Cultural, social and linguistic barriers are a great challenge for healthcare providers. In order to overcome these barriers, clinicians must rethink their daily clinical work. The data compared in this article show that immigrants in Europe differ from natives but also from their countrymen at home. The investigation of this population should help us to provide better healthcare.
Increasing migration worldwide leads to formation of multi-ethnic societies. In 2006, there were about 200 million immigrants worldwide. Ethnic and cultural diversity presents a great challenge for all healthcare providers. Problems arising through this diversity are wide-ranging and require rethinking of already existing healthcare approaches and structures.
Talking about racial and ethnic differences highlights an important question: terminology of ethnic categories is often inconsistent and problematic. Use of such basic terms like ‘race’, ‘ethnicity’ and ‘minority’ is almost always undifferentiated. The diversity of minority groups less homogenous is not usually perceived by an observer who does not belong to this group. Usual terminology also does not take into account the degree of acculturation to the country of immigration.
Racial disparities in health have been well-described in current literature. Data shows that members of minority groups suffer disproportionately more cardiovascular disease, diabetes, asthma, and cancer. Musculoskeletal pain is more prevalent among immigrants in Europe than among native Europeans. Mood disorders among immigrants to Europe have also been reported to be more prevalent than among native Europeans, but not all studies confirmed these findings.
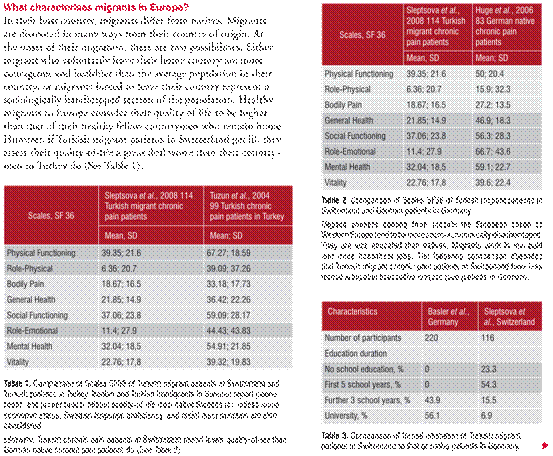
Racial differences among migrants result in migrants receiving unequal treatment. Most studies find that various ethnic groups are not given equal healthcare. This inequality of healthcare for various ethnic groups was observed for instance in pain treatment for all types of pain (i.e. acute, cancer, chronic non-malignant) and in all settings (i.e. postoperative, emergency room).
Communication between doctor and patient is often negatively affected by these cultural differences. In medical consultation, both migrant patients and their providers interact differently than natives and their clinicians do. To reduce racial and cultural disparity in care, the authors recommend that healthcare providers and organisations employ a culturally sensitive approach.
The quality of the relationship between the clinician and the patient is crucial for diagnosis, treatment and healing. Patient-centred encounters increase patient satisfaction and improve medical outcomes. Similarly, cultural competency in treatment of migrant patients is recognised as an essential factor for the quality of healthcare. Thus, patient-centred communication should contain the specification of cultural competency.
Many authors present ‘cultural competency’ as an integrative model of the healthcare system at both institutional and professional levels. The institutional level of such a culturally competent healthcare system requires primarily that both interpreter services and culturally and linguistically appropriate health education materials are available. Training programmes for healthcare providers to develop their cultural competency are necessary at the professional level of such a healthcare system. Such training programmes improve knowledge, attitudes, and skills of health professionals, which influence patient satisfaction positively.
The perspective of the patient to culturally sensitive healthcare has also been investigated. Along with universal themes like individualised treatment, effective communication and professional competency, results revealed that patients wish a culturally specific patient education and culturally sensitive staff.
An increasing quantity of current literature has begun to reflect on terminology. Fundamental terms such as ‘culture’, ‘culturally sensitive’ and ‘culturally competent’ in medical context begin to be used by clinicians who are confronted everyday by migrant patients. The need to articulate clear definitions of these terms and find consensus has been slowly recognised. One thing is clear: Culture is a dynamic concept. Moreover, culture varies within an ethnic group and is in change. Most authors emphasise that clinicians must become aware of and also respect differences in cultures. Clinicians should recognise unique cultural and religious beliefs, ethnic values, and traditional practices—all of which can be in transformation—within any ethnic group. Cultural sensitiveness and competency requires that the clinician reflect on his or her own cultural system. Self-reflection is necessary to develop awareness of one’s own attitude toward persons of different ethnic or cultural groups.
Although current studies show that language is not the only influence on the quality of clinical communication, nevertheless language proficiency does play a very important role in medical encounter. Several studies establish that professional interpreters have a positive impact on clinical care. Lack of linguistic comprehension decreases patient satisfaction. Whereas concordance of language between the clinician and his or her patient does reduce emergency visits and their costs, in general, such enhanced interpreter service intervention does not significantly change hospital costs.
