to administer administrative and clinical operations that deal with patient service revenue. It starts as soon as a patient makes an appointment and goes on to the time the hospital gets the last payment of the services given. The process involves a number of intertwined steps, which include the registration of patients, checking insurances, capture of charges, submission of claims, posting payments, and controlling denials.
Successful healthcare revenue cycle processes demand accuracy and alignment of the departments, which include billing, coding and clinical documentation. Any wastage or malfunction - inaccurate patient information, errors in coding, or missing claims - may lead to loss of claims, wastage of revenue, or legal action. Therefore, in the case of hospital leaders, it is crucial to ensure that the process of RCM is executed as smoothly as possible to ensure the financial stability and the overall patient satisfaction.
The Strategic Importance of RCM in Hospitals
RCM has more significance in hospitals than just collecting revenue. An effectively operated RCM system increases cash flow, decreases claim denials, better adherence to payer conditions and improves relations with patients. With the changes of the reimbursement model to the value-based rather than the volume-based mode of care delivery, hospitals should adopt more strategic management of their financial activity.
Furthermore, the role of RCM is significantly connected to the reputation of the hospital and its efficiency. On-time billing and effective dialogue with patients on their financial obligations assist in improving patient trust. With the current healthcare consumer demands of visibility and online convenience, intensive RCM procedures can assist organizations to compete in an industry.
Regarding leadership, RCM does not simply concern numbers, but rather the investment capability of the hospital in clinical excellence, technology upgrades and development of the workforce. The absence of a powerful RCM structure can make even the most developed medical facilities not grow.
Hospital RCM Strategies for Financial Optimization
Leaders of hospitals who want to enhance their financial performance should treat RCM as a strategic dynamic role. To maximize the results, the use of advanced analytics and automation, as well as training of the workforce, should be part of the strategies of RCM in the hospital. The success factors include the following.
1. Data Accuracy and Integrity
Effective RCM is based on quality data gathering when registering the patient and checking his/her insurance. Mistakes in the demographic or insurance information can be considered one of the most frequent reasons why claims are denied. Hospitals that invest in real-time eligibility checks and automated data validation mechanisms will save a lot of manual errors, enhance the speed of claims incurred, and increase the first-pass solution rates.
2. Automation and Technology Integration
The digital revolution has changed the way healthcare finances are handled. Claim scrubbing, coding validation, and posting of payment are now being used with artificial intelligence (AI) and robotic process automation (RPA) to automate the repetitive tasks. Predictive analytics will be able to recognize the trend of rejected claims, and then act proactively. In the case of hospital leaders, the financial commitment to advanced RCM technology platforms does not only enhance efficiencies but also enables information-oriented decision-making in the long-term of financial optimization.
3. Proactive Denial Management
One of the largest hurdles on the way to the enhancement of hospital cash flow is denied claims. A successful RCM plan includes the determination of the trends in denial, resolving the underlying causes, and the continual communication with the payers. Revenue leakage can be greatly minimised in hospitals that have separate denial management departments. Besides, the use of machine learning models to forecast possible denials at the time of submission will contribute to maximizing revenue recovery and saving on administration expenses.
4. Enhancing Patient Financial Experience
RCM that is patient-centered has become the hall of prominent healthcare organizations. Hospitals with clear prices, clear billing statements and offering multiple options to make payments have an increased patient satisfaction and collection rates. Convenience in which patients can view bills, estimate costs, and make payments through digital portals and mobile applications are becoming helpful in boosting revenue collection rates and building trust.
5. Continuous Staff Training and Process Audits
Regardless of the technological progress, human skills are always at the core of proper revenue cycle management in the healthcare operation. Employees are to be trained on updated codes, payer rules and standards of compliance on a regular basis. Internal audit can be conducted on regular basis to detect any inefficiencies in the process, and risk to compliance and the RCM framework should be made responsive and consistent with the industry best practices.
Leveraging Data Analytics for Financial Performance in Healthcare
With the new hospital system, data is the currency of optimization. The healthcare industry has a high level of financial performance based on data analysis and response to its utilized insights. Any advanced analytics allows the hospital leaders to track such key performance indicators (KPIs) as days in accounts receivable (AR), denial rates, net collection ratios.
The analysis of this information will help decision-makers to see the bottlenecks, predict the trends of revenue, and create specific action plans aimed at enhancing the optimization of finances in a hospital. As an example, predictive analytics can evaluate payment patterns of patients so that hospitals can adjust their collection policies. In the same way, revenue forecasting models may assist the leaders in making wise budgetary choices and allocate resources effectively.
