Strengthening Health Systems through Artificial Intelligence (AI)

Artificial Intelligence (AI) will restructure health systems for the future. Many healthcare institutions are testing AI innovations to optimise operations and improve population outcomes. This article highlights its current application in health systems, challenges, and potential strategies that industry and health leaders can adopt to facilitate AI adoption in healthcare.
Artificial Intelligence (AI) is pushing the frontiers of digital innovation in the current decade. The release of ChatGPT beckons a tipping point of a tech revolution, with its humanlike ability to write codes, poems, and academic reports. AI’s potential to disrupt traditional industries, once a pipedream, will be realised in healthcare soon.
Private and government investments in AI are increasingly common in healthcare. Between 2022 to 2029, the global AI in healthcare market is projected to grow from US$13.82 billion to a staggering US$164.10 billion1. With boundless healthcare applications such as virtual nursing assistants, research of novel therapies, and medical diagnostics, AI promises to rebuild health systems for the future.
Current applications of AI in health systems
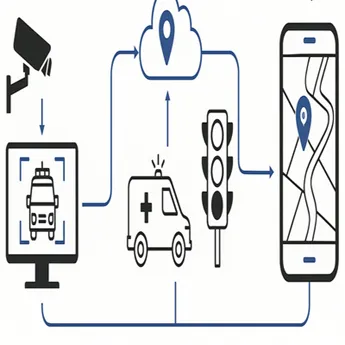
#1: Real-time surveillance and predictive analysis of infectious diseases
The use of predictive analytics for disease risk has been one of the most pervasive AI applications in recent years. Using a combination of machine learning and AI algorithms, predictive analytics analyses large volumes of data to identify patterns and future trends. These key insights generated then inform health decision-making.
For public health surveillance, governments have deployed AI-powered analytics to evaluate infectious diseases’ risk. In 2019, the Thai Ministry of Public Health partnered Microsoft to deploy a cloud-based AI system that predicts public health risks and gastrointestinal disease hotspots. With the assistance of community volunteers capturing photographs of public restrooms, the AI model evaluates these photos at an accuracy rate of 80 – 90% and notifies health administrators of sanitation issues2.
With substantial accuracy, AI-powered analytics can aid health administrators in evaluating the risk of infectious disease outbreaks and directing public health action.
#2: Patient triaging of high-risk patients and preventive care measures
Predictive analytics have aided doctors to triage patients by calculating their risk profiles and prioritise early intervention for them. Apollo Hospitals, one of India’s largest private hospital chains, partnered with Microsoft to develop an Indian-specific heart risk score by applying machine learning and AI to cardiovascular health records. The AI model helps predict a patient’s risk of heart disease and allows doctors to customise a care plan for them3.
Similarly, North Carolina-based health system Novant Health leverages on Jvion’s predictive analytics to reduce readmissions for congestive heart failure patients. Through this, high-risk patients are identified with changeable trajectories and provided patient-specific recommendations4. These recommendations have reduced congestive heart failure by 13%, preventing 130 readmissions per 1,000 discharges for a potential saving of approximately US$1 million5. AI-powered triaging is a powerful tool capable of increasing healthcare savings, optimises health workforce efficiency, and improving population health.
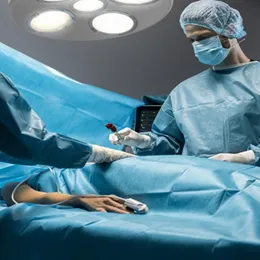
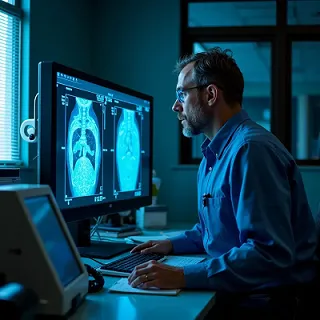
#3: AI-powered Medical Imaging
The future of medical imaging will integrate AI-analytics into existing diagnostics, aiding healthcare professionals to deliver more efficient and accurate patient diagnoses. In the early stages of the COVID-19 pandemic, chest CT scans of patients assisted physicians to diagnose infections early, and complemented lab testing6,7.
