Navigating Chronic Kidney Disease: Advancements in Diagnosis and Treatment
This article explores recent advancements in Chronic Kidney Disease (CKD) diagnosis and treatment, emphasizing biomarkers, imaging technologies, genetic testing, AI-driven diagnostics, novel therapies, and regenerative medicine. It addresses challenges like underdiagnosis, disparities, and workforce shortages, highlighting the importance of multidisciplinary care and emerging trends in precision medicine and health equity initiatives.
Introduction and Background:
Chronic Kidney Disease (CKD) represents a significant healthcare challenge globally, impacting millions of individuals and posing a substantial burden on healthcare systems. This progressive condition, characterized by the gradual loss of kidney function over time, requires early detection, precise diagnosis, and effective management strategies to mitigate its progression and improve patient outcomes. Recent years have witnessed remarkable advancements in both the diagnosis and treatment of CKD, ushering in new approaches and technologies that offer renewed hope for patients and healthcare providers alike.
Advancements in CKD Diagnosis
Traditional Diagnostic Measures - Diagnosis of CKD traditionally relied on measures such as serum creatinine levels and estimated glomerular filtration rate (eGFR). While these parameters remain fundamental in assessing kidney function, they have limitations, particularly in detecting early-stage CKD.
Biomarkers in CKD Diagnosis - One of the most significant breakthroughs in CKD diagnosis is the utilization of biomarkers. Biomarkers, such as urinary albumin-to-creatinine ratio (UACR), kidney injury molecule-1 (KIM-1), and neutrophil gelatinase-associated lipocalin (NGAL), provide valuable insights into kidney health and can detect kidney damage at earlier stages than traditional markers.
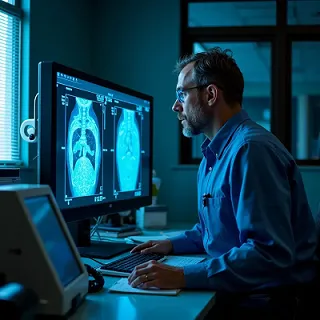
Imaging Techniques for CKD Assessment - Advancements in imaging techniques have also revolutionized the diagnosis and monitoring of CKD. Technologies such as renal ultrasound, computed tomography (CT) scans, magnetic resonance imaging (MRI), and renal scintigraphy allow for detailed assessment of kidney structure, function, and perfusion.
Genetic Testing and Molecular Profiling - Furthermore, genetic testing and molecular profiling have emerged as powerful tools in CKD diagnosis and risk stratification. Genetic factors play a crucial role in the pathogenesis of CKD, particularly in inherited kidney disorders such as autosomal dominant polycystic kidney disease (ADPKD), Alport syndrome, and Fabry disease.
Omics Technologies - The integration of omics technologies, including genomics, proteomics, metabolomics, and microbiomics, has revolutionized CKD diagnosis. These approaches enable a deeper understanding of the molecular mechanisms underlying CKD progression, paving the way for personalized treatment strategies based on individual genetic and biochemical profiles.
Point-of-Care Testing - The development of point-of-care testing devices for CKD biomarkers allows for rapid and convenient monitoring of kidney function in clinical settings or even at home. This accessibility enhances patient engagement and facilitates timely interventions, contributing to better disease management outcomes.
AI-Driven Diagnostics - Artificial intelligence (AI) and machine learning algorithms are increasingly being employed to analyze vast datasets related to CKD biomarkers, patient demographics, and clinical outcomes. These AI-driven diagnostics can identify patterns, predict disease progression, and assist healthcare providers in making more informed treatment decisions tailored to each patient's unique needs.
Advancements in CKD Treatment
Pharmacological Interventions - Pharmacological interventions play a pivotal role in CKD management, with a focus on blood pressure control, glycemic management, and dyslipidemia.
Novel Therapeutic Agents - Moreover, the introduction of novel therapeutic agents, such as sodium-glucose cotransporter-2 (SGLT2) inhibitors, mineralocorticoid receptor antagonists (MRAs), and endothelin receptor antagonists (ERAs), has expanded treatment options and demonstrated promising outcomes in slowing CKD progression and improving cardiovascular outcomes.
Lifestyle Modifications and Dietary Interventions - Complementary to pharmacotherapy, lifestyle modifications, and dietary interventions play a pivotal role in optimizing CKD management.
Advanced Renal Replacement Therapies - Advanced renal replacement therapies (RRT), including hemodialysis, peritoneal dialysis, and kidney transplantation, remain essential interventions for patients with end-stage renal disease (ESRD).
