Cambodia is on a mission to make a change in its healthcare system and reach for the great opportunity that sits waiting on its horizon. C Cambodia ranks very low in availability of surgical care, at 146 out of 192 countries today, with only 419 procedures performed per 100,000 people. By comparison, the U.S. averages more than 21,000 procedures per 100,000 people, while South Africa averages 5,4001. Cambodia is working toimprove the health status of its citizens simply by increasing surgical capacity and quality.
For all low- and middle-income countries, including Cambodia, improving surgical capacity is in everyone’s best interests. Limited access puts up to five billion people at risk globally, resulting in about 17 million deaths annually. These avoidable deaths include people with noncommunicable diseases (cancer, diabetes, heart disease), and trauma victims, as well as pregnant women and newborns.

Transformational outcomes
According to local health experts, Cambodia could potentially reduce noncommunicable diseases by 30-50% if more surgical facilities were available. Significantly reducing the number of people with disabilities (from injuries in car accidents, etc.) and addressing congenital anomalies, such as cleft lip, are other projected outcomes.
Achieving such aspirational goals, however, requires transformational change. And, Cambodia, catalyzed by the GE Foundation-funded Safe Surgery 2020 (SS2020) program, is making great progress towards these aims.
Established as part of the GE Foundation’s $25 million commitment to accelerate access to safe surgery and anesthesia worldwide, SS2020 was introduced in Cambodia in early 2019 with eight training modules. Topics covered included Key Performance Indicators; Leadership; Clinical Training; Safe Anesthesia; Equipment Sterilization; Health Technology Maintenance (through training biomedical technicians); Mentorship (through Project ECHO), and Remote Clinical Training (using Touch Surgery to teach surgical skills). Through these trainings, close to 900 Cambodian surgical experts, clinicians, and nurses had gained new surgical, anesthesia, and caesarian procedure skills when the program concluded this year.
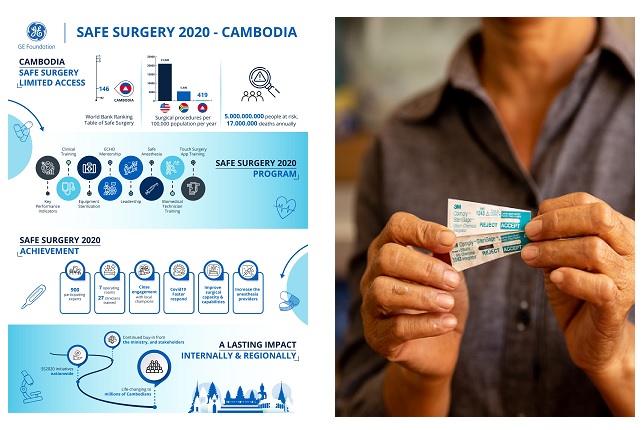
An audit to identify urgently needed equipment and training was also held. From this assessment, seven operating room packages were installed at seven hospitals with training sessions run for an additional 27 clinicians.
Success factors and insights gained
Achieving this level of success was not a given or sure thing. Language barriers, liaising with diverse program partners, creating Cambodia-relevant programs, and managing a host of priorities, challenged the program partners.
These hurdles were well-managed, however, by the Safe Surgery 2020 program implementation partners Assist International, Jhpiego, Harvard Program for Global Surgery and Social Change, and Dalberg Advisors. Working closely with Cambodia’s Ministry of Health and the Calmette Hospital in Phnom Penh, they adopted strategies that are relevant and applicableto any organization (corporate, non-profit, government, etc.) entering a new market and deploying new innovations. Close engagement with local champions was pivotal. Regular meetings and calls with key stakeholders, program managers, and partners throughout Cambodia were vital to build awareness and trust.
Finding a like-minded partner was equally vital. In our case, the Calmette Hospital was a terrifically, and advocate in encouraging the Ministry of Health to back SS2020. Calmette was also instrumental in encouraging two other national, and five provincial, hospitals to join the program.
Agility was the other important factor. As SS2020 Cambodia coincided with the start of the coronavirus outbreak, we pivoted quickly to run virtual training programs. At various times, we also swapped out content to deliver COVID-19 information covering critical care and oxygen therapy.
Right program at the right time
The surgical capacity programs also produced an unexpected, but timely and important benefit. They helped strengthen Cambodia’s health system when it was stressed during the coronavirus pandemic.
Newly donated equipment helped the eight partner hospitals to respond faster and more effectively to COVID-19. For instance, patient monitors, pulse oximeters and ventilators that were donated to Calmette Hospital played a key role in diagnosing and treating hypoxemia. Donated anesthesia machines along with ventilators were also repurposed for patients who did not have COVID-19, thus freeing-up ventilators for COVID-19 patients. SS2020 also helped setup tele-mentoring systems to share COVID updates provided by physicians around the world.
A lasting impact – internally and regionally
While SS2020 Cambodia wrapped up in May this year, we believe the 24-month program has laid the groundwork for more healthcare innovation and collaboration. It has also introduced foundational training programs that can be updated for future generations.
A Safe Surgery Checklist shared with stakeholders will also provide more consistency and adherence to common standards in sterilization and anesthesia best practices. And, as we have seen in other SS2020 markets like Tanzania and Ethiopia, we expect the Project ECHO mentorship program, a framework to share information with physicians and other health professionals, to grow more and more impactful as it continues.
Most importantly, Cambodia now has champions and leaders who can keep advocating and pushing for more access to safe surgery. They can lead the charge to scale up SS2020 initiatives nationwide.
With continued buy-in from the ministry, and other stakeholders, there will be profound change for millions of Cambodians. In time, Cambodia’s champions and leaders could also share their expertise with regional colleagues facing similar capacity issues. We continue to look forward and are excited to learn more as we go and to celebrating new successes and milestones in the years ahead.
Reference:
1. World Bank Database, Asia Pacific Observatory on Health Systems and Policies, ‘The Kingdom of Cambodia Health Systems Review’, 2015 (Safe Surgery 2020 Impact Report)