Growing use of the interpreter presents new problems to researchers and clinicians. The role of the interpreter in the clinician-patient consultation has not been clearly ascertained. The so-called transmission model of communication introduced by Shannon and Weaver requires precise and complete translation. In clinical reality, however, this theoretical model does not suffice.
The role of the interpreter in healthcare settings has been discussed, but consensus is yet to be achieved. One of these roles is that of the so-called ‘cultural broker’. Can culture really be translated?
In any case, the quality of clinical consultation depends on mutual agreement by all participants about the interpreter’s role. However, innovative strategies of medical translation, for instance Remote Simultaneous Medical Interpreting (RSMI) have been introduced and tested in the clinical practice. This strategy of translation removes the person interpreting from the presence of the patient. Patients believe their privacy is better protected and feel more satisfied than in consultations with usual interpreting.
In healthcare systems today, the problems of cultural diversity seem to be perceived and taken seriously than ever before. Nevertheless, far too little research has been made on this topic. A natural tendency of most health researchers is to take on the cultural perspective of the majority ethnic group to which they belong, at the expense of the perspective of minority ethnic groups. Development of culturally competent researchers is in any case needed. Such culturally competent researchers could initiate both needed investigations as well as culturally competent practice. Because there is so little research about the effectiveness of culturally competent healthcare systems, it could not even be determined.
If ethnic and racial disparity and its ensuing consequences are to be reduced or even eliminated, healthcare systems must overcome cultural, linguistic and social barriers.
References
United Nations “global estimates” http://esa.un.org/migration
(01.) Edwards CL et al. Race, ethnicity and pain. Pain 2001, 94; 133-137
(02.) Ernst G. The myth of the “Mediterranean Syndrome”: do immigrants feel different pain? Ethnicity and Health, 2000, 5(2): 121-126
(03.) Chaturvedi N. Ethnicity as an epidemiological determinant –crudely racist or crucially important? International Journal of Epidemiology 2001, 30: 925-927
(04.) Ezenwa MO et al. Racial and ethnic disparities in pain management in the United States. Journal of Nursing Scholarship, 2006, 38:3, 225-233
(05.) Nuran Bayram, et al.; Qual. Life Res (2007) 16: 1319-1333
(06.) Emine Tuzun et al.; A comparison study of quality of life in women with fibromyalgia and miofascial pain syndrome Disability & Rehabilitation (2004) 26; 4: 198-202
(07.) Wiking et al.; J. Epidemiol. Community Health (2004) 58: 574-582
(08.) Volker Huge et al.; Impact of a functional restoration program on pain and health-related quality of life in patients with chronic LBP (2006) 7; 6: 501-508
(09.) Eliminating racial and ethnic disparities in health: overview [cited 2003 Mar 15]. http://www.raceandhealth.hhs.gov/sidebars/sbinitover.htm
(10.) Allison TR et al. Musculosceletal pain is more generalised among people from ethnic minorities than among white people in Greater Manchester. Ann Rheum Dis 2002, 61:151-156
(11.) A, Allison T. What if my back breaks? Making sense of musculosceletal pain among South Asian and African-Caribbean people in the North West of England. Journal of Psychosomatic Research 2004, 57: 79-87
(12.) Acculturation and the prevalence of pain amongst South Asian minority ethnic groups in the UK. Rheumatology 2007, 46: 1009-1014
(13.) Scott K et al. Mental-physical comorbidity in an ethnically diverse population. Social Science and Medicine 2008, 66: 1165-1173
(14.) Kavuk I et al. One-year prevalence and socio-cultural aspects of chronic headache in Turkish immigrants and German natives. Cephalalgia 2006, 26: 1177-1181
(15.) Mösko M et al. Does a Turkish Migration Background influence treatment outcome? Psychother. Psych. Med. 2008, 58: 176-182
(16.) Wittig U et al. Mental health of patients from different cultures in Germany. European Psychiatry, 2008, 23: 28-35
(17.) Taloyan M et al. Poor self-reported health and sleeping difficulties among Kurdish immigrant men in Sweden. Transcultural Psychiatry 2006, Sept., Vol. 43(3); 445-461
(18.) Hjörleifsdottir K. et al. Self-reported anxiety, sleeping problems and pain among Turkish-bron immigrants in Sweden. Ethnicity and Health 2007, Vol. 12, N 4; 363-379
(19.) Sanne GHA et al. Mood disorders and migration. Meta-analysis. British Journal of Psychiatry, 2007, 190, 6-10
