Navigating Healthcare Policy and Regulation: Aligning Governance with Operational Excellence
-(1)-(1).jpg)
Healthcare institutions operate within increasingly complex policy and regulatory environments. For hospital leaders, understanding, navigating and leveraging this environment is no longer optional it is central to sustainable success. This article explores the key policy and regulatory frameworks influencing hospital operations today, examines how these regulations impact clinical, financial and operational performance, and outlines strategic responses for hospital-managers to embed compliance and governance into everyday practice. Emphasis is placed on the Indian context but with global relevance, aligning regulation with quality, access and economic objectives.
Introduction
As healthcare systems evolve, the interplay between policy, regulation and hospital operations becomes ever more critical. Regulatory frameworks shape everything from facility licensing and clinical standards to reimbursement, patient rights and environmental compliance. Hospitals that succeed in embedding regulatory awareness and governance into their strategy gain a competitive advantage, operational resilience and risk mitigation. Conversely, weak regulatory alignment creates financial, reputational and legal risk. For executives and healthcare professionals, understanding the regulatory terrain is a strategic imperative.
1. The Regulatory Landscape: Scope & Significance
Regulation in healthcare covers diverse domains: facility licensing, accreditation, patient safety, data protection, insurance and reimbursement, pricing, environmental standards, and public–private partnerships. In India, for example, the Clinical Establishments (Registration and Regulation) Act, 2010 mandates registration of clinical establishments and sets minimum standards. The regulatory architecture is layered: central‐government policy sets broad direction while state governments implement many regulations, since “public health” falls under the State List in India’s constitution.
From a hospital management perspective, regulation is not simply a compliance burden it is a structural framework that shapes strategy, operational models, and resource allocation. Accreditation, licensing, reimbursement approval and regulatory oversight all have direct implications on cost, revenue, care quality and institutional reputation.
2. Key Policy Frameworks and Their Impact
2.1 National Health Policy and Systemic Goals
The National Health Policy 2017 (NHP 2017) articulated India’s ambition for “universal access to good quality health care services without anyone having to face financial hardship”. For hospitals, this translates into pressure to deliver better quality, increase coverage and demonstrate accountability. The policy emphasises prevention, health promotion and an integrated care approach.
2.2 Accreditation and Quality Regulation
Hospital accreditation (for example, via the National Accreditation Board for Hospitals & Healthcare Providers, NABH) has become a regulatory differentiator. Accreditation aligns standards in patient safety, governance and processes. Accreditation or equivalent status increasingly features in government empanelment or insurance schemes, thus affecting referral networks and revenue flows.
2.3 Pricing and Reimbursement Regulation
Regulation of package rates, tariffs and insurance claims has become salient. For instance, in India, revisions to the Central Government Health Scheme (CGHS) procedure rates demonstrate the regulatory anchor for reimbursement. An effective hospital strategy must account for regulatory decisions on pricing, which shape revenue sustainability, especially for private providers.
2.4 Public–Private Partnership (PPP) and Empanelment Regulation
Healthcare policy increasingly favours public–private partnerships and empanelment of private hospitals under government insurance schemes. For hospitals, successful PPP participation depends on regulatory compliance, transparency, patient safety standards and process alignment.
2.5 Regulatory Reform for Digital Health and Insurance Oversight
Emerging regulation covers digital health (telemedicine, e-health records), claims oversight and health information exchange. For example, steps to bring the national claims portal under tighter oversight aim to curb cost inflation in hospital services. Hospitals must monitor such regulatory shifts as they affect workflow, IT systems, and reimbursement risk.
3. Why Regulation Matters: Operational and Economic Imperatives
3.1 Risk Mitigation & Governance
Non-compliance can lead to licence suspension, certified status revocation, financial penalties or loss of empanelment. Operational disruption and reputational damage follow quickly. Strong governance frameworks enable proactive risk identification and regulatory alignment.
3.2 Cost Containment and Operational Efficiency
Regulations often set minimum standards for processes (e.g., waste management, environmental norms, and patient safety). Meeting these standards may require investment, but delays or non-compliance often results in higher long-term costs. Efficient regulatory integration into operations yields cost-efficient compliance and better outcomes.
3.3 Revenue Protection and Growth
Regulatory frameworks determine eligibility for insurance empanelment, state contracts, accreditation incentives and ability to attract international patients. For example, accreditation status or compliance with state empanelment rules directly influences hospital revenue streams.
3.4 Quality, Access and Reputation
Regulation ensures baseline standards for patient safety, care quality and access factors increasingly visible to patients, payers and regulators. Hospitals with strong regulatory compliance and transparency build reputation, patient trust and market differentiation.
