Medical tourism has become an important alternative for patients to get timely treatment and to seek desired medical care in foreign countries. Telemedicine can play a vital role in medical tourism through an evaluation of the involved business processes.
Although it may easily be dismissed as another BPO-like fad, medical tourism is nothing short of a serious business that has the potential to revolutionise the global healthcare industry. It is worth US$ 300–375 million, and growing at a rate of 30 per cent annually (2004 figures). Today, patients are combining vacation with care because either the local treatment is too expensive or involves long waiting periods or both.
Telemedicine is a serious attempt at bridging the gap between the care receivers and providers by making physical distances irrelevant and cutting down on travel. An essential cog in the wheel of medical tourism, it facilitates the patient and the care providers to “know each other” before they meet each other for the first time. It allows all the remote and local care providers to exchange health-related notes on an on-demand basis throughout the duration of the clinical care process beginning from the first encounter, to follow-up sessions until the patient is relieved. Consequently, it increases the efficiency, productivity and attractiveness of medical treatment as a whole and medical tourism in particular.
Telemedicine
The word Telemedicine is a combination of the Greek word ‘Tελε’ (tele) meaning ‘distance’ and the Latin word ‘mederi’ meaning ‘to heal’ and therefore literally means, ‘distance healing’. It is not one specific technology but a means of providing health services from a distance using telecommunications and computer science. It spans every level of healthcare from the first responder or emergency medical systems to tertiary medical speciality consultations to performing invasive and / or surgical procedures delivering home care.
The technology makes it possible to have the ‘right’ information (clinical information) available to the ‘right’ people (patients, care providers, family and friends) at the ‘right’ time (on-demand, during and after the treatment process).
In short, telemedicine is a high-tech solution to the universal problem of access to healthcare irrespective of physical location of the various stakeholders of the clinical care process.
Medical tourism
Medical tourism is a term applied to the process where people from all around the world travel to foreign countries to obtain medical, dental and surgical care. At the same time, it is a tour, a vacation and an experience of visiting them.
Medical tourism companies help organise patients’ treatment, travel arrangements and tours. The modus operandi is to couple the medical treatment with travel and tourism at a fraction of cost incurred in the patient’s own country. This is a great value addition to all concerned. The patient gets relief quickly without compromising on the quality and quantity of care. The healthcare industry earns valuable revenues. The healthcare industry gets invaluable business. The countries where medical tourism is being actively promoted include Greece, South Africa, Jordan, India, Malaysia, Philippines and Singapore.
Medical tourism definitely adds itself to the top-line of the various healthcare institutions. Even though the revenue model is volume-dependent, the capacity and quality of care is enough to ensure healthy profit margins at reduced rates.
Medical tourism business process
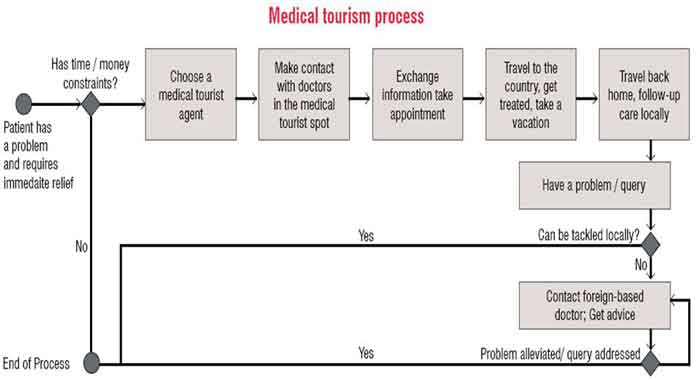
In medical tourism, the basic business process is as follows:
1. A patient residing in an area where he is unable to get relief from his problems due to high treatment costs, long delays in getting the treatment or both, looks for ways and means to get relief as soon as possible at equal or lower cost
2. Patient decides to travel to a place where the cost of comparable quality and quantity treatment is same or less and is readily available
3. A competent care provider at an institution of patient’s choice located in
a foreign country reviews patient’s case records and gives an appointment.
4. The patient then travels to the country where the institution is located and receives the treatment
5. Pre- or post-treatment, patient conducts some sightseeing according to his choice (and budget), and then at the termination of his visit travels back to his country with all his treatment records and post-treatment advice to his primary care physician
6. For follow-ups required at his place of residence, patient is provided with instructions regarding how these actions need to be undertaken
The most important decision point being both the quality and quantity of care ensure patient safety while providing the best of care available anywhere.
