Introduction
The emphasis on the importance of knowledge as the new competitive advantage has led to the adoption of knowledge management (KM)in healthcare organisations (Omotayo, 2015; Wills, Sarnikar, El-Gayar and Deokar, 2010). KM has been ascertained as a new management tool which can facilitate healthcare organisations to effectively manage their internal and external knowledge (Omotayo, 2015; Wills, Sarnikar, El-Gayar and Deokar, 2010). It is a discipline that enables healthcare organisations to transform large amounts of medical data into relevant clinical information (Dwivedi, Bali, James, and Naguib, 2001), and to promote sharing of knowledge gained through years of experience among healthcare professionals.
Generally, any KM implementation requires processes such as create, locate, capture, and share knowledge (Alavi and Leidner, 2001). In order for KM processes to function effectively, the right KM strategies and the essential factors of success in implementing KM should be considered. Most KM literature discusses KM processes, strategies and success factors separately. However, this paper addresses the integration of KM processes, strategies and success factors as guides for the successful KM implementation.
Background
Previously, the focus of KM in healthcare was solely on the implementation of technology-based KM for KM processes in healthcare organisations. For instance, Bose (2003) discussed the KM capabilities, the technical infrastructure, and the decision support architecture for healthcare. Besides, Falkman, Torgersson, Jontell, and Gustafsson (2005), argued that IT plays a supporting role in KM processes by using virtual community tools to support collaboration, community building and learning between clinicians and patients. In addition, Dwivedi, Bali and Naguib (2005) pointed out that KM-related tools and technologies could be used to produce Clinical Knowledge Management (CKM) solutions. Koumpouros, Nicolosi, and Martinez-Selles(2006) promote knowledge creation and utilisation by chronic patients through the introduction of a virtual, private, disease-specific patient community called ‘Health Community KM System”. As reported by Davenport, De Long, and Beers (1998) in their study on successful KM projects, any KM initiatives should have a balance between organisational and technological aspects for successful implementation.
As a matter of fact, the current models of successful KM are based on technology-enabled factors. For instance, Hwang, Chang, Chen and Wu (2008) carried out a survey study on the users of KMS in the hospital in Taiwan to assess the perceived value of KMS. With respect to this study, users of KMS were discovered to be voluntary physicians from departments such as clinical departments, infection control, insurance claims, and disease classification. In their job description, they managed to identify these factors as critical to KMS use:perceived usefulness, system quality, and information quality. Besides, Koumpouros et al. (2006), in their studies on KMS in cardiology, mentioned that the quality of knowledge and the use of right terminology are important for doctors when utilising KMS. Additionally, up-to-date and reliable source of knowledge were also essential in the use of KMS. Based on the studies conducted, doctors were shown to exhibit a higher tendency of using such systems if they are user-friendly, easily accessible and practical to their work. Undeniably, the security of the systems, which is closely related to the protection of contributor’s knowledge and the integrity of knowledge, is considered a significant success factor. Based on the survey conducted by Ali, Tretiakov, Whiddett, and Hunter (2017) on physicians in hospitals in New Zealand regarding the factors determining the success of KMS, it was discovered that organisational factors such as leadership and incentives are significant factors for KM success.
The previous models were developed independently from KM strategies and they solely focused on the success factors. In connection with the KM initiatives in healthcare, the integration of KM processes and success factors with KM strategy was proposed to provide a comprehensive overview on the effective implementation of KM.
Theoretical and Conceptual Framework
The primary reason organisations encourage the incorporation of KM efforts into the system is to enable themselves to convert tacit knowledge into explicit knowledge. In this context, the conversion of knowledge will greatly enhance its transferability so that it can be made available to others and reused. These efforts involve several processes that allow firms to recognise, create, transform, and distribute knowledge (Gold, Malhotra, and Segars, 2001). With regards to the healthcare context, KM is defined as a systematic process of capturing, storing, dissemination and reuse of clinical knowledge that can optimise information, collaboration, expertise and experience of healthcare practitioners. Hansen, Nohria and Tierney (1999) described two knowledge management strategies to managing knowledge: codification and personalisation. Codification strategy makes explicit knowledge such as routine cases available to healthcare professionals so that they can reuse and apply knowledge in solution of everyday problems. Personalisation means providing individuals with the tacit knowledge such as creative solutions to solve problems by communication with other experts. For these strategies to be effective, the essential factors of success should be considered.
