Over the past 50 years, the postoperative mortality from liver resection has fallen from 33 to 1.5 per cent. Whilst this is multifaceted, one key ingredient is our ability to transect liver parenchyma in a ‘bloodless’ fashion. The emerging new techniques for liver transection not only improve survival rates but also reduce mortality rates considerably.
Over the past few decades, the management of liver tumours has become a truly multidisciplinary speciality. Advances in imaging, medical oncology and interventional radiology have now allowed treatment with curative intent for many lesions that previously would have received palliation only. However, surgical resection remains the mainstay of management of liver lesions and is the most important method of achieving a cure for primary and secondary tumours. Indeed, combined with the above modalities and in the presence of favourable prognostic indicators, the surgical resection of colorectal liver metastases can offer five-year survival rates of up to 40 per cent and a mortality of less than 5 per cent.
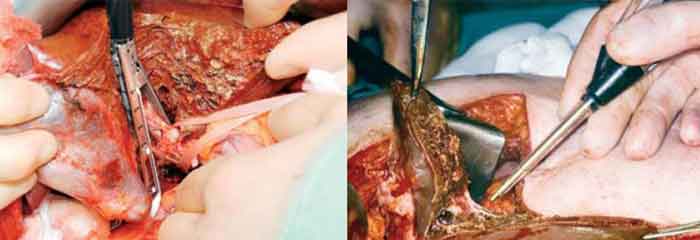
Finger Fracture
Historically, parenchymal division was firstly described via the finger fracture technique (‘digitoclasy’). Proposed by the Lin and colleagues in 1958, the friable liver tissue was fractured between the forefinger and thumb whilst identifying and isolating the key vascular and ductal structures, which could then be ligated and divided. This rather crude and imprecise technique was subsequently refined by the use of ‘crush clamp’, specially designed to crush liver tissue without damaging major vascular or ductal structures.
However, the ‘near bloodless field’ described by the use of crush clamps was often achieved at the expense of compromised oncological margins, and soon led to the development of more precise and targeted dissecting instruments.
Ultrasonic dissection
An ultrasonic dissector such as the CUSA (Cavitron Ultrasonic Surgical Aspirator, Tyco Healthcare, Mansfield, MA, USA) emits ultrasonic waves of a frequency high enough to divide the liver parenchyma whilst sparing structures greater than 2 mm in diameter, which can then be sutured or clipped. Using the same principle, the ultrasonic shears (Harmonic Scalpel, Ethicon, Cincinnati, OH, USA), often used in laparoscopic resections, uses ultrasound to divide and seal vessels up to 3 mm in diameter between its jaws.
High pressure water dissection
Water jet dissectors use a pressurised jet of water to achieve transection. Both CUSA and water jet dissectors have the advantage of removing a 5 mm diameter line of tissue, important in achieving a margin where dissection is close to the tumour.
Radiofrequency Dissection
The TissueLink dissecting sealer (TissueLink Medical Inc., Dover, NH, USA) uses radiofrequency energy coupled with a saline to achieve both dissection and coagulation of liver tissue. More recently, radiofrequency ablation, in which coagulative necrosis is induced in a sphere of tissue around the tip of a probe, has been used sequentially along the transection line to achieve ‘in line’ coagulation. A knife is then used to transect the pre-coagulated parenchyma.
Diathermy
Diathermy uses high frequency alternating current to generate high local temperatures which induces local coagulative necrosis. Some of the most popular instruments currently available are the Argon beam coagulator (Valleylab, Tyco Healthcare, Boulder, CO, USA), which allows coagulation of small vessels, and more recently, a bipolar vessel sealing device (Ligasure, Valleylab, Tyco Healthcare, Boulder, CO, USA), which seals arteries up to 6 mm and veins up to 12 mm in diameter.
Although some of these instruments (such as the harmonic scalpel and ligasure) claim to be able to both dissect parenchyma and seal vessels, reports of bile leaks are common following their use. It is, therefore, usually necessary following transection to formally seal vessels in order to ensure meticulous haemostasis and prevent bile leaks. Historically, this has been achieved by a combination of monofilament sutures, clips, diathermy and topical agents (such as coagulative glue and haemostatic collagen). More recently, stapling devices have also been successfully used to transect liver parenchyma in addition to large vessels.
Principles of transection
Dissection through the liver parenchyma poses unique challenges. Firstly, the liver’s inherent vascularity poses a high risk of uncontrollable haemorrhage if blood vessels are not identified and sealed in a timely and effective manner. It is now well established that morbidity and mortality from liver resection is closely correlated with intraoperative blood loss. Furthermore, the need for blood transfusions during liver surgery is strongly associated with poorer long-term outcomes. Therefore, surgical and anaesthetic techniques have focussed on reducing intraoperative blood loss when transecting the liver. Secondly, the complexity of the liver’s biliary structures necessitates careful dissection and occlusion to avoid postoperative bile leaks, another important source of morbidity and mortality in the post-liver resection patient.
The ideal surgical instrument for liver transection must therefore be able to effectively cut through the parenchyma whilst simultaneously sealing any portal vessels or bile ducts. In reality, because no such single instrument yet exists, transection is achieved by a combination of instruments and techniques which firstly facilitate division of the liver tissue with subsequent identification and sealing of the vessels. In this way, a ‘Two-surgeon technique’ has evolved, whereby the first surgeon directs parenchymal dissection and the second surgeon is responsible for coagulation and vessel sealing. Also, it reduces the transection time—especially important in limiting liver ischaemia during use of the Pringle manouevre. It also acts as a valuable training tool.
The significance of minimising intraoperative bleeding has led to methods aimed at achieving bloodless liver surgery, involving surgical techniques to occlude hepatic inflow and outflow vessels, and anaesthetic techniques to minimise central venous pressure.
Inflow vessel occlusion
Pringle firstly described portal triad compression in 1908 in an attempt to control bleeding from the liver in trauma patients. The ‘Pringle manoeuvre’ is achieved by application of a soft (non-crushing) bowel clamp to the structures in the hepatoduodenal ligament at the porta hepatis. Whilst this is beneficial in limiting parenchymal bleeding from inflow vessels, it unfortunately has no effect on back bleeding from the hepatic veins and Inferior Vena Cava (IVC), which may still be alarmingly profuse. In addition, it renders the parenchyma ischaemic for the duration the clamp is applied, and intermittent clamping (e.g. 20 minutes on, 5 minutes off) is preferred by many surgeons, including our unit, to reduce the risk of post-hepatic liver insufficiency potentially caused by hepatocyte ischaemia. Where possible, inflow vessels to the segment to be resected should be ligated and divided prior to transection (the extra-hepatic approach). In addition to devascularising the segment to be resected, this has the advantage of demarcating the transection plane.
Outflow vessel occlusion
Heaney and colleagues were the first to describe total vascular exclusion during a liver resection by control of the suprahepatic portion of the IVC. This method allowed a true bloodless surgical field that could be safely maintained for a period of up to 60 minutes while the liver was transected. However, it was a complicated and time-consuming procedure, and was poorly tolerated in patients with low cardiorespiratory reserve, as evidenced by their mortality rates of up to 50 per cent. This technique has further been refined by the use of vascular stapling devices to seal individual hepatic veins after they are dissected out. Combined with inflow vessel occlusion, this provides a rapid and effective method of achieving a near bloodless field during transection.
Low CVP anaesthesia
The higher the Central Venous Pressure (CVP), the greater the venous engorgement of the liver and the greater is its tendency to bleed on transection. This has led to an important role for the anaesthetist in reducing blood loss during liver surgery. The intraoperative use of fluid restriction and venodilators allows a CVP of 0–5 mmHg in the face of a normal blood pressure, and minimises blood loss by limiting retrograde bleeding from the hepatic veins during transection. A number of studies have now shown that low CVP anaesthesia is well tolerated and that the theoretical risk of air embolism is very rarely clinically evident.
Anatomical considerations
A better knowledge and understanding of the segmental anatomy of the liver, described in detail by Couinaud, has revolutionised liver resection strategies. The ability to perform segmental liver resections has allowed the radical excision of lesions whilst maximising the size of the remaining healthy liver, vital in avoiding postoperative liver insufficiency. In addition, the hepatic lesion must be well imaged prior to surgery to determine not only whether it is resectable, but also the nature of the intended resection with respect to the location of hepatic veins and major portal vein structures. Careful examination of preoperative imaging, further refined by intraoperative ultrasound allows anticipation of these structures during transection, thereby avoiding their accidental division. It also enables an adequate resection margin to be established around the tumour, allowing curative excision.
Transection at our institution
Basingstoke is a large volume centre with a throughput of 178 cases in 2007 and a total of 1657 patients resected so far. All patients are imaged preoperatively using liver-specific MRI, which uses two contrast agents (Gadolinium and Resovist). The liver is approached via a right subcostal incision and an assessment is made of resectability and the confirmation of the absence of peritoneal disease or nodes at the porta hepatis, which would render the case irresectable. The liver is mobilised and resectability is further confirmed by bimanual palpation and intraoperative ultrasound. The resection margins are delineated with diathermy. An extra-hepatic approach is preferred for inflow vessel occlusion where the tumour is close to the porta hepatis. In cases where the tumour is greater than 2 cm from the porta, extra-Glissonian stapling of the portal triad is preferred. The hepatic veins are stapled where possible to enable total vascular occlusion. Parenchymal dissection is performed using an ultrasonic aspirator (Cavitron Ultrasonic Aspirator, CUSA, Tyco Healthcare, Mansfield, MA, USA) with intermittent portal triad clamping (20 minutes on, 5 minutes off. In steatotic and cirrhotic livers the times are 10 and 7 minutes, respectively). During transection, vessels less than 1 mm in diameter are sealed via the Argon beam coagulator (Valleylab, Tyco Healthcare, Boulder, CO, USA). Larger branches are clipped or ligated with monofilament suture. The two-surgeon technique is used, with the lead surgeon on the patient’s right operating the CUSA, and applying clips and sutures, and the second surgeon on the patient’s left operating the Argon beam coagulator. Both apply traction to the liver in opposing directions to accentuate the transection line. Following removal of the specimen, the freshly transected liver surface is sealed using coagulant glue (Quixil, OMRIX biopharmaceuticals, Belgium) and haemostatic collagen sheets (Fibrillar, Johnson & Johnson Medical, Ascot, UK). Using these techniques, a median clamp time of 32 minutes and blood loss of 330 ml was achieved for 2007, with a mortality of 0.3 per cent.
Conclusion
There is currently no single instrument available that effectively addresses both tasks of parenchymal dissection and vessel sealing, and transection of the liver is generally achieved using combinations of the above instruments and techniques. There is little evidence from randomised controlled trials demonstrating superiority of one instrument over another, and the available literature suggests that all current strategies for transection can be used with equal effectiveness. Choice of transection instrument and technique is, therefore, based on individual surgeon preference, and the most significant factor in achieving an effective and safe liver resection remains the experience of the surgeon.
AUTHOR BIO
Alun Jones is a Specialty Registrar in General Surgery currently working in Basingstoke and North Hampshire Hospital. He graduated from the University of Cambridge Medical School in 2003 and subsequently completed a Basic Surgical Training Rotation at Norfolk and Norwich University Hospital.
Merv Rees is a Hepatobiliary Surgeon based at Basingstoke Hospital, North Hampshire, UK. He is currently President of the Association of Upper Gastrointestinal Surgeons of Great Britain and Ireland.