The prime area of concern however is that the patient visits and gets treated by a set of care providers who have never ever seen him before and will probably never see him again. This leaves only non-physical contact methods to interact when the need arises. If and when he requires any follow-up evaluation and advice for the actual treatment received, he will have to rely on those care providers who did not provide the treatment and most possibly have only limited information regarding the same. Consequently, he is left to rely on telecommunication to help him bridge this gap, perceived or otherwise.
The patient is thus left with several options such as letters, faxes, expensive long-distance telephone calls, instant messenger chatting, video conferencing (low grade: inexpensive and informal; high grade: expensive and formal requiring prior appointments) etc. Added to this cauldron is the inevitable mayhem of information lost in transmission and faulty instructions percolated through —all due to the existence of non-integrated information exchange mechanisms causing serious inefficiencies to creep in to the healthcare delivery system. Thus, records are neither correctly interpreted nor received on time in many instances. These invariably lead to a great deal of stress, which is extremely undesirable especially in a sector where stress-free environment should be the first requirement of both the provider and receiver.
Telemedicine-enabled scenario
Let us now consider what would happen in telemedicine technology environment. Here, the patient would have a single medium through which a ‘virtual’ clinical encounter can take place where clinical data exchange—both textual and visual— can be done electronically on-demand at the speed of light. The entire medical record is available to all the stakeholders right from the beginning as the patient continues to receive his treatment irrespective of his physical location. Once he is back in his country of residence, he can continue to receive follow-ups remotely with his care providers who treated him and are consequently in the best position to monitor his progress. His primary care physician or any other care provider based locally would have physical access to the patient and can use the technology to hold consultations with the foreign care providers either as a conference in the presence of patient or by direct interaction.
The business process points that would get impacted through telemedicine would be as follows:
1. First encounter or a series of pre-procedural evaluation encounters—where the patient would interact with his foreign care providers. Telemedicine will allow a comprehensive remote-consultation face-to-face and one-on-one. If needed, medical records can be exchanged and reviewed. The primary care or the referral physician can actively participate to help clarify health issues and in devising a care plan
2. Procedural encounters—where the primary care physician can actively participate in all encounters, including surgeries as observers, and be an integral part of the care process
3. Follow-up encounters—where the patient gets in touch with his foreign care providers whenever he requires. Telemedicine allows a face-to-face interaction where the local primary care physician can actively participate to ensure better level of post-procedural and follow-up care to be delivered
There are inevitable downsides of telemedicine technology ranging from issues related to patient privacy and secrecy due to electronic transmission of Protected Health Information (PHI) to differences in time zones leading to encounters taking place at odd hours to faulty connectivity. Since nothing comes without a price, the stakeholders need to be aware of the costs involved in it and concentrate more on its benefits. Then, the entire experience will truly be a fascinating one.
Conclusion
Both telemedicine and medical tourism are here to stay. Both of them are bound to increase in acceptance and practicality to a point where it would be considered not a ‘nice to have’, i.e. want or premium requirement, but a ‘must have’, i.e. need or basic necessity.
There is a great synergy between telemedicine and BPO in healthcare in general and medical tourism in particular. For any healthcare process, there has to be a follow-up and it does not make much sense either to ask the patient to return or to forget about him once discharged. Therefore, follow-up advice and re-evaluation is imperative. Also, patient’s local care provider needs to be instructed regarding what all needs to be done further and what not. And, this is currently possible only through telemedicine.
It may justifiably be stated that without telemedicine, medical part of medical tourism is incomplete. Telemedicine allows for exchange of the patient’s medical record. Once the treatment cycle is over and the patient is fit for discharge, telemedicine becomes the medium-of-choice to follow-up remote monitoring and consultation. Since the patient is always a tourist in medical tourism, he is expected to be at a physical distance that cannot be easily bridged. His local care provider may frequently be unable to provide adequate help in many clinical situations that has a direct causal relationship with the care received in a foreign land. Telemedicine accomplishes this and therefore needs to be an integral part of medical tourism.
Author Bio
Suman Bhusan Bhattacharyya is a healthcare domain expert with over two decades of experience. He is a business solutions architect for healthcare provider applications and has worked for several IT MNCs in India. Currently, he is working as Vice-President, Clinical Services, Karishma Software Limited and is the National Secretary to the Indian Association for Medical Informatics.