Telehealth 2.0: Why Remote Patient Monitoring is the Next Big Opportunity for Clinics and Device Vendors

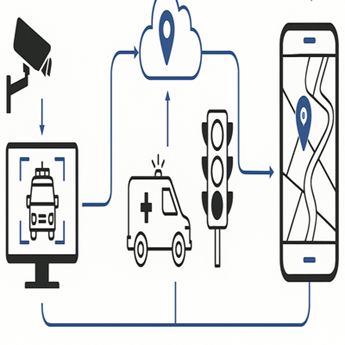
Remote Patient Monitoring (RPM) is transforming the process of healthcare delivery so that clinics and hospitals can deliver care continuously in a data-driven fashion out of the context of traditional settings. Telehealth 2.0 combines AI, IoT-based devices, and cloud computing to improve patient outcomes, decrease hospital readmissions, and increase operational efficiency. To device vendors, this change creates an enormous B2B opportunity in the creation of innovative monitoring solutions and scalable healthcare infrastructure.
Introduction: The Evolution of Telehealth
The healthcare environment has been seismically shifting within the last ten years, but this process was boosted by the pandemic around the world. What initially emerged as a very simple type of video conferencing, telehealth has evolved into a full ecosystem that supports remote and sustained interaction with a patient. Telehealth 2.0 also expands on the episodic model of care, utilizing the data of interconnected devices in order to offer proactive solutions.
In the case of clinics and hospitals, this change is a chance to improve patient outcomes with minimal operating expenses. To device vendors, it provides an expanding market into IoT-enabled devices, analytics platforms, and integration solutions. The intersection of technology and the provision of healthcare is forming a good ground to B2B collaboration.
A. What is Remote Patient Monitoring (RPM)?
The concept of Remote Patient Monitoring (RPM) can be interpreted as digital technologies, the purpose of which is to receive and gather health-related data about patients who have already left the standard healthcare facility and relay patient information to the clinician in order to consider it and act on it. It is based on wearable devices, connected sensors, cloud and analytics software.
Common RPM devices include:
- Smart blood pressure monitors
- Glucose monitoring systems
- Pulse oximeters
- Wearable ECG patches
RPM allows real-time tracking of patients with chronic illnesses, after-surgery and high-risk medical history. RPM will enable healthcare providers to react quickly to abnormalities and modify treatment plans and decrease unnecessary hospital visits by seamlessly integrating into clinic workflows.
B. Business Case for Clinics and Hospitals
The implementation of RPM has several practical and tactical advantages to healthcare providers:
Improved Patient Outcomes
Clinicians can trace the warning signs before the situation gets worse by ensuring that the vital and other health parameters are observed at all times. This is especially required where he or she is required to deal with long-term patients like diabetes or high blood pressure or heart failure.
Operational Efficiency and Cost Savings
Hospitals will be able to decrease the rate of readmissions and avoidable visits to the emergency thus leading to quantifiable savings. In outpatient clinics, RPM will enable the efficient distribution of resources, which will enable employees to pursue other areas of critical care.
Data-Driven Decision Making
RPM gives a rich source of patient data to enable informed decisions by clinicians to rely on trends and predictive analytics, and not just on the intermittent visits to patients in person.
Enhanced Patient Engagement
Patients who have RPM devices are more actively engaged in their care. Connection promotes conformity to treatment regimes and promotes better health behaviors in a virtuous cycle of better results and satisfaction.
These benefits make a strong argument that clinical facilities should invest in RPM technology, and device vendors have a strong sense of demand direction of their products.
C. Opportunities for Device Vendors
At the Telehealth 2.0 revolution are the vendors of devices. Connected health devices are marketed at an accelerated pace due to the need to monitor in real-time and provide data-driven insights.
High-Demand Segments
- Wearable sensors and monitors are known for cardiovascular, metabolic, and respiratory.
- Predictive care AI-based analytics.
- Integration platforms between devices and EHRs, as well as telehealth platforms.
Partnerships and B2B Collaborations
Hospitals, clinics, and telehealth sites can collaborate with those who are selling products to sell integrated solutions. RPM packages, which are customizable with devices, software, and analytics services, are becoming more appealing to healthcare institutions.
Innovation Opportunities
The vendors are able to differentiate their products using the new technologies such as AI-based anomaly detection and predictive alerts. Clinician-friendly dashboards can be applied especially well in decision fatigue mitigation and patient outcomes.
Regulatory and Compliance Considerations
The compliance with healthcare regulations, including HIPAA in the U.S. or CE certification in Europe, is an essential issue among vendors. Compliance also grants credibility with the health encompassing and reduces the adoption speed in clinical setups.