In addition, combining clinical with financial data provides whole picture of the hospital operations. Once leaders are aware of the association between patterns of care delivery and outcomes of reimbursements, they are able to make strategic decisions to enhance the quality of clinical care and financial results.
Navigating Challenges in Healthcare Revenue Cycle
The healthcare revenue cycle is characterized by challenges, although it is a strategic one. Difficulty in the complex payer regulations, increased administrative expenses, staffing issues, and continuous compliance reforms pose constant challenges. Denials of claims have been a common issue, and the root causes are inadequate documentation or wrong coding.
What is more, the shift towards the value-based care models adds a new layer of complexity. Hospitals have become bound to connect reimbursement with patient results and quality measures instead of volume of service. This transformation requires more advanced RCM models that can deal with bundled payments, risk sharing contracts and performance incentives.
There are also major threats of cybersecurity and data privacy. With the digitization of the financial processes in the hospitals, it will be the most important to protect the data related to the hospital and make sure that its laws are enforced, including HIPAA. The violation of the regulations also leads to financial fines, not mentioning that the patients lose trust.
The hospital leaders need to be proactive, technology-oriented, and collaborative in RCM to overcome these issues. Contracting with established vendors of RCM or sourcing of some of its functions can also help the burden of operation and increase the efficiency.
The Link between RCM and Hospital Cash Flow
Maintaining a steady healthcare delivery is maintained by a healthy hospital cash flow. Effective RCM will guarantee that the revenue coloured by services is smoothly flowing within the organization. Any slowness in the filing of claims, high level of denials, or even ineffective collection procedures can put strain on liquidity which will impact on payroll up to procurement.
In comparison, an optimized RCM system reduces the revenue realization time and increases operational flexibility. This liquidity can be invested back by hospitals in the key areas like technology, infrastructure upgrades and staff development. Simply put, RCM has a direct impact on the ability of a hospital to become innovative and provide high-quality patient care.
Furthermore, as there is a growing pressure on financial disclosure, now more than ever, investors and regulators are looking over the shoulders of hospitals in terms of financial viability. Good RCM is financially prudent enhancing institutional credibility and sustainability.
The Future of Revenue Cycle Management in Healthcare
The healthcare of the future, regarding the evolution of a healthcare revenue cycle management system, will be determined by automation, interoperability, and patient empowerment. The merging of the electronic health records (EHRs) and RCM systems will keep improving, establishing a more efficient data exchange between the clinical and the financial departments.
Artificial intelligence will be beneficial in automating previous authorizations, forecasting refusal, and tailoring billing to patients. In the meantime, the blockchain technology can become a safe way of handling multifaceted payer contracting and avoiding fraud.
The other trend is the increasing consumer driven healthcare. Patients continue to desire the same digital convenience when paying healthcare that they are enjoying in retail or banking. Hospitals that can leverage their RCM systems to accommodate these anticipations, by offering clear pricing, online wallets and options of payment, will be competitive.
Lastly, healthcare finance sustainability will be determined by the vision of leadership. Hospital leaders, who perceive RCM as a strategic operation and not an operation in the back office, will be in a better position to overcome the economic uncertainties and regulatory changes.
Building a Culture of Financial Excellence
Being an expert in RCM means more than technological expertise it needs to be a culture of financial responsibility and cooperation. Hospital leaders should create the atmosphere in which all departments are aware of the influence of their position on the revenue integrity, including the front desk staff as well as clinicians.
Interdepartmental cooperation between clinical and administrative and finance teams is determined to make sure that the documentation of care is congruous with the billing codes and payer demands. Sense of ownership among employees can also be achieved by making leadership transparent and monitoring their performance.
Besides this, the organization should incorporate the idea of continuous improvement into its DNA. The RCM process is dynamic and aligned with the future because of the routine analysis of performance, comparison with the standards of the industry, and the adoption of innovative technologies.
Conclusion
Healthcare revenue cycle management is much more than a financial operation - it is the sustenance of the hospital. With the healthcare sector under increasing regulatory, technological, and consumer pressure and demands, hospital leaders should focus on RCM as an element of operational excellence.
With the use of data analytics, automation, patient-centered care, and continuous improvement culture, hospitals can attain financial results in healthcare that will facilitate its mission of providing quality care. When it comes to mastering RCM, leaders do not only protect the financial well-being of their organization but also provide it with the capabilities to succeed in the competitive, value-oriented healthcare landscape.
The bottom line is that RCM success is not a matter of mastering each of the individual processes - it is a matter of coordinating them to create a sustainable, smart, and patient-centered system that remains financially sound and clinically excellent.