The Vital Role of Rehabilitation in Recovery after ICU Discharge

Recovering after an ICU stay can be challenging for many patients, as they often face physical, cognitive, and emotional struggles. Rehabilitation is essential in helping patients regain their strength and confidence, making it easier for them to return to daily activities. Key areas of focus in rehabilitation include physical recovery through exercises, cognitive support and addressing emotional and social reintegration challenges.
Introduction
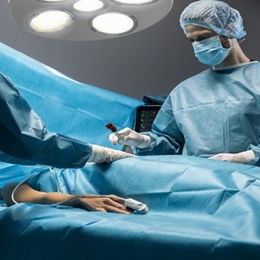
Surviving a stay in the Intensive Care Unit (ICU) is a significant milestone, but for many patients, the real challenge begins after they leave. The journey to full recovery can be long and demanding, often accompanied by lingering physical, mental, and emotional struggles. This is where rehabilitation plays a crucial role, helping individuals regain their strength, confidence, and independence. A well-structured rehabilitation plan tailored to individual needs can make a world of difference in improving quality of life and easing the transition back to daily activities.
Understanding the Impact of an ICU Stay
A prolonged ICU stay can take a toll on the body and mind. Many patients experience a condition called Post-Intensive Care Syndrome (PICS), which includes:
Physical challenges: Muscle weakness, fatigue, reduced mobility, and difficulty performing routine activities.
Cognitive difficulties: Memory problems, confusion, trouble concentrating, and slowed mental processing.
Emotional struggles: Anxiety, depression, and post-traumatic stress disorder (PTSD), which may affect overall well-being.
These complications can make it difficult for patients to return to their pre-ICU lives, underscoring the need for a comprehensive rehabilitation plan that addresses not only physical recovery but also emotional and social reintegration.
Essential Components of Post-ICU Rehabilitation
a. Physical Recovery and Strength Building
Many patients experience muscle loss and extreme fatigue after an ICU stay, making it difficult to perform daily activities.
Rehabilitation focuses on progressive exercises, including light resistance training, balance exercises, and endurance-building activities.
Breathing exercises and pulmonary rehabilitation help those recovering from respiratory distress or prolonged ventilation.
b. Cognitive and Mental Health Support
Brain fog, difficulty concentrating, and memory lapses are common post-ICU issues that require targeted interventions.
Activities like puzzles, reading, and structured mental exercises can help improve cognitive function.
Counselling and therapy provide crucial support for patients dealing with anxiety, depression, or PTSD.
c. Emotional and Social Reintegration
The emotional and social aspects of recovery are just as important as physical and cognitive rehabilitation. An ICU stay can be a traumatic experience, leaving patients with emotional scars and challenges in reintegrating into their social lives.
Emotional Impact of an ICU Stay
Patients often face emotional challenges such as:
Anxiety and Fear: Worries about health, fear of relapse, or returning to the hospital.
Depression: Feelings of sadness, hopelessness, or lack of motivation.
PTSD: Flashbacks, nightmares, or intrusive thoughts related to the ICU experience.
Grief and Loss: Frustration or anger over lost abilities or independence.
Social Reintegration Challenges