D. Technological Trends Driving RPM
There are various technology trends that are contributing to the development and application of RPM:
Artificial Intelligence & Machine Learning
AI algorithms process their input of incoming patient data to form a pattern, forecast possible health events, and suggest interventions. Machine learning models are improved as time goes on, and predictive performance is improved.
Internet of Medical Things (IoMT)
IoMT links wearables, sensors, and other devices into a single system to have an opportunity to collect data continuously. Such devices give clinicians the ability to track patients in real-time and act proactively.
Cloud & Data Analytics Platforms
RPM tools on clouds provide a smooth data storage, access, and analysis. The Electronic Health Records (EHRs) can be integrated to view the history of patients in a holistic manner and provide a personalized care plan.
Interoperability Challenges
Although the potential of technology is immense, there is still a problem in integrating various devices and software platforms. The B2B healthcare market will be characterized by vendors that offer interoperable, plug-and-play solutions.
E. Challenges and Considerations
As promising as it is, RPM implementation has a number of issues:
Data Security & Privacy
It is best to ensure that the HIPAA, GDPR, and local healthcare policy standards are met. Information leakages may deter trust and adoption.
Patient Engagement and Compliance
The success of RPM relies on the regular use of patients using the devices and adherence to care plans. Solutions by vendors with easy-to-use interfaces and automated reminders enhance compliance.
Integration with Existing Systems
Hospitals and clinics have a tendency to use legacy systems. Interoperability with current EHRs and telehealth systems is mandatory to adopt.
Scalability and Cost
RPM should be scalable to both big and small clinics. The vendors should be able to strike a balance between cost-effectiveness and high functionality to attract a wide B2B market.
F. Future Outlook: Telehealth 2.0 and Beyond
The next stage of healthcare delivery is known as Telehealth 2.0, which dwells upon lifelong care and preventive programs, and active care of a patient. Emerging models include:
- Clinic and hospital-based RPM services through subscriptions.
- Wearable-based and analytics-based preventive care packages.
- Teleconsultations with predictive insights with AI.
The RPM market is expected to rise exponentially in the next five years, with North America, Europe, and Asia-Pacific having the highest prospects of adopting it. The vendors of devices placed to deliver integrated and scalable solutions will get a large portion of the market share.
Digital health ecosystems comprising interconnected devices, cloud computing, and artificial intelligence analytics are altering the nature of how health care is provided, and this has presented a win-win situation between the clinics and the device vendors.
Conclusion
Remote Patient Monitoring has ceased to be an option; it is a strategic necessity for the current healthcare providers. In the case of clinics and hospitals, RPM enhances the overall patient outcomes, cost reduction, and operational efficiency. To the vendors of devices, it is a swiftly growing B2B opportunity to provide creative, combined, and comfortable solutions.
Telehealth 2.0 is preconditioning the future of care, and with the adoption of RPM, the organizations will gain a competitive edge; not only that, they will have the opportunity to change the care delivery systems in the world.
FAQs: Telehealth 2.0 and Remote Patient Monitoring
1. What is the difference between traditional telehealth and Telehealth 2.0?
Video consultations or phone calls are the major forms of traditional telehealth. Telehealth 2.0 involves the use of Remote Patient Monitoring (RPM), AI analytics, and IoT-based devices that allow providing proactive, continuous care beyond the clinical environment.
2. How does RPM benefit clinics and hospitals?
RPM enables medical professionals to track patients and decrease hospital admissions, manage human resources, and enhance patient outcomes, in general. It also offers a method of coming up with improved and data-driven preventive care decisions.
3. What types of devices are used for Remote Patient Monitoring?
Smart blood pressure sensors, wearable ECG patches, glucose sensors, pulse oximeters, and health or fitness trackers are some of the most likely RPMs that are Internet of Things connected. Such devices relay data to clinicians to be constantly examined.
4. Are there regulatory requirements for implementing RPM solutions?
Yes. The clinics and equipment vendors should comply with the privacy and safety laws on data, including HIPAA in the United States, GDPR in Europe, and other local healthcare regulations. The vendors are to certify and verify that the devices and platforms are in line.
5. How can device vendors take advantage of the RPM market?
The vendors can also offer connected devices, analytics dashboards, predictive notices using AI, and hospital and clinic integration solutions. High-value opportunities may be formulated through telehealth platforms and B2B custom solutions.
6. What are the main challenges of adopting RPM?
Challenges encompass the issue of data security, patient engagement and adherence, legacy system integration, and scalability to clinics of various sizes. Remedies that cover these areas of pain are at an advantage.
7. What is the future of RPM in healthcare?
Subscriptions to the RPM services, teleconsultations aided by AI, predictive analytics, and preventive care models are part of the future. The RPM market is starting to grow at a very high rate globally, which gives opportunities to the healthcare providers as well as the device vendors.

.jpg)