Is Public-Private Partnership the Key to Reviving Dying Public Healthcare?
-(1).jpg)
The article shall explore whether Public-Private Partnerships (PPPs) can revive struggling public healthcare systems. It will take cues from global case studies, benefits like capital infusion and efficiency, and challenges, including equity and oversight. Finally, arguing that PPPs are not a cure-all, however, they can be effective tools when designed with public interest, accountability, and outcomes in mind.
The Patient in Crisis
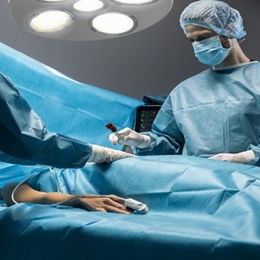
Walk into a district hospital in many low- and middle-income countries and you will find peeling paint, decades-old equipment, and a queue so long that the sick arrive before dawn just to be seen before dusk. Even in relatively better-off regions, the headlines point to overcrowded facilities, stretched staff, and underfunded infrastructure. Public healthcare, the social contract that promises care according to need rather than ability to pay, is visibly ailing.
Against this backdrop, public-private partnerships (PPPs) are being prescribed as the revitalising tonic. From India’s outsourced diagnostics to Turkey’s gleaming city hospitals and Canada’s LEED-certified healthcare infrastructure, the model seems to promise fresh capital, modern technology, and managerial agility—without fully privatising a public good. Yet critics warn of hidden costs, two-tier care, and the slow hollowing-out of public capacity.
Can PPPs revive the system, or do they simply mask deeper issues? This article explores the global evidence with a contextual eye for India’s policy and operational landscape.
Diagnosing the Malaise: Why Public Healthcare is struggling
Before prescribing a remedy, we must understand the disease. Four critical stress points stand out:
- Under-investment: Decades of deferred capital expenditure have left many public facilities unsafe and under-equipped. India’s infrastructure gaps are mirrored in NHS backlogs in the UK, which grew from £4 billion in 2012 to £11.6 billion in 2023.
- Rigid procurement and HR systems: Bureaucratic bottlenecks often mean MRI machines remain idle due to a lack of trained radiographers—common to Indian district hospitals and NHS trusts alike.
- Technology lag: Telemedicine, AI triage tools, and digital health records have proliferated in India’s private sector and global health systems, leaving public counterparts lagging.
- Fiscal pressures: Pandemic recovery, demographic shifts, and competing development priorities squeeze health budgets across emerging and developed economies alike.
PPP 101: What Does It Actually Mean in Healthcare?
A PPP is a structured collaboration between the public sector and private partners where roles, risks, and rewards are clearly defined. The model spans a spectrum:
- Service-only PPPs: Outsourcing specific services such as labs, dialysis, or ambulance fleets. Maharashtra has implemented this across 22 MRI and 31 CT sites.
- Design-Build-Finance-Maintain (DBFM): The private party builds and maintains the facility while the government pays an annual fee. Canada's Abbotsford Regional Hospital is a case in point.
- Design-Build-Finance-Operate-Transfer (DBFOT): The private partner handles full operations along with infrastructure development, as seen in Turkey’s Başakşehir City Hospital and proposed models in India.
- Digital-first PPPs: Private tech platforms integrated into national health schemes. Rwanda’s Babyl platform handles over 5,000 e-consults daily.
Why Governments Are Turning to PPPs
1. Capital without Upfront Burden: Countries like Côte d’Ivoire and India are using PPPs to expand diagnostics without immediate fiscal outlay. This enables facility upgrades while staying within budget limits.
2. Improved Efficiency and Speed: Performance-linked payments, fixed timelines, and private-sector accountability can accelerate project execution. Canada’s PPP hospitals and Indian diagnostic centres alike have demonstrated this.
3. Tech Integration: Rwanda and India are leveraging PPPs to introduce AI-enabled consultations and mobile diagnostics far faster than typical public-sector rollouts.
4. Bridging Service Gaps: India’s state-level diagnostic PPPs, like those in Delhi, Punjab, and Maharashtra, have significantly reduced wait times and brought services to Tier-2 and Tier-3 towns.
Case Studies from the Field
Turkey:
City Hospitals Programme - Başakşehir Çam-Sakura, opened in May 2020 with 2,682 beds, exemplifies scale and modernity delivered through a PPP model. However, clinical integration and long-term adaptability remain areas of concern.
Canada:
Abbotsford Regional Hospital - Launched under a DBFM contract, the hospital met LEED environmental standards and opened on time. Oversight mechanisms tied payments to uptime and availability rather than simply capital inputs.
India:
Diagnostics PPPs - States like Maharashtra and Chandigarh have successfully outsourced imaging and dialysis services. In Chandigarh, wait times for MRI dropped to zero post-PPP.
Rwanda:
A Digital Leap - The Babyl platform integrates AI triage, e-prescriptions, and mobile payments with national insurance, expanding rural access dramatically.
Côte d’Ivoire: In Progress - A PPP aimed at modernising diagnostics across 14 hospitals includes risk-sharing and KPIs—potentially a replicable model for Indian states.
Lessons from the UK: When PPPs Go Wrong
The UK’s Private Finance Initiative delivered over 50 hospitals but left taxpayers with a £160 billion repayment burden. Key concerns included:
- Rigid Contracts: Adapting facilities to evolving care models proved costly.
- Opaque Profits: Refinancing gains benefitted private investors disproportionately.
- Crowded-Out Spending: High annual repayments left less room for staff and equipment.
India can learn from these pitfalls by ensuring better contract design, performance auditing, and public transparency.
Designing a "Health-First" PPP: Five Key Principles
- Outcome-Based KPIs: Link payments to infection rates, turnaround time, and triage, not just bed availability.
- Balanced Risk Transfer: Allocate construction risk to private players, share epidemiological risk, and absorb tariff risk within the government.
- Tariff Transparency: Publish shadow-tariff and subsidy frameworks to build public trust.
- Built-in Flexibility: Include five-yearly review clauses to allow EMR upgrades or new service models.
- Independent Oversight: Use third-party audits, dashboards, and grievance systems akin to Chandigarh’s MRI PPP model.
Are PPPs Equitable?
Equity concerns are valid, but not insurmountable.
- Rwanda’s digital PPP expanded rural access.
- UK PFIs didn’t restrict access but increased financial pressure.
- India’s diagnostics PPPs offer free services at point-of-care—if reimbursements are timely.
Contract design, not ownership structure, ultimately determines equity outcomes.
The Bigger Picture: PPPs in Global Health Finance
The WHO and World Bank’s Health Impact Investment Platform (2024) aims to mobilise €1.5 billion into primary care using blended finance, including PPPs.
Given India’s fiscal constraints post-COVID, such mechanisms offer a pragmatic avenue to scale high-impact services like radiology, dialysis, and tele-triage.
Conclusion: Is PPP the Right Prescription?
PPPs are neither magic bullets nor Trojan horses. When well-conceived, they can inject capital, discipline, and innovation. But they are not substitutes for core public funding, stewardship, and universality.
Used wisely, PPPs in India can:
- Build radiotherapy bunkers, not replace vaccination drives.
- Expand digital triage, not fragment emergency care.
- Improve operations, not undermine equity.
Health leaders should ask:
- What gap am I plugging with this PPP?
- Will the contract protect the vulnerable and remain affordable?
- Can I monitor it effectively
If yes, PPPs can revive ailing public healthcare. If not, they risk becoming expensive distractions from deeper reform.