4. Strategic Response: Embedding Regulatory Intelligence
4.1 Regulatory Intelligence and Monitoring Function
Hospitals should establish a regulatory intelligence cell monitoring updates in central/state law, insurance rules, accreditation criteria and environmental norms. This cell tracks regulatory trends, assesses risk/opportunity implications and advises senior leadership on compliance strategy.
4.2 Strategic Compliance Roadmap
Develop a compliance road map aligned with institutional strategy: prioritise high-impact regulations (e.g., accreditation renewal, empanelment criteria, and digital health regulations), set timelines, allocate ownership and link compliance to operational planning and budgets.
4.3 Integration with Operational Governance
Regulation should not live in a silo. Compliance must be integrated into operational governance—clinical pathway design, quality improvement, IT systems, procurement, facilities management and human resources. For example, accreditation renewal becomes part of the annual strategic plan, with cross-departmental accountability.
4.4 Data and Digital Infrastructure
Regulatory requirements increasingly require data reporting (patient outcomes, safety incidents, audit logs, claims data). Hospitals should invest in robust hospital information systems (HIS), digital dashboards and analytics infrastructure so that regulatory reporting aligns with operational data flows, avoiding duplication and manual burden.
4.5 Training, Culture and Stakeholder Engagement
Compliance depends on culture, not just systems. Hospitals must train staff in regulatory standards, embed regulatory awareness into routine processes (clinical, managerial and support services) and communicate the operational relevance of regulation (not just as a ‘box-ticking’ exercise). Stakeholders (clinicians, nurses, administrators) must appreciate how regulatory alignment supports quality, access and institutional viability.
5. Case Study: Regulatory Alignment in a Women & Child Specialty Hospital
A women-and-child specialty hospital, for instance, may face multiple regulatory dimensions: licensure of maternity services, NICU standards, paediatric ICU accreditation, and insurance empanelment for maternal child schemes, digital health compliance, biomedical waste, and environmental norms. Effective management involves:
- Mapping applicable regulations (national and state) for maternity, NICU, paediatrics and diagnostics.
- Ensuring accreditation (e.g., NABH) and using accreditation status as a strategic differentiator for empanelment and insurance networks.
- Aligning empanelment criteria for national insurance schemes (e.g., under the Pradhan Mantri Jan Arogya Yojana/PM-JAY) with institutional strategy: quality, access, cost management.
- Leveraging digital health regulation (tele-paediatrics, remote antenatal counselling) to expand access in rural catchments, thus aligning with policy goals of universal access while creating operational efficiency and new referral pipelines.
- Monitoring reimbursement and regulatory changes (for example, hospital package rates, empanelment rules or claims oversight) to ensure financial viability.
By embedding regulatory strategy into the hospital’s management framework, the institution ensures compliance, enhances reputation, expands access and maintains financial sustainability.
6. Emerging Regulatory Trends and Hospital Implications
6.1 Value-based Care Regulation
Globally, regulatory frameworks are shifting from volume-based to outcome-based models. Hospitals must monitor policies that tie reimbursement to outcomes, patient experience and quality indicators. While India is still evolving in this space, awareness and preparedness will become crucial.
6.2 Digital Health and Data Regulation
Policies governing telemedicine, health data protection, interoperability and digital claims processing are evolving rapidly. Hospitals must ensure compliance with data privacy laws (e.g., Personal Data Protection Bill in India), engage with national digital health architecture (such as the Ayushman Bharat Digital Mission), and integrate digital workflows in a regulatory-compliant manner.
6.3 Environmental, Social and Governance (ESG) Regulation
Hospitals increasingly face regulation around environmental management (waste, emissions, resource consumption). For example, environmental action plans imposed by regulatory bodies demand hospitals contribute to pollution control and sustainable operations. Hospitals should treat ESG as a regulatory and strategic pillar.
6.4 Insurance and Claims Oversight Reforms
Governments are tightening oversight of claims, tariffs and provider behaviour to control cost escalation. For instance, the plan to bring the national health claims portal under regulatory oversight signals that hospitals will face increased scrutiny on billing practices. Hospitals should strengthen audit, documentation and compliance mechanisms.
6.5 Accreditation and Quality Mandates for Scheme Eligibility
Empanelment under national schemes increasingly mandates accreditation or higher quality benchmarks. For example, hospitals without required accreditation may be de-empanelled, affecting access to public insurance programmes. Hospital leadership must prioritise accreditation as strategic infrastructure.