Beyond COVID-19 imaging, Singapore applied SELENA+, an AI-powered image reader, to support its national retinopathy screening program. The deep learning AI system analyses retina images to identify signs of diabetic eye diseases. Used together with the expertise of healthcare workers, the approach saved patients up to 20% of screening costs and delivered screening reports in less than half an hour8. AI-assisted medical imaging promises to minimise human errors and save patient costs.
The state of AI uptake across health systems
Key global shifts both recent and longstanding are fuelling AI’s adoption in healthcare: the overwhelming volume of health data; the COVID-19 exacerbating existing healthcare gaps; and massive technology advances9.
Unfortunately, geographic disparities in adopting AI innovation to health systems remain. Healthcare leaders in Asia reported the highest uptake of predictive analysis in their clinical settings compared to other geographies10. Even among Asian countries, Singapore’s estimated uptake of predictive analytics (92%) far outweighs Indonesia (62%), and India (59%)11. In several countries, the adoption of many AI-driven services is spearheaded by private entities, limiting access to patients who can afford private healthcare.
Barriers to adopting AI in health systems
Many roadblocks in health systems must be addressed in the quest to herald in the age of AI. Data security and privacy are critical issues for leaders with healthcare data breaches on the rise. In the past three years, over 90% of global healthcare organisations reported at least one data breach12. Also, many countries still lack a regulatory sandbox to test and drive AI innovation in their public health systems.
Digital upskilling of clinicians is a large gap for AI adoption where it has been cited as the biggest barrier to digital health adoption even in Singapore – a global leader in AI healthcare adoption13. Nevertheless, there are several proposed strategies -such as a co-governance model -that can help to overcome these barriers and minimise concerns from policymakers, healthcare professionals and patients14.
What are some policies or systems that hospitals and healthcare systems can put in place to facilitate adoption of such disruptive technologies?
Firstly, policy makers must have a holistic view of the various perspectives stakeholders have on AI. A clear mapping of different viewpoints is the first step towards creating a common agenda among various agendas, enabling the development of effective governance around AI15. Allowing policymakers and managers to involve key stakeholders will help incorporate their insights into AI policies16. Thus, an adaptive approach allows for policies to be tweaked accordingly as new technology progresses and uncertainties emerges.
The adoption of AI-applications is also contingent on having the necessary data infrastructure. Policymakers must prioritise the development of data collection, integration, and management platforms before focusing on real-world applications17. It is necessary to first shift written medical records to electronic health records (EHRs) for AI to run its predictive analysis and modelling. The shift to EHRs requires health professionals to be upskilled digitally.
To prevent data leaks and for secured data protection, differential privacy and AI software that minimises privacy breaches can be developed. Differential privacy is a form of data security using a machine learning algorithm to anonymise the data, such that even when patterns and insights generated are publicly shared, it withholds personal data18. This helps to protect patient confidentiality and personal health data by designing AI with privacy-enhancing technology. In Romania, a cloud-based AI application with advanced data protection features has been developed where specific functions in a cloud infrastructure such as ID copying protect one’s data verification19.
Despite the promise of AI models in medical imaging, it may be difficult for physicians to interpret AI-assisted clinical diagnoses to patients. To address this challenge, healthcare systems can consider explainable AI (XAI) which focuses on understanding how the AI model functions20. XAI techniques are less accurate with a focus on predictive performance but simplifies clinical interpretation in a healthcare setting. Doctors can utilise XAI technology to interpret the results according to patients’ medical condition. This allows for health systems to shift towards a patient-centric approach with clinicians drawing support from AI.
Future trends
The large amount of data processed by AI makes it compatible with blockchain technology. Blockchain in healthcare allows for the secure transfer of patient medical records, making it suitable for storing large amounts of data generated by healthcare. The synergy of AI and blockchain is an exciting prospect with AI’s ability to process large volumes of data. Together with secured data access, patients’ privacy, and interoperability provided by blockchain, the combination of blockchain and AI provides a chance to reshape current healthcare ecosystems towards a patient-centric approach21.
An example of current AI and blockchain usage would be its implementation in combating the COVID-19 pandemic where decentralisation offered by blockchain allows for various providers to gain access to health records for decision-making across different care settings22. With COVID-19 surveillance data stored on the blockchain, this allows the construction of a primary dataset in a secure, decentralised storage for COVID-19 research while keeping patient confidentiality.
While AI disruption in healthcare is progressing, its potential continues to be tapped on to strengthen national health systems, support clinical decision-making, and explainability of medical decisions for patient understanding.