Immunotherapies - Emerging immunotherapies targeting specific pathways involved in CKD pathogenesis show promise in halting disease progression and preserving kidney function. These therapies, including monoclonal antibodies and immune modulators, aim to modulate the immune response and reduce inflammation in the kidneys, thereby slowing the decline in renal function.
Nanotechnology-Based Therapeutics - Nanotechnology-based drug delivery systems offer targeted and sustained release of therapeutic agents directly to the kidneys, minimizing systemic side effects and improving drug efficacy. Nanoparticles, liposomes, and hydrogels designed for renal drug delivery enhance treatment precision and patient compliance.
Telemedicine and Remote Monitoring - The integration of telemedicine platforms and remote monitoring devices enables continuous monitoring of CKD patients' vital signs, medication adherence, and disease progression outside traditional healthcare settings. Teleconsultations with nephrologists and virtual care programs improve access to specialized care, especially in rural or underserved areas.
Multidisciplinary Care and Patient-Centered Approaches
Multidisciplinary Care Models - The integration of multidisciplinary care models, collaborative care teams, and patient-centered approaches is paramount in optimizing CKD management and improving patient outcomes.
Challenges in CKD Management
Underdiagnosis and Delayed Interventions - One of the primary challenges is the underdiagnosis and underutilization of early CKD detection methods, leading to delayed interventions and increased disease burden.
Comorbid Conditions and Polypharmacy - Another challenge in CKD management is the complexity of comorbid conditions and polypharmacy in patients with advanced kidney disease.
Disparities in Access to Kidney Care - Furthermore, disparities in access to kidney care, particularly among underserved populations and minority communities, remain a significant concern.
Cost and Affordability - The high cost of advanced CKD treatments, including dialysis and transplantation, poses financial challenges for patients, healthcare systems, and insurers. Addressing cost barriers through innovative financing models, insurance coverage expansions, and cost-effective treatment protocols is crucial to ensuring equitable access to quality kidney care.
Patient Education and Empowerment - Limited awareness about CKD symptoms, risk factors, and preventive measures among the general population contributes to late-stage diagnoses and suboptimal disease management. Comprehensive patient education programs, community outreach initiatives, and digital health tools empower individuals to proactively manage their kidney health and engage in shared decision-making with healthcare providers.
Workforce Shortages - The growing prevalence of CKD worldwide exacerbates healthcare workforce shortages, particularly in nephrology specialties. Investing in training programs, incentivizing nephrology careers, and adopting team-based care models involving advanced practice providers and allied health professionals can alleviate workforce constraints and improve patient access to comprehensive kidney care services.
Emerging Trends in CKD Management
Artificial Intelligence (AI) and Machine Learning - Looking ahead, several emerging trends hold promise for further advancements in CKD diagnosis and treatment.
Precision Medicine Approaches - Moreover, precision medicine approaches, leveraging genomics, proteomics, metabolomics, and microbiomics data, are poised to revolutionize CKD management.
Biomimetic Kidney Devices and Regenerative Therapies - Biomimetic kidney devices, bioengineering solutions, and regenerative medicine approaches offer innovative avenues for developing bioartificial kidneys, renal tissue engineering, and cell-based therapies for CKD and ESRD.
Bioengineering Solutions - Advancements in bioengineering, including 3D bioprinting and organ-on-a-chip technologies, hold promise for developing bioartificial kidneys and personalized renal tissue constructs. These bioengineered solutions mimic native kidney structures and functions, offering potential alternatives to traditional dialysis and transplantation modalities.
Regenerative Medicine - Regenerative medicine approaches, such as stem cell therapies and tissue engineering techniques, aim to regenerate damaged kidney tissues, repair renal function, and restore kidney health. Clinical trials exploring the safety and efficacy of regenerative therapies in CKD and ESRD patients are underway, marking a transformative shift towards regenerative nephrology.
Health Equity Initiatives - Addressing disparities in CKD prevalence, outcomes, and access to care requires targeted health equity initiatives focused on vulnerable populations, including racial and ethnic minorities, socioeconomically disadvantaged communities, and rural residents. Culturally competent care delivery, community-based interventions, and advocacy for policy reforms are essential components of comprehensive health equity strategies in CKD management.
Conclusion:
In conclusion, while challenges persist, ongoing research, technological innovations, and multidisciplinary collaborations hold tremendous potential for advancing CKD diagnosis, treatment, and patient outcomes. Addressing barriers to early detection, optimizing medication management, addressing health disparities, and embracing emerging trends in precision medicine and regenerative therapies are key priorities in navigating the evolving landscape of chronic kidney disease management.

.webp)