Proposed Integrated Model for Effective KM
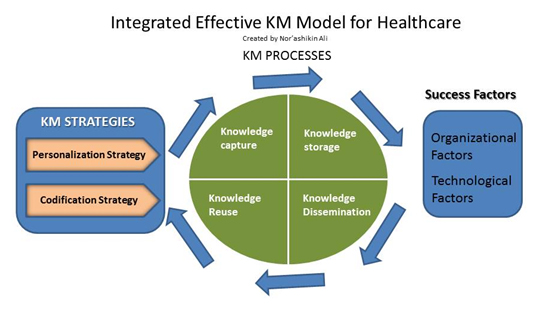
KM Processes
In the process of converting tacit knowledge to explicit knowledge, some processes involved are as follows:
Knowledge capture. First, knowledge capture process is the process of acquiring knowledge from the internal of external sources. In healthcare, knowledge is primarily derived from the sharing of clinical experiences, skills, and know-how while delivering healthcare to patients. Through this interaction between the physician and the patient, knowledge is created and stored in the KMS by the physician. As a matter of fact, methods of capturing can be in various forms including:
1) Use blogs, knowledge portal or knowledge bases
2) Expert directories where the physicians enter their contacts, which are linked to their knowledge afterwards
3) Collaborative virtual workspaces
4) Video sharing, where knowledge is recorded
5) A platform for communities of practice, e.g. electronic discussion forum
6) Structured interview technique.
Knowledge storage. Second, the knowledge that is captured is stored in a knowledge repository. In this context, knowledge in the mind is often difficult to access; thus individuals’ knowledge needs to be acquired and stored so that it is accessible for reuse. Generally, the methods available for storing knowledge are as follows:
1) Knowledge portal
2) Blogs
3) Electronic knowledge repository that contains medical databases, physicians’ experiences
4) Document libraries that keep all documents related to clinical treatment, research articles
5) Evidence-based repository.
Knowledge dissemination. Third, knowledge dissemination involves sharing and transferring of clinical activities or decision making from healthcare practitioners or repository to other practitioners. In this respect, healthcare practitioners are allowed to share their experiences in solving patients’ illness. The importance of sharing culture or dissemination of knowledge was also highlighted by Gagnon (2011) which stated that knowledge must be made available in a readily accessible manner and practical format to whoever needs it in the organisation anywhere and anytime. In this process, the methods used are as follows:
1) Knowledge cafes
2) Workshops
3) Web-based communities of practice
4) Social media
5) Online community
6) Blogs
Knowledge reuse. Fourth, the purpose of KM is to avoid reinventing solutions that are already available in the organisation through reusing knowledge that is stored. In particular, knowledge that is stored and codified can be-reused by other practitioners to solve similar problems encountered with other patients. Significantly, this process of reusing knowledge is time-saving (time taken to source for solutions is significantly minimised or omitted) as it tackles various problems with existing knowledge. In fact, new knowledge can be generated based on the existing knowledge as the current knowledge repository contains algorithms of the symptoms of more than 500 illnesses (Hansen, Nohria, and Tierney, 1999). Most importantly, in this case, healthcare is not inventing a new way to cure diseases since physicians have the privilege of accessing available knowledge to comprehend sophisticated situations. The benefits of this process are:
1) To enable good search engine to retrieve knowledge
2) To improve quality of knowledge
3) To provide platforms for meaningful communication through newsletters, training, websites
4) To promote the use of lessons learned and best practices via push technology.
KM Strategies
In this paper, two knowledge management strategies are proposed for the purpose of sharing explicit and tacit knowledge: personalisation strategy and codification strategy.
Personalisation strategy
First and foremost, a personalisation strategy is a social-organisational approach that employs dialogue, and collaboration as means to disseminate best practices and lessons learned throughout the organisation. This strategy focuses on the transfer of tacit knowledge, which is hard to access in documents. Essentially, it promotes interactions between individuals to communicate ideas and share their expertise. Besides, professionals are also able to obtain knowledge which occasionally cannot be found in the knowledge repository. For instance, this strategy involves a series of conversations among individuals and groups whereby they provide questions, responses, and comments that are difficult to be presented in documents. Similarly, the use of technology such as groupware, online chat, conferencing tools such as video conferencing and teleconferencing can assemble healthcare practitioners simultaneously despite being separated by distance. Indeed, a personalisation strategy is often observed in communities of practice where groups of professionals share similar interests and job roles. To sum up, this strategy promotes generation of new and refined knowledge whereby respective individuals in a group contribute ideas, knowledge and expertise acquired through interaction among group members.
