As Asia’s MSPs evolve, so too will Asia’s health insurance sector—and the symbiotic relationship that binds the two together. Indeed, it is not inconceivable that Asia’s large hospital chains may one day seek to enter the health insurance industry themselves.
Across Asia, governments are grappling with the serious challenges of providing adequate medical coverage against a backdrop of rising costs, inefficient healthcare insurance systems, and growing public pressure for change. In many countries poverty exacerbates the need for change, particularly in rural communities, where medical expenses not only put earnings at risk but also destroy savings. At the same time, a growing middle class throughout the region is demanding far more choice in the form of new and innovative healthcare products.
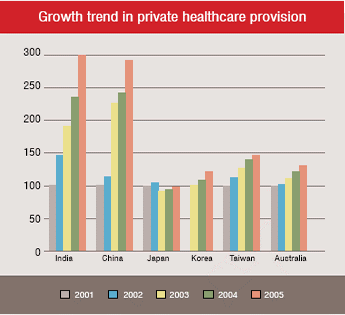 These challenges and their solutions will have a tremendous impact on Medical Service Providers (MSP), insurers and the increasingly demanding public that both serve.
These challenges and their solutions will have a tremendous impact on Medical Service Providers (MSP), insurers and the increasingly demanding public that both serve.
MSPs and insurers are bound to grow closer in coming years, working together to provide creative solutions for patients’ needs. In developed markets, insurers help provide cost-effective healthcare, covering a large range of both conventional and unconventional treatments. They also bring many benefits to hospitals, namely increased patient traffic, cashless transactions and strong support for positive regulatory outcomes. For Asia’s MSPs to enjoy the benefits such a relationship can offer, they need to adopt a proactive approach to dealing with insurers and Third Party Administrators (TPAs), who are destined to play an ever bigger role in controlling Asia’s healthcare costs, ensuring quality healthcare, and laying the foundation for sustainable growth of the healthcare industry.
China and India: Growing role of insurers
Any doubts about the radical changes underway in Asia’s healthcare sector are dispelled by examining recent history, particularly in Asia’s future economic superpowers, China and India.
In China, reform of the healthcare system is at the top of the State agenda: in March, Premier Wen Jiabao announced that the country would spend CNY10.1 billion (US$ 1.26 billion) to extend coverage of the Rural Cooperative Medical Scheme, aiming to deliver basic medical coverage to 80% of the rural population by the end of 2007. He also formed a task force to draw up plans for reforming the urban healthcare system.
Meanwhile, China’s insurance regulator is actively encouraging greater partnership between local authorities and private insurers. Its goal is a multilevel coverage system that will serve different segments of the community, using the tools and products that deliver the most appropriate healthcare coverage in the most efficient manner
In India, until recently, cooperation between the insurance and healthcare industries was minimal. In spite of this lack of cohesion, private hospitals and healthcare providers have proliferated throughout the country. While this growth made medical care accessible to many more Indians, healthcare bills drove many into debt and poverty—a situation which still exists today. In the last few years, however, insurers and medical service providers are working more closely together achieving very encouraging results.
Several major changes have driven the trend for cooperation in India, namely the introduction of TPAs for medical insurance.
 Although the hospital/TPA/insurance relationship is complex, it has led to service improvements at both hospitals and insurers, with the end result of more affordable care for patients. Cashless transactions at hospitals have risen sharply and more hospital beds are filled, boosting their profitability. Tellingly, Indian doctors and hospital administrators are increasingly becoming conversant in TPA and insurance terminology and practice, helping them make the most of their partnerships with insurers.
Although the hospital/TPA/insurance relationship is complex, it has led to service improvements at both hospitals and insurers, with the end result of more affordable care for patients. Cashless transactions at hospitals have risen sharply and more hospital beds are filled, boosting their profitability. Tellingly, Indian doctors and hospital administrators are increasingly becoming conversant in TPA and insurance terminology and practice, helping them make the most of their partnerships with insurers.
In the longer term, such partnerships will yield even greater benefits. By 2050, India is expected to be the world’s most populous nation with 1.63 billion people compared to China’s projected 1.44 billion. If just 10% of this massive population buy healthcare insurance, it will represent a customer base of 307 million people. By fostering close relationships with insurers, healthcare providers will be ensured of access to this large patient base.
Additionally, the emergence of medical tourism, with many hospital chains in Asia setting themselves up as centres of excellence, will lead to increased collaboration. Indeed, Asia's medical travel market is projected to be worth US$ 7 billion in the next five years, boosted in part by an increasingly affluent consumer in India and China alongside poor healthcare provision throughout the rest of the world.
The winds of change across Asia
Change is also underway in Asia’s other countries, as the economic realities of modern healthcare force governments to review their relationship with the population in regard to healthcare costs. In Japan and Korea, rising medical costs pose grave problems for both the countries’ national healthcare systems. In Southeast Asia, the public provision of healthcare is increasingly becoming unsustainable owing to increasing usage and expectations. In Australia, an ageing population is putting strain on a system that is already running at overcapacity. Although the solutions may differ by country, what is certain is that the relationship between healthcare insurers and MSPs will be strengthened.
Many models exist to define the role that both MSPs and insurers should play in healthcare systems. Often, this depends on the current market infrastructure, mainly the structure of the insurance industry and medical service provider network, as well as the regulatory frameworks that govern both. Experience in developed markets shows that the more advanced the infrastructure, the more interaction there is between insurers and MSPs. A robust infrastructure provides many incentives for MSPs and insurers to work together, ensuring a closer alignment of interests. Key areas for cooperation include mutually beneficial managed care and intervention programmes, guaranteed customer payments via cashless transactions, guaranteed bed capacity and cost reduction strategies.
Less cash, more cash flow
In virtually every case, this closer interaction has led to the gradual increase of advanced reimbursement models among the insurers, MSPs and insured—a great improvement over traditional fee-for-service arrangements. Such models also give doctors strong incentives to balance the needs of patients with economic realities.
The fee-for-service model, moreover, can encourage the prescription of unnecessary medications and treatments, sharply raising costs for the party least able to afford it—the patient. A more consistent focus on costs can also be of benefit to the MSPs themselves, as ultimately a strong relationship with insurers can provide the much needed quantum leap in patient traffic, which in turn boosts income needed to upgrade facilities and enable expansion.
While the changing healthcare landscape in Asia presents many challenges for medical service providers, it also presents unprecedented opportunities for growth. As Asia’s MSPs evolve, so too will Asia’s health insurance sector—and the symbiotic relationship that binds the two together. Indeed, it is not inconceivable that Asia’s large hospital chains may one day seek to enter the health insurance industry themselves. Ultimately, the changes afoot across Asia will result in more preferred provider arrangements, with hospitals and insurers playing a dual role in customising affordable solutions and designing affordable products for the most important party in the mix—the patient.