7. Practical Implementation: Checklist for Hospital Leaders
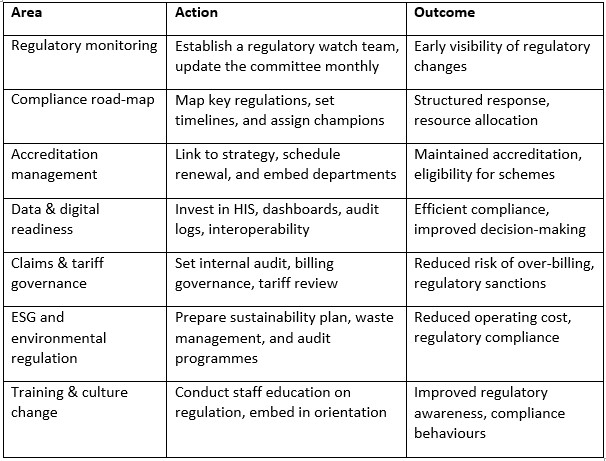
8. Challenges and Risk Factors
While regulatory alignment offers significant benefits, hospitals face challenges:
- Regulatory complexity: overlapping central and state laws may create ambiguity and administrative burden.
- Implementation lag: many regulations are enacted but not yet fully supported by rules, resources or enforcement frameworks.
- Cost burden: compliance often demands upfront investment (IT systems, accreditation processes, and audits) and ongoing resource allocation.
- Rapid evolution: digital health, insurance reforms and ESG regulations are evolving quickly, requiring agility.
- Balancing innovation and regulation: hospitals must innovate while maintaining regulatory compliance not always an easy balance.
Hospital leaders must therefore adopt not just a compliance mentality but also a strategic governance mindset, anticipating regulation, investing in infrastructure and aligning regulation with institutional purpose and performance.
9. Policy Influence and Advocacy
Hospitals are not simply regulated entities; they are stakeholders and contributors to policy development. Leaders in healthcare institutions should engage in policy dialogue, collaborate with industry associations, contribute to consultation processes and advocate for practical and balanced regulation. Through active participation, hospitals can help shape regulatory frameworks that support both quality care and institutional sustainability.
10. The Future Outlook
Policy and regulation in healthcare will increasingly emphasise integrated care, outcome-based reimbursement, digital health governance, patient rights and sustainability. Hospitals that proactively integrate regulatory intelligence with strategic planning will lead. Key areas of focus will include:
- Data-driven regulatory compliance (real-time dashboards, benchmarking outcomes)
- Interoperable digital health ecosystems aligned with national architecture
- Accreditation as a cornerstone of access to national schemes and international partnerships
- Sustainable operations embedded in regulatory compliance and organisational strategy
- Outcome-aligned reimbursement frameworks, moving hospitals from volume to value
In this future, regulation will not be a gate-keeper but a partner of operational excellence, enabling hospitals to deliver better care, reach more patients, and remain economically viable.
Conclusion
Effective governance of healthcare policy and regulation is no longer a peripheral function—it is central to the strategic operations of contemporary hospitals. Regulation shapes access, quality, cost and sustainability. For hospital executives and healthcare managers, the challenge is to move beyond compliance as burden, and embrace regulation as enabler of operational excellence, risk mitigation and sustainable growth. By embedding governance, digital readiness, accreditation and culture of regulatory awareness into strategy, hospitals position themselves to deliver not only safe, high-quality care but also equitable access and sound economics.
The institutions that thrive will be those that recognise regulation as a strategic instrument not merely a cost centre and weave it into every dimension of clinical, operational and financial strategy.
Reference:
- .https://en.wikipedia.org/wiki/Clinical_Establishments_%28Registration_and_Regulation%29_Act%2C_2010?utm_source=chatgpt.com
- https://www.legal500.com/developments/thought-leadership/code-of-care-an-overview-of-indias-key-healthcare-laws/?utm_source=chatgpt.com
- chrome-extension://efaidnbmnnnibpcajpcglclefindmkaj/https://www.mohfw.gov.in/sites/default/files/9147562941489753121.pdf?utm_source=chatgpt.com
- https://en.wikipedia.org/wiki/National_Accreditation_Board_for_Hospitals_%26_Healthcare_Providers?utm_source=chatgpt.com
- https://timesofindia.indiatimes.com/city/chandigarh/ahpi-welcomes-revision-of-cghs-package-rates/articleshow/124297378.cms?utm_source=chatgpt.com
- https://timesofindia.indiatimes.com/city/delhi/green-plan-in-place-for-hospitals-to-take-on-pollution-congestion-ngt-told/articleshow/125065507.cms?utm_source=chatgpt.com
- https://timesofindia.indiatimes.com/city/bhopal/50-ayushman-hosps-face-de-empanelment-with-nabh-caveat/articleshow/124219848.cms?utm_source=chatgpt.com