Today, smartphones and tablet computers have become, in many cases, the first access points for healthcare. Coupled with the rapid adoption of telehealth during COVID-19, and predictions for how sustained this change may be - we investigate how telehealth will impact the physical design of clinic facilities, and the fundamental duality that will drive healthcare design as a digital/physical hybrid.

In a few short months during the initial periods of COVID-19, telehealth went from almost nonexistent, to boom, and has begun to decline towards a yet undetermined state of normalcy. At its height, telehealth was projected to transform what was an estimated US$3 billion in total annual revenue to a projected US$250 billion in US healthcare spending post COVID-19. Yet, the pandemic has highlighted the need for fully integrated telehealth to provide access to care and ensure business continuity now and in the future. Healthcare organisations have a tremendous opportunity to build upon the lessons learned during COVID-19 to transform care delivery moving forward. By determining which services will stay in the footprint, which services are best suited for virtual care, and which services can be agile, moving between in-person and virtual visits, healthcare organisations and independent provider practices can more effectively and efficiently respond to shifting market demands and meet evolving patient and provider preferences and needs.
As technologies advance and care delivery models morph, the boundaries between the physical and digital environments will continue to blur. It is essential to ensure that our clinic facilities can seamlessly and effectively support the integration of virtual care into their physical spaces. Agility between digital (cloudprint) and physical (footprint) assets, equity in terms of digital access and in-person and virtual interactions, and enhanced human experience will all be key components to ensure success of Internet of Medical Things (IoMT), as we continue the quest for better health outcomes. Here, we outline a few design strategies for cloudprint and footprint to address the future of healthcare services:
When considering which types of services were best suited to being conducted as a telehealth visit, 88 per cent of primary care physicians polled by HKS in 2020 considered telehealth to be a viable option for conducting primary care visits. For mental and behavioral health visits, 78 per cent of mental and behavioral physicians considered telehealth a suitable form of conducting visits, while 57 per cent of urgent care physicians and 46 per cent of women’s health physicians felt telehealth visits were suitable. Speciality services such as neurology, cardiology, oncology, orthopedic and radiology that are technology dependent were rated by physicians who conduct those services as the lowest in terms of applicability for telehealth use. Ultimately, physicians believe telehealth will increase patient volumes, requiring clinics to maintain their existing footprint while expanding their cloudprint.
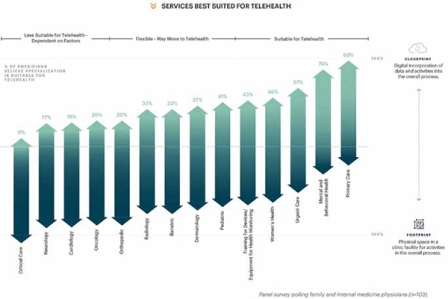
Some health interactions are better suited to telehealth, some are better suited to an in-person visit, and some are agnostic- and can be either in-person or virtual. Understanding the nuances of each interaction is important to assess whether telehealth, in-person visit, or a hybrid approach are best suited for primary care and family medicine. It is essential to program not just space, or technology, but rather the interactions that create a seamless experience across both. By establishing clear guidelines as to what types of services need to be delivered in-person, this will enable providers to determine which services can effectively move to a virtual platform in the mid-term and long-term. Within HKS’ Batist Health Hamburg Outpatient clinic design, spaces for virtual care delivery are embedded in multiple areas and at multiple scales, to support increased flexibility for accommodating present and future spatial needs – as well as the provision of a flexible layout for spaces that support telehealth to ensure they can be easily modified to support changing practice needs over time.
In HKS’ same 2020 poll, physicians also noted access and convenience as the greatest opportunities for telehealth moving forward. Telehealth possesses great potential to increase access to highquality services for patients in remote or rural areas that lack speciality services and those with physical challenges or transportation issues, but all this is dependent on digital literacy and accessibility. Educational sessions, both virtual and in-person provide the foundation in supporting patients in expanding their digital literacy, and providers should utilise telehealth platforms that are intuitive and easy for patients and providers to use to support ease of adoption. Telehealth can save both patients and providers valuable time and effort due to reduced travel time to the office, the potential for extended hours, increased opportunities for follow-up for non-exam related issues, and the opportunity to engage quickly and more frequently with patients. By leveraging virtual visits to increase service options and convenience for patients, it is also imperative to consider creative opportunities to provide necessary resources for those with limited access to technology or internet services in their home.