(20.) Lindert J. et al. Depression, anxiety and posttraumatic stress disorders in labor migrants, asylum seekers and refugees. Psychother. Psych. Med 2008; 58: 109-122
(21.) Green CR et al. The unequal burden of pain: confronting racial and ethnic disparities in pain. Review Article. Pain Medicine 2003, Volume 4, Number 3
(22.) Bonham VL. Race, ethnicity and pain treatment: striving to understand the causes and solutions to the disparities in pain treatment. Journal of Law, Medicine & Ethics, 2001, 29: 52-68
(23.) Nguyen M et al. Access to care for chronic pain: racial and ethnic differences. The Journal of Pain 2005, Vol. 6, N 5: 301-314
(24.) Chibnall JT et al. Race differences in diagnosis and surgery for occupational low back injuries. Spine 2006 May, 31 (11): 1272-75
(25.) Pletcher MJ et al. Trends in Opioid prescribing by race/ethnicity for patients seeking care in US Emergency Departments. JAMA 2008, 299 (1): 70-78
(26.) Green CR et al. Patient attitudes regarding healthcare utilization and referral: a descriptive comparison in African- and Caucasian Americans with chronic pain. Journal of the National Medical Association 2004, Vol. 96, N 1
(27.) Schouten BC, Meeuwesen L. Cultural differences in medical communication: A review of the literature. Patient Education and Counseling 2006, 64, 21-34
(28.) Schouten BC, Meeuwesen L. Cultural diversity in patient participation: The influence of patients characteristics and doctors’ communicative behaviour 2007, 67, 214-223
(29.) van Ryn M. Research on the provider contribution to race/ethnicity disparities in medical care. Medical Care 2002, Vol. 40, Number 1, Supplement, 140-151
(30.) D.L. Roter, K.A. Cole, D.E. Kern et al., An evaluation of residency training in interviewing skills and the psychosocial domain of medical practice. J Gen Intern Med 5 (1990), pp. 347–354. Full Text via CrossRef | View Record in Scopus | Cited By in Scopus (42)
(31.) D. Roter, An exploration of health education’s responsibility for a partnership model of client-provider relations. Patient Educ Counsel 9 (1987), pp. 25–31. Article | PDF (552 K) | View Record in Scopus | Cited By in Scopus (24)
(32.) J.A. Hall, J.T. Irish, D.L. Roter et al., Gender in medical encounters: an analysis of physician and patient communication in a primary care setting. Health Psychol 13 (1994), pp. 384–392. Abstract | PDF (927 K) | Full Text via CrossRef | View Record in Scopus | Cited By in Scopus (157)
(33.) R.L. Street, V.K. Piziak, W.S. Carpenter et al., Provider-patient communication and metabolic control. Diabetes Care 16 (1993), pp. 714–721. View Record in Scopus | Cited By in Scopus (45)
(34.) D.L. Roter, J.A. Hall and N.R. Katz, Relations between physicians’ behaviors and analogue patients’ satisfaction, recall, and impressions. Med Care 25 (1987), pp. 437–451. Full Text via CrossRef | View Record in Scopus | Cited By in Scopus (128)
(35.) J.A. Hall, D.L. Roter and N.R. Katz, Meta-analysis of correlates of provider behavior in medical encounters. Med Care 26 (1988), pp. 657–675. Full Text via CrossRef | View Record in Scopus | Cited By in Scopus (413)
(36.) Roter D. Which facets of communication have strong effects on outcome—a meta-analysis. In: Stewart M, Roter D, eds. Communicating with Medical Patients. London: Sage Publications; 1989:183–196.
(37.) Beach MC et al. Cultural Competence. A systematic review of healthcare provider educational interventions; April 2005, Medical Care, Vol. 43, N4
(38.) Tucker CM. Cultural sensitivity in physician-patient relationships. Medical Care 2003, Vol. 41, N7, 859-570
(39.) Carrasquillo O. et al. Impact of language barriers on patient satisfaction in an emergency department. J Gen Intern Med 1999 Feb; 14(2): 82-7
(40.) Karliner LS et al. Do professional interpreters improve clinical care for patients with limited English proficiency? A systematic review of the literature. Health Services Research 42:2; April 2007
(41.) Baker DW et al. Interpreter use and satisfaction with interpersonal aspects of care for Spanish-speaking patients. Med Care 1998 Oct; 36(10); 1461-70
(42.) Jacobs EA et al. The impact of an enhanced interpreter service intervention on hospital costs and patient satisfaction. J Gen Intern Med, 2007, 22(Suppl 2): 306-11
(43.) Shannon C, Weaver W. The mathematical theory of communication, Urbana: University of Illinois Press, 1963 (Original work published in 1949)
(44.) Gany F et al. Patient satisfaction with different interpreting methods: a randomised controlled trial. J Gen Intern Med 22(Suppl 2):312-8
(45.) Papadopoulos I. Developing culturally competent researchers. Journal of Advanced Nursing, 37 (3), 258-2564
(46.) Anderson LM et al. Culturally competent healthcare systems. A systematic review. Am J Prev Med 2003; 24 (3S)