NEONATAL CARE
A global crisis in desperate need of innovation
Despite considerable progress in other areas of healthcare, poor neonatal care causes devastating outcomes globally. Infant incubators play a leading role in reducing mortality and morbidity, but lack innovation making any meaningful progress costly and hard to achieve.

Significant progress has been made in reducing global mortality in children under the age of five, and the world would be on track were it not for the lagging progress in reducing newborn mortality.
In 2016, the United Nations (UN) issued an urgent call for all participating nations in Sustainable Development Goals (SDGs) to reduce neonatal mortality rates. Since, progress in lowering mortality for newborns has been slower than that for older children under five—in fact, newborn mortality has increased according to the World Health Organization (WHO). In 2020, nearly half (47 per cent) of all under-5 deaths occurred in the newborn period (the first 28 days of life), an increase from 1990 (40 per cent). Every day, over 6,500 babies die in the first month of life. In 2020, an estimated 2.4 million newborns died worldwide. Considering other factors such as underreporting, the numbers are arguably much higher.
The first month of life is the most vulnerable period for child survival. Preterm birth, intrapartum-related complications (birth asphyxia or inability to breathe at birth), hypothermia (low body temperature), infections and birth defects are the leading causes of most neonatal deaths. Most newborns who die within the first 28 days of birth suffer from conditions and diseases associated with lack of quality care at or immediately after birth and in the first days of life.
In this article, light will be shed on some of the reasons and factors for this relative lack of global progress with newborn healthcare and the high numbers of neonatal mortality. There is no silver bullet to reduce newborn mortality and more specifically neonatal morbidity, but there are glaring gaps in care and lack of adequate solutions.
Socioeconomics, maternal and newborn health are all closely linked, but newborns who are sick or born prematurely have unique clinical needs of their own. We have to understand and address the leading causes of global newborn mortality such as hypoxia, hypothermia, severe infections, and complications related to prematurity.
Simple interventions — from education and perinatal care before and after birth, to providing a clean environment, oxygen, heat, antiseptics and antibiotics to the newborn could save millions of lives, but they often fail to reach sick babies in a timely manner.
These issues hindering progress are not only in developing countries, but also in the developed world too. Variations in infant and neonatal mortality continue to persist in the United States and in other countries based on both socio-demographic characteristics, such as race and ethnicity, and geographic location. One potential driver of these differences is variations in access to risk-appropriate delivery care. According to the March of Dimes 2022 report, the U.S. preterm birth rate increased to 10.5 per cent in 2021 – a significant 4 per cent increase in just one year and the highest recorded rate since 2007. The highest majority were in Black and native American women.
The sad fact is many healthcare systems are understaffed and under-budget to deliver the appropriate care needed and where it is needed. It is no secret that staffing shortages are rampant or that providers are ill-equipped to provide the special care these babies need after delivery. A simple example is the use of Chlorhexidine solution to disinfect the umbilical cord, or provide heat, breathing support or phototherapy, which will save countless lives. More so than any other patient, sick babies rapidly deteriorate and need close, meticulous care even in low-resource and low-tech settings. This brings us to the most important device in saving newborns. The cornerstone of technical solutions to save a small life remains the infant incubator.
Neonatal incubators are a basic, but unique and highly specialised medical equipment designed as the patient’s own medical contained space to provide a clean and controlled environment for premature or ill newborns. Their use can help to reduce the risk of morbidity in premature or ill infants by providing a controlled environment that promotes growth and development with a direct health outcome for years to come. This can include maintaining a consistent temperature, humidity and oxygen levels, as well as protecting the infant from infection. In addition, they can also provide medical support, such as administering oxygen, tube feeding or phototherapy. There are several key factors that must be considered in order to properly maintain an infant incubator. Some of these include cleanliness to prevent nosocomial infections, maintenance and repairs, infant monitoring and staff training. Overall, the use of infant incubators can help improve the health and survival rate of premature or ill infants and prevent stunted growth, as well as future physical and mental development.
Unfortunately, globally we spent less than US$8.6 per newborn the whole year to purchase new incubators
One of the driving factors is to rethink and overhaul the system, which include the lack of will and appetite to invest in affordable and practical innovation in the basic healthcare of neonates. This is a challenge we face despite the staggering number of babies dying annually or survive to live with disabilities for the rest of their lives, especially in developing countries, which costs four to seven times more for a preterm infant with common morbidities than babies born healthy. The economic fallout runs in the billions globally for infant morbidity and mortality, and is the single greatest socioeconomic burden on any society.
Locally appropriate and accessible “neonatal care units” need to be urgently developed and staffed with motivated and skilled neonatal nurses, and adequately equipped with lifesaving devices supported by simple yet innovative technologies that are affordable and practical to maintain and operate. We are not talking about preventable illness and diseases; we are talking about simple innovation of a gold-standard machine that has been using the same principal technology for over a century.
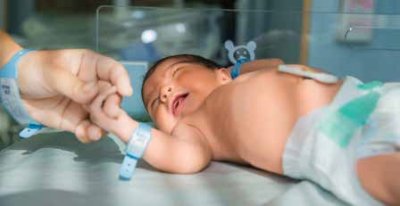
Incubators must evolve
There can be several reasons for a shortage of infant incubators:
- Lack of innovation: As we are building on top of a century-old technology, new technical developments only increase the price and complexity of the machine.
- High cost to purchase: Infant incubators quite expensive, making them particularly difficult to afford in low and middle-income countries (LMIC).
- High cost to maintain and clean: The nature of providing heat and humidity makes infant incubators notorious for harboring thriving pathogens, despite routine cleaning and disinfecting. This makes incubators a source of nosocomial (hospital-acquired) diseases.