Within the footprint, telehealth capabilities can be seamlessly integrated in exam rooms to access virtual visits with external providers, and sufficient spaces within the clinic program will support conducting a virtual visit with multiple care team members in the same location. Beyond handheld devices and tablets, E-kiosks can also create an alternative for patients to electronically access their health information, so it is vital to ensure patient privacy and security of this health information. All these factors are crucial in establishing increased profitability, efficiency and safety as key opportunities for telehealth moving forward, as well as improved care and increased patient satisfaction.
In ensuring a reliable cloudprint for both synchronous (telemedicine) and asynchronous (store and forward) telehealth, the provision of high-speed internet capabilities must be adequately met to ensure seamless connectivity throughout the virtual visit. Whilst leveraging remote monitoring devices to support care continuity across the continuum, telehealth also calls for virtual technology support services, which play a key role in the assistance of device set-up and maintenance for both patients and providers.
Within the physical footprint, enhanced video and audio capabilities will support high-quality synchronous communication between patient and providers, addressing challenges and increase the ease of connectivity during the virtual visit. In-person technology support services, such as a tech bar within
the clinic, allow telehealth platforms to support ease of device set-up and maintenance for patients.
Despite the relatively high patient satisfaction and its perceived benefits, virtual care is still seen as a ‘proxy’ to the in-person visit. If telehealth is to reach its full potential, digital interactions during a virtual visit must be made a worthy substitute of the in-person visit, creating more experiential and more personal interactions that enhance the relationship between patients and physicians – thus, it is essential to ensure equity in terms of digital access and virtual interactions. These mean that applications to access platforms, as well as interfaces should be intuitive and easy to use, whilst ensuring simplicity of the digital format. The user interface is an opportunity to enhance the patient and provider experience, hence, applications should reduce redundancy such that information is only requested once, as well as consider single port of entry into telehealth platform that allows for text, video, email, etc.
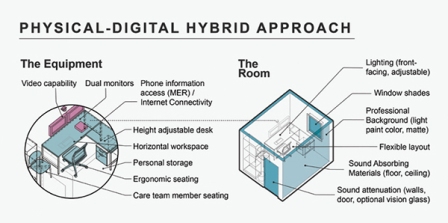
In today’s world, systems are needed where our physical interactions can be mirrored in digital space, and viceversa so the experience (and resulting outcome) is enhanced, creating beneficial redundancies for care delivery. This can also provide clinics with longterm resilience- be it in response to unforeseen events like the pandemics, or rapid advancements in technology, to ensure business continuity. The clinic footprint at HKS’ recently completed Parkland Moody Outpatient centre integrates adjustable lighting to reduce glare, sufficient illumination, enhanced video capabilities, professional and distraction-free backgrounds that have a light colour and glare reducing finishes to enhance communication, as a few interior conditions that were considered in design to optimise the virtual visit. In terms of equipment, providers should consider ergonomic furniture with adequate horizontal worksurface to support staff comfort and ensure camera placement allows for the provider to establish visual connection with the patient while dual monitor capabilities support synchronous viewing of EMR information and patient during the virtual visit.
Are we there yet? Seeking the patient and system perspective
Telehealth will very likely be an additive component to primary care, especially for family medicine and internal medicine, allowing health providers to have more business continuity, extended access, and higher convenience. At the same time, how telehealth can improve provider-patient interaction, and overall health outcomes, still warrant investigation. As healthcare organisations and independent physician practices consider how to leverage telehealth to provide the greatest benefit to patients and providers, it will be essential to think beyond current care delivery models and explore how an integrated physical/digital hybrid model will impact the future of clinic design.
Furthermore, while these strategies provide a snapshot in time to telehealth’s current limitations and future aspirations, it also serves as an impetus for further exploration and innovation to address growing questions on the topic. Can telehealth be leveraged to address the imminent healthcare worker shortages across the world? How can advances and improvements in technologies such as AI, the Internet of Things, and remote patient monitoring be leveraged to solve some of the emerging challenges with equity, engagement, and experience across the continuum of care? As more care shifts to the virtual environment in the coming future, it is imperative we begin to consider the future of home health, mobile health, retail health and healthcare’s distribution from other third places. While telehealth is the start in carving out a new frontier in virtual care deliver, it will certainly not be the end.