Codification strategy
The codification strategy involves the identification, capture, and indexing of knowledge. This knowledge is later made accessible to professionals who are keen on reusing and applying the relevant knowledge to support routine problem solving. Interestingly, this strategy adopts a ‘people to document, which emphasises on the connection of healthcare practitioners to documents that contain explicit and codified knowledge (Hansen, et al., 1999). Moreover, codified knowledge is accessible in various forms including printed documents and electronic documents (e.g., health portal, software algorithms, clinical practice checklists).For instance, codified knowledge at healthcare organisations includes scientific research outputs, clinical guidelines, and operating manuals (Denis and Lehoux, 2013).Most importantly, the primary goal of this strategy is to enable the re-use of explicit knowledge at a specified time later depending on the user’s need while optimising the accessibility of this knowledge at a widespread level. As a result, this strategy can prevent knowledge loss as well as remove duplication of efforts in looking for solutions that are already available in the organisations.
Success Factors
The success factors are categorised into organisational and technological factors.
Organisational Factors
• The commitment and dedication from top level management are needed to support knowledge management
• Developing a knowledge-oriented culture where trust, openness, and collaboration are being practiced
• Facilitating access to the dissemination of knowledge
• Training programmes
• Establishing monetary and non-monetary incentive systems.
Technological Factors
Efficient and effective information and communication technology (ICT) is a critical enabler for KM. In particular, healthcare organisations must incorporate ICT into their KM initiatives and pay considerable attention towards the following technological factors:
• ICT that enables rapid search, access and retrieval of information, and supports collaboration and communication between organisational members
• ICT that can facilitate KM activities through the codification of knowledge and support interactive forms of communication through the Internet and email
• Effective infrastructure for knowledge management processes
• The simplicity of technology, ease of use, suitability to users’ needs, relevance of knowledge content, and standardisation of a knowledge structure orontology.
Conclusion
In conclusion, it is crucial that healthcare organisations incorporate KM processes, KM strategies, and success factors into their existing system for the successful implementation of KM in healthcare. From this perspective, it is important for KM processes and KM strategies to be addressed in a systematic and structured manner. Clearly, an effective KM model compliments the previous KM success models by integrating the success factors with the KM strategies and processes as fundamental components of KM success model. Essentially, the proposed components can function as a basis for healthcare organisations to evaluate their KM practices.
References
Ali, N., Tretiakov, A., Whiddett, D., & Hunter, I. (2017). Knowledge management systems success in healthcare: Leadership matters. International Journal of Medical Informatics, 97, 331-340.
Birkinshaw, J. (2001). Why is knowledge management so difficult?. Business strategy review, 12(1), 11-18.
Bose, R. (2003). Knowledge management-enabled health care management systems: capabilities, infrastructure, and decision-support. Expert systems with Applications, 24(1), 59-71.
Davenport, T. H., De Long, D. W., & Beers, M. C. (1998). Successful knowledge management projects. Sloan management review, 39(2), 43.
Denis, J. L., &Lehoux, P. (2013). Organizational theories. Knowledge translation in health care: Moving from evidence to practice, 308-319.
Dwivedi, A. N., Bali, R. K., &Naguib, R. N. G. (2006, January). Implications for healthcare knowledge management systems: A case study. In Engineering in Medicine and Biology Society, 2005. IEEE-EMBS 2005. 27th Annual International Conference of the (pp. 5668-5671). IEEE.
Falkman, G., Torgersson, O., Jontell, M., &Gustafsson, M. (2005). SOMWeb-Towards an Infrastructure for Knowledge Sharing in Oral Medicine. Studies in health technology and informatics, 116, 527-532.
Gold, A. H., Malhotra, A. &Segars, A. H. (2001). Knowledge management: An organizational capabilities perspective. Journal of management information systems, 18(1), 185-214.
Hansen, M. T., Nohria, N., & Tierney, T. (1999). What’s your strategy for managing knowledge. The knowledge management yearbook 2000–2001, 1-10.
Guptill, J. (2005). Knowledge management in health care. Journal of health care finance, 31(3), 10-14.
Hwang, H. G., Chang, I. C., Chen, F. J., & Wu, S. Y. (2008). Investigation of the application of KMS for diseases classifications: A study in a Taiwanese hospital. Expert Systems with Applications, 34(1), 725-733.
Koumpouros, Y., Nicolosi, G.L. and Martinez-Selles, M.(2006). Critical success factors for establishing a
multidisciplinary health community KM systemusing internet-based ICTs: the cardiology paradigm.
International Journal of Healthcare Technology &Management, 7(3/4), 1–2.
Omotayo, F. O. (2015). Knowledge Management as an important tool in Organisational Management: A Review of Literature. Library Philosophy and Practice, 1.
Wills, M. J., Sarnikar, S., El-Gayar, O. F., &Deokar, A. V. (2010). Information systems and healthcare XXXIV: Clinical knowledge management systems—Literature review and research issues for information systems.