Patients may struggle with:
Stigma and Misunderstanding: Feeling judged or misunderstood by others.
Loss of Social Roles: Difficulty resuming roles as parents, partners, or employees.
Isolation: Withdrawing from social activities due to physical or emotional struggles.
Relationship Strain: Stress on relationships with family or caregivers.
Strategies for Emotional and Social Reintegration
To address these challenges, rehabilitation plans should include a variety of strategies tailored to the patient’s unique needs. Emotional and social reintegration is a multifaceted process that requires a combination of professional support, peer interaction, and family involvement. Below are detailed strategies to support this critical aspect of recovery:
Counselling and Therapy
Professional mental health support is essential for helping patients process their ICU experience and address emotional challenges.
Individual Therapy: One-on-one sessions with a psychologist or counselor can provide a safe space for patients to express their feelings, work through trauma, and develop coping mechanisms. Therapists can help patients reframe negative thoughts, manage anxiety, and build emotional resilience.
Cognitive Behavioural Therapy (CBT): CBT is particularly effective for addressing anxiety, depression, and PTSD. It helps patients identify and change negative thought patterns and behaviours that may be hindering their recovery.
Trauma-Focused Therapy: For patients experiencing PTSD, specialized therapies such as Eye Movement Desensitization and Reprocessing (EMDR) can help reduce the intensity of traumatic memories and promote emotional healing.
Support Groups and Peer Counselling
Connecting with others who have had similar experiences can be incredibly empowering for ICU survivors.
ICU Survivor Support Groups: These groups provide a platform for patients to share their stories, challenges, and successes. Being part of a community that understands their struggles can reduce feelings of isolation and provide hope and encouragement.
Peer Mentorship: Pairing patients with ICU survivors who have successfully reintegrated into their lives can offer practical advice and emotional support. Peer mentors can serve as role models, demonstrating that recovery is possible and helping patients navigate the challenges they face.
Family Education and Involvement
Families play a crucial role in the recovery process, but they also need support to understand the patient’s emotional and physical challenges.
Family Counselling: Counselling sessions that include family members can improve communication, address misunderstandings, and strengthen relationships. Families often need guidance on how to provide emotional support without becoming overwhelmed.
Caregiver Training: Educating caregivers about the emotional and social challenges of recovery can help them provide better support and avoid burnout. Caregivers need to learn how to balance their own well-being with the demands of supporting a loved one.
Gradual Social Reintegration
Reintegrating into social life is a gradual process that requires patience and support.
Setting Realistic Goals: Patients should be encouraged to set small, achievable social goals, such as attending a family gathering, reconnecting with a friend, or participating in a community event. These small steps can build confidence and reduce anxiety about social interactions.
Community Engagement: Participating in community activities, hobbies, or volunteer work can help patients regain a sense of purpose and belonging. Engaging in activities they enjoy can also improve mood and overall well-being.
Workplace Reintegration: For patients returning to work, a phased approach with accommodations can ease the transition and reduce stress. Employers should be educated about the patient’s needs and encouraged to provide a supportive work environment.
Holistic Approaches
Holistic therapies can complement traditional rehabilitation methods and support emotional healing.
Mindfulness and Relaxation Techniques: Practices such as meditation, yoga, or deep breathing exercises can help patients manage anxiety, reduce stress, and improve emotional resilience. These techniques can be easily incorporated into daily routines.
Creative Therapies: Art, music, or writing therapies provide an outlet for expressing emotions and processing trauma. These therapies can be particularly helpful for patients who struggle to articulate their feelings verbally.
The Role of Healthcare Providers
Healthcare providers, including doctors, nurses, and rehabilitation specialists, play a key role in facilitating emotional and social reintegration.
Early Screening: Identifying patients at risk of emotional or social challenges early in the recovery process allows for timely interventions.
Personalized Care Plans: Tailoring rehabilitation plans to address the unique emotional and social needs of each patient ensures that they receive the support they need.
Collaboration with Mental Health Professionals: Ensuring that patients have access to psychologists, psychiatrists, or counsellors as part of their recovery journey is essential for comprehensive care.

Challenges in Post-ICU Rehabilitation
While rehabilitation is essential, there are obstacles that may hinder recovery:
Lack of Awareness: Many patients and families are unaware of the long-term effects of an ICU stay and the importance of rehabilitation.
Limited Resources: Access to specialized rehabilitation services may be challenging in some regions.
Financial Constraints: The cost of therapy and medical support can be high, making it difficult for some patients to receive the care they need.
Patient Motivation and Compliance: Long-term rehabilitation requires commitment, and some patients struggle with motivation or adherence to therapy plans.
Conclusion
Recovering from a critical illness is more than just leaving the ICU; it is about regaining one’s strength, independence, and quality of life. Rehabilitation is a crucial part of this journey, addressing physical, cognitive, emotional, and social challenges. A holistic approach involving physiotherapy, mental health support, and social reintegration can help ICU survivors rebuild their lives. Awareness, access to resources, and strong family and community support are key to ensuring that every patient has the opportunity for a full and meaningful recovery. By prioritizing emotional and social reintegration alongside physical and cognitive recovery, we can help ICU survivors not only survive but thrive after their ICU experience.

.jpg)
.jpg)