- Limited resources: Many healthcare facilities, particularly in LMIC, may not have the resources or funding to maintain or replace existing incubators. It is a known practice to use old refurbished and donated incubators with a lifespan of few months and unable to be repaired thereafter.
- Limited access to electricity: With the lack of innovation, incubators are totally dependent on grid electricity. In many countries, especially in rural areas, electricity is unreliable or not widely available, which leads to tragic outcomes.
- Limited access to spare parts: In some countries, spare parts for incubators may not be available to maintain or repair existing incubators and more so for the old and refurbished donated units.
- Limited access to trained personnel: In some areas, there may be a shortage of trained personnel on site, such as technicians, neonatologists and neonatal intensive care unit (NICU) nurses, who are able to operate and maintain infant incubators.
- Limited manufacturing: The lack of financial incentives for production of infant incubators has led to scarcity in comparison to the number of sick babies.
- Political will and economic instability: In many areas globally, political and economic instability can make it difficult for hospitals and healthcare facilities to secure funding for new equipment or to maintain existing equipment.
Overall, a shortage of infant incubators can be caused by a combination of many factors, but without seriously rethinking of the technology, a core problem which hinders any progress is hospital-acquired (nosocomial) infections for premature and ill newborns in the NICU. The main source of such a problem is the cleanliness of infant incubators. Nosocomial infections cause substantial harm to hospitalised neonates. They have considerable health and economic consequences, including increased morbidity and mortality, prolonged length of stay (LOS) and increased medical costs. In North America, it is estimated that each episode of sepsis prolongs the duration of a neonate's hospital stay by two weeks, resulting in an incremental cost of US$25,000 per episode. This can compound to millions of dollars for infants who stay months in the NICU.
Among medical devices, neonatal incubators have been well recognised as a source of pathogens involved in the spread of nosocomial infections. One study conducted in a French NICU over a 3-year period (2016 to 2018) investigated premature infants with bacteremia. Initially, several outbreak containment strategies were carried out without success. Next, outbreak investigation pinpointed the neonatal incubators as the primary reservoir and source of contamination in this outbreak, which led to their replacement, thus resulting in the containment of the outbreak.
Another study from Nepal indicated that almost 75 per cent of the NICU samples came back positive. The majority of infections were isolated from incubators and radiant warmers. Clearly, disinfection protocol, routine surveillance and supervision of the various aspects of the disinfection processes might not provide a safe environment avoiding harmful conditions for the newborns.
Unfortunately, the reality is continued mortality and morbidity, lengthier hospital stays, the lack of meaningful innovation, cost, complexity and valuable time spent by staff cleaning and disinfecting incubators instead of monitoring and caring for a sick baby. Nevertheless, such protocols will take many incubators, which are scarce in number to start with, out of commission.
Overall, maintaining the current NICU system in a hospital setting is costly and might not be sufficient without a new and innovative way of thinking. Smaller hospitals may not be able to afford to have a NICU fully equipped due to the high costs associated with specialised equipment, staffing and resources required to provide high-quality care for premature and critically ill infants. This is a global problem and no one country is spared, but devastating in low-resource areas. According to the United States Government Accountability Office in 2022, research indicates that the number of rural hospitals providing obstetric services declined from 2004 through 2018 to half, according to the most recent data available. Studies showed that closures were focused in rural counties that had a majority of Black or Native American residents, and were considered low income. Vast swaths of the U.S. are in crisis, and the rates of prematurity is increasing and NICU’s are closing.
And yet, neonatal mortality and morbidity remain a silent global crisis with deep psychological, economic, social and ethical consequences.
The current neonatal care system is designed around century-old, expensive, complicated and hard to maintain technologies which were developed for high-income countries and yet are used in low-resource areas and LMIC countries. Such a system that lacks the fundamental understanding of the needs and circumstances on the ground for stakeholders, users and patients - is flawed. The current system is designed from the top down, rather from the base up.
There is a great deal of information and countless scientific studies addressing the core cause of infant mortality and the shortage of care for ill newborns, some of which are the complex and expensive systems to run a NICU, the initial cost of infant incubators and their high cost to maintain and a lack of evolution that addresses those challenges.
It's important to note that the status quo with its complexity and high-cost designs for developing countries and its use in low resource settings should not be “a matter of fact” consideration especially when it comes to neonatal care. We should design what works, without compromising quality of care.
We should rethink the quality of care and the health and well-being of the newborns with a new vision and foresight, promoting innovative thinking and technologies to leap forward.
References:
1 https://www.who.int/news-room/fact-sheets/detail/levelsand-trends-in-child-mortality-report-2021
2 https://www.marchofdimes.org/about/news/march-dimes-2022-report-card-shows-us-preterm-birth-rate-hits-15-year-high-rates#:~:text=March%252520of%252520Dimes%25252C%252520the%252520nation's,highest%252520recorded%252520rate%252520since%2525202007.
3 https://www.usp-pqm.org/sites/default/files/pqms/article/chlorhexidine-for-umbilical-cord-care-cwg-2014-07.pdf
4 https://pubmed.ncbi.nlm.nih.gov/17606536/
5 https://publications.aap.org/pediatrics/article/129/4/e1104/32369/Epidemiology-and-Diagnosis-of-Health-Care
6 https://journals.asm.org/doi/10.1128/spectrum.00964-22
7 https://aricjournal.biomedcentral.com/articles/10.1186/s13756-021-00901-2
8 https://www.gao.gov/assets/gao-